Breast cancer: how to reduce your risk
It's the disease women fear most – and new discoveries about genetic causes only make us feel more helpless. Yet there are changes we can make to help prevent it, says Jane Feinmann
The fear of breast cancer is a source of persistent anxiety for many women alongside a fatalistic feeling that, short of radical surgery, there's little if anything that can be done to reduce the risk of this frightening disease.
A report earlier this month of a newly discovered gene on chromosome 8, named NRG1, will have done little to reduce this anxiety. NRG1, a gene we all have, has been shown to act as a brake on the growth of tumours, stopping cancer cells from developing. Around one in two women with breast cancer has a damaged version of NRG1, effectively turning off the gene and thereby allowing cancer to develop.
British scientists say the breakthrough could lead to new ways of treating cancer. But, for many women, it's a further cause for concern. While genes are only responsible for a tiny percentage of breast cancers, it's worries about genetic susceptibility to breast cancer that particularly prey on women's minds.
For the increasing number of women who have a close relative diagnosed with breast cancer, there's a feeling that so many risk factors cannot be changed, with family history the number one cause for concern. But women are told they're also at greater risk if they have their first period at a younger than average age, if they are tall or thin, or if they have their first child over 30 or are childless – most of these factors beyond a woman's control.
Such pessimism is no longer appropriate, however. Here are some ways to help prevent the development of breast cancer – or at least to ensure that the disease is picked up and treated at the earliest possible moment.
Breast-feeding could save your life
There's been overwhelming evidence for some years showing that taking an "often and early" approach to motherhood reduces the breast cancer. Indeed the increase in rates of breast cancer in newly prosperous countries such as India and China is thought to be largely linked to the trend in these countries for having children later in life.
The findings on breast-feeding have been less clear-cut – until now. In September, researchers reported that breast-feeding for a minimum of three months reduces the risk of pre-menopausal breast cancer by a stunning 25 per cent – and it doesn't seem to matter if formula milk is also used and if the three months is spread over more than one infant.
The findings, reported in the Archives of Internal Medicine, were the result of eight years of monitoring more than 60,000 women who had been recruited in the Nurses' Health Study in the US. The research team found that breast-feeding provided the greatest protection for women who had one or more close family member diagnosed with breast cancer – among this group, those who breast-fed had a 59 per cent reduced risk.
"This reduction in risk is comparable to that found in high-risk women who take hormonal treatments such as tamoxifen," said lead researcher, Dr Alison Stuebe of the University of North Carolina. "While family history is not modifiable, this is truly an action women can take to reduce their breast cancer risk."
Eat a low-fat diet– and get your daughters on the same regime
Women who eat a low-fat diet have lower levels of female hormones in their blood – and this reduces the risk of breast cancer, especially in the years after the menopause when body fat is the richest source of oestrogen. There is also some evidence that the earlier you start, the greater the impact. Research suggests that a low-fat diet in the teenage years has a major impact in establishing low levels of oestrogen in the blood levels and thus reducing the risk of breast cancer in adulthood. An ongoing study, however, is investigating the safety of encouraging a low-fat diet in teenagers, particularly with regard to the impact on the developing skeleton and the possible risk of osteoporosis.
Get sun-soaked
It's well known that breast cancer is most common in areas of the world that get the least sun. The reason seems to be that there's a correlation between breast cancer and low levels of vitamin D, which the body makes in response to the ultraviolet B rays of the sun, according to Canadian research. The study tested levels of the sunshine vitamin in 512 women with breast cancer and found that, over the following six years, those with the lowest levels were most likely to suffer a recurrence of the disease or to die of it. Laboratory and animal studies suggest that vitamin D may actually prevent breast cancer developing by curbing the growth both of abnormal cells and the blood vessels that feed tumours. Nutritional expert Dr Andrew Weil recommends that anyone at risk of vitamin D deficiency should take 1,000mg daily supplement of vitamin D3, the most easily absorbed type. "It isn't easy to get enough D from your diet," he says – though the best sources are fortified milk and cereals, eggs, salmon, tuna, mackerel and sardines.
Take regular exercise throughout your life
Everyone needs to exercise – but it's particularly important for those at high risk of breast cancer. Recent research showed a reduction in the risk of pre-menopausal breast cancer in women who spent a minimum of three hours a week exercising from their teenage years onwards. And, once you're past the menopause, the importance of exercise becomes even more crucial. Post-menopausal women who are overweight and exercising are at lower risk than those who are overweight and not exercising. Those who are a healthy weight and exercising are at lower risk than women who are a healthy weight but not exercising.
Be assertive with your GP
It's not that there's a link between standing up for yourself and getting breast cancer. But new evidence shows that four out of 10 people put off seeing their GP when they fear they have cancer symptoms. And this peculiarly British trait is a key factor in the persistent late diagnosis of cancer in this country compared to the best-performing European nations, according to Cancer Research UK. It claims that picking up cancer earlier could prevent 11,000 deaths every year if we matched other European nations. "When British etiquette stops us talking to the GP about potentially serious symptoms, it can be dangerous," warns Professor Jane Wardle of University College, London.
Know your family history
Eligibility for a mammogram, currently based on age and offered only to women between 50 and 69, could soon be based on a woman's genetic risk of developing breast cancer instead, experts predict. For a start, a simple mouth swab, currently under development, will make testing much easier. And scientists at Cambridge University have recently reported the discovery of a number of new genes, each of which individually has a modest impact on the risk of breast cancer – but which, in combination, can hand a woman "a bad hand of cards" genetically.
As more of these low-risk genes are identified over the next few years, it will make sense, scientists say, for women to get the test in their early 30s. Those at high risk of developing breast cancer could then be given access to regular mammograms, while older women at low risk could choose not to have mammography.
The researchers still have to prove that "these combination genes raise the risk of breast cancer in the real world, and that's a few years away", says Professor Sir Bruce Ponder of Cancer Research UK's Cambridge Research Institute. Until then, it's worth getting to know your family history in order to be alert to early signs of cancer. The red flags are women with a relative on either side of the family who have had pre-menopausal breast cancer, bilateral breast cancer (cancer that appears in both breasts) or ovarian cancer.
Avoid drinking to excess
According to Cancer Research UK, drinking raises the risk of developing breast cancer – but only minimally, unless you're consuming seriously unhealthy amounts of booze. In a review of the evidence published in June, it says that, by the age of 80, the number of women who will develop breast cancer will be 8.8 out of 100 if they don't drink at all, 10.1 if they have two drinks a day, and 13.3 if they have six drinks a day
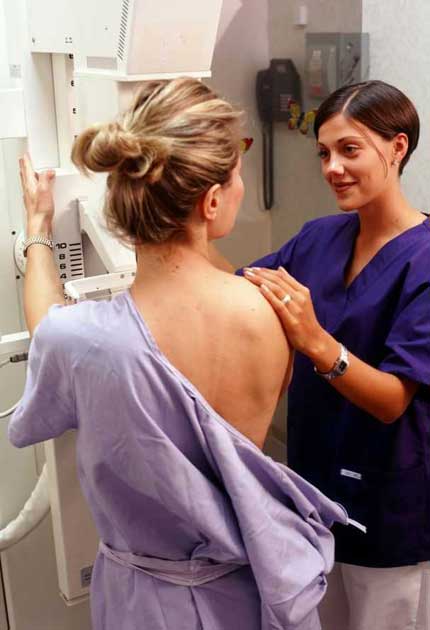
Have regular mammograms
There are experts who claim that having a mammogram puts you at an increased risk of over-diagnosis and unnecessary treatment and therefore is not worthwhile. Most experts, however, say that one set of statistics should be your guide: mammography has so far detected 117,000 cancers, saving around 1,250 lives every year and bringing a 35 per cent reduction in mortality in the 50 to 69 year age group. It's definitely worth being in that group even if it means having a somewhat unpleasant test every three years – and the good news is that a blood test which detects a breast-cancer fingerprint long before a tumour has started to grow could replace the mammogram within years. It's also worth bearing in mind that a positive mammogram is only the first step in a diagnostic procedure that involves a number of checks and tests before treatment is considered.
Subscribe to Independent Premium to bookmark this article
Want to bookmark your favourite articles and stories to read or reference later? Start your Independent Premium subscription today.

Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies