New doctors on the wards: A matter of life and death
Every year in Britain's hospitals comes Black Wednesday, when junior doctors take charge for the first time - and death rates rise by 6 per cent. So how did it feel to be one of this year's rookies?
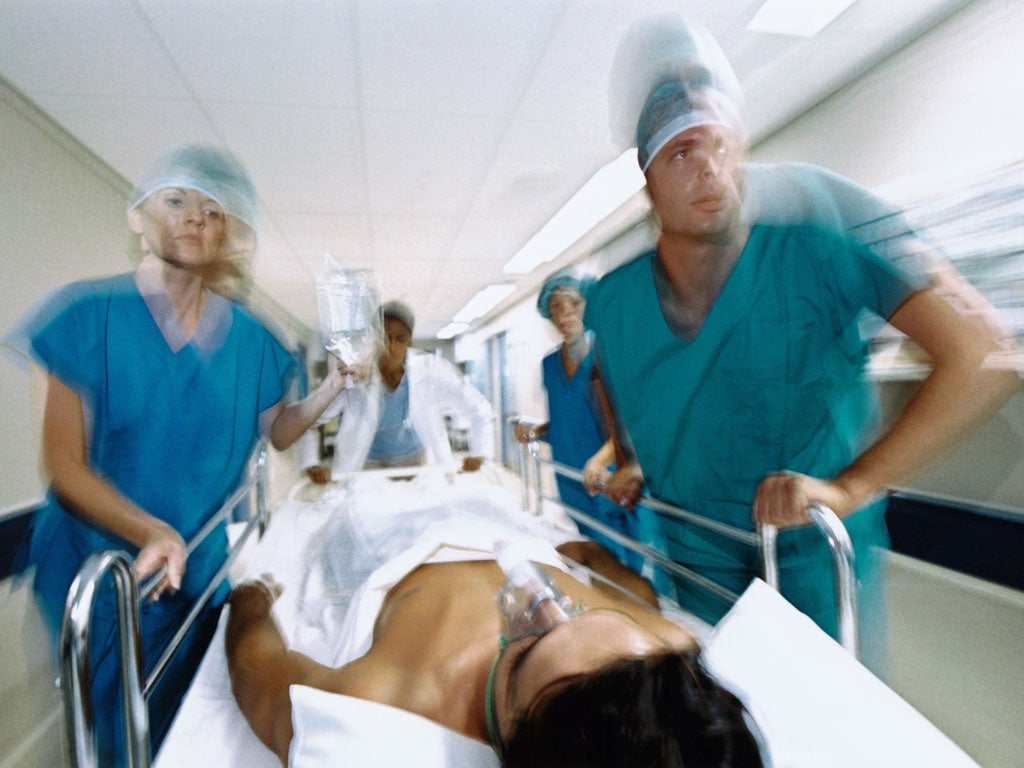
A male first-year doctor, aged 24, working in Liverpool
Most junior doctors would admit they have mixed feelings about their first day – a combination of excitement, nervousness, and a sense that loss of liberty is fast approaching.
The stress is exacerbated by the fact that many doctors move to a different city to take up the post, meaning they have to contend with a new hospital, new faces and a hunt for accommodation while preparing for their first day flying solo. The primary objective is not to harm anyone.
Like most of my peers, I arrived very early on my first morning – surgeons are notorious for starting early. As one once said to me when I turned up for a ward round at 9am, "I have my lunch at 9 o'clock!"
I brought a few props – mostly medical handbooks – along for comfort but knew in reality that I'd never have time to consult them. The first ward round was a steep learning curve. I'd been on hundreds as a student but it's different when you're trying to deal with patient notes and compile a list of tasks for the day when instructions are being barked out faster than they can be written down.
After the ward round I collected my bleep. It would be hard to find a first-year doctor who wasn't at least a little excited at being given their bleep and the associated responsibility. The novelty wore off quickly though as the beeper went off constantly, providing a rich supply of tasks that even the most efficient doctor might struggle to get through in a shift. And the novelty was completely gone for me at 3.30am when I was asleep after my first day; I had forgotten to switch it off and was woken by an urgent call for the medical emergency team. A mistake I'll make only once.
The most disconcerting thing about my "Black Wednesday" was not knowing what I was meant to be doing at a particular time, as I was without direct supervision. When I started medical school I imagined that working as a doctor would be non-stop drama running around with a defibrillator. Little did I know that the bulk of my day would be spent as essentially a "desk jockey", prescribing medicines and writing discharge letters. Nothing really prepares you for writing your first prescription when you're doing it for real with the potential to harm a patient. I checked and rechecked the British National Formulary, asked advice from my colleagues and the ward pharmacist and re-read the patient's notes before signing that first script.
Five minutes before the end of my first shift the staff nurse came into the office and asked me to review a patient becoming increasingly unwell. The man was having a complication of a surgical procedure performed five days earlier so I immediately called the consultant, who after he arrived said on several occasions, "I'm not happy… I am not happy about this." My heart sank, as I thought he was referring to management of the patient, but I later discovered he was talking about the patient's condition.
Under pressure, with the consultant standing over me, I had to take an arterial blood gas sample – no simple task. Thankfully I got it first time and somehow managed to impress the consultant and redeem myself a little. The day ended rather dramatically with me sprinting to the lab with the sample as the analyser in the A&E department was broken. The patient's life was saved later in surgery.
My shift ended three hours later than planned, confirming to me that, in medicine, "home time" is an aspiration rather than a reality. And the same goes for lunch breaks – for the last few days I've been surviving on Mini Cheddars and chocolates lying around our office.
An aspect of starting work I was concerned about was my relationships with colleagues. Without the support of nursing staff I wouldn't have made it through the first couple of days, but I do feel slightly uncomfortable when asking a nurse to do something. Ordering around people who are vastly more experienced and skilled than me doesn't come naturally.
Despite all of these challenges, the job really is a great privilege. While we are the most junior of the medical staff often bearing a disproportionate level of responsibility, we have a fabulous job because we're arguably closest to the patients, most of whom I've gotten to know very well in the space of two days. Already, I can see that being an F1 helps you put whatever problems you have at work or outside it in perspective. Seeing a patient recovering from a serious nerve disorder celebrate the fact she managed to walk 14 steps to the toilet, or a man delighted he can taste food for the first time in months, or even something simple like children coming to visit their grandfather for the first time in weeks, is what it's all about.
First-year doctor, aged 24, working in the South East
I am on a coronary care ward. A couple of patients have gone into cardiac arrest and we have had to call the crash team. One woman had so many things wrong with her I was trying to think through the implications of each problem and how you would treat it. The trouble was the treatment for one problem – giving a drug for her heart – would cause problems for her kidneys, which were already failing. It was mind boggling.
It has been quite a transition from medical school. I have found it a lot more stressful than I thought. I was covering the ward on my own and at one point in the afternoon people were throwing more jobs at me than I could cope with. I was writing discharge letters, making referrals, prescribing fluids – and trying to cover the ward.
As a first-year doctor, you are not so much a medic as a well-paid administrator – you spend your day on the phone, writing notes, organising beds and carrying out the tasks that make the ward run. My scariest moment was dealing with one of the patients who had a cardiac arrest. I was the first doctor on the scene, with the nurses, and made sure they were inserting cannulas and carrying out the necessary tasks. I did chest compressions for about 30 seconds – it is physically exhausting, so you swap around. The patient did come round but unfortunately he died later.
I had attended cardiac arrests before but as a student any contribution you make is a bonus. When it's your patient, it is another matter. You have to make the decisions about what treatments to give, what interventions to perform.
I had only the met the patient briefly in the morning so had not got to know him. When patients have been on the ward a long time and you lose them it is more difficult – it does get to you. You have to learn to deal with it. When you go home, you have to try and get on with the rest of your life.
Female first year doctor, aged 22, from Kent
I am on a medical ward with elderly patients. Most are stable but sometimes things start to go wrong.
My scariest moment was being called by the nurses to see a patient who was unwell – his heart was racing and his breathing rate had increased. When the nurses come and expect something from you, that is pressure.
It is a matter of going through the basics systematically – taking the pulse, listening to the lungs, taking blood. Checking there are no obvious abnormalities. Then I spoke to a senior doctor.
Usually people come in to this ward with a series of problems. We try to stabilise them and then provide support till they can get home.
As a medical student, you are asked to do things. Here, no one tells you what to do. You have to come up with a plan yourself. Getting on well with the nurses is really important. It is the first lesson you need to learn – they know better than the doctors how things work on the ward.
Subscribe to Independent Premium to bookmark this article
Want to bookmark your favourite articles and stories to read or reference later? Start your Independent Premium subscription today.

Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies