Cancer to cause 'crisis of unmanageable proportions' for NHS as survival rate soars
With 2.5 million Britons now living with side effects of the disease, charity warns of increasing demand for services
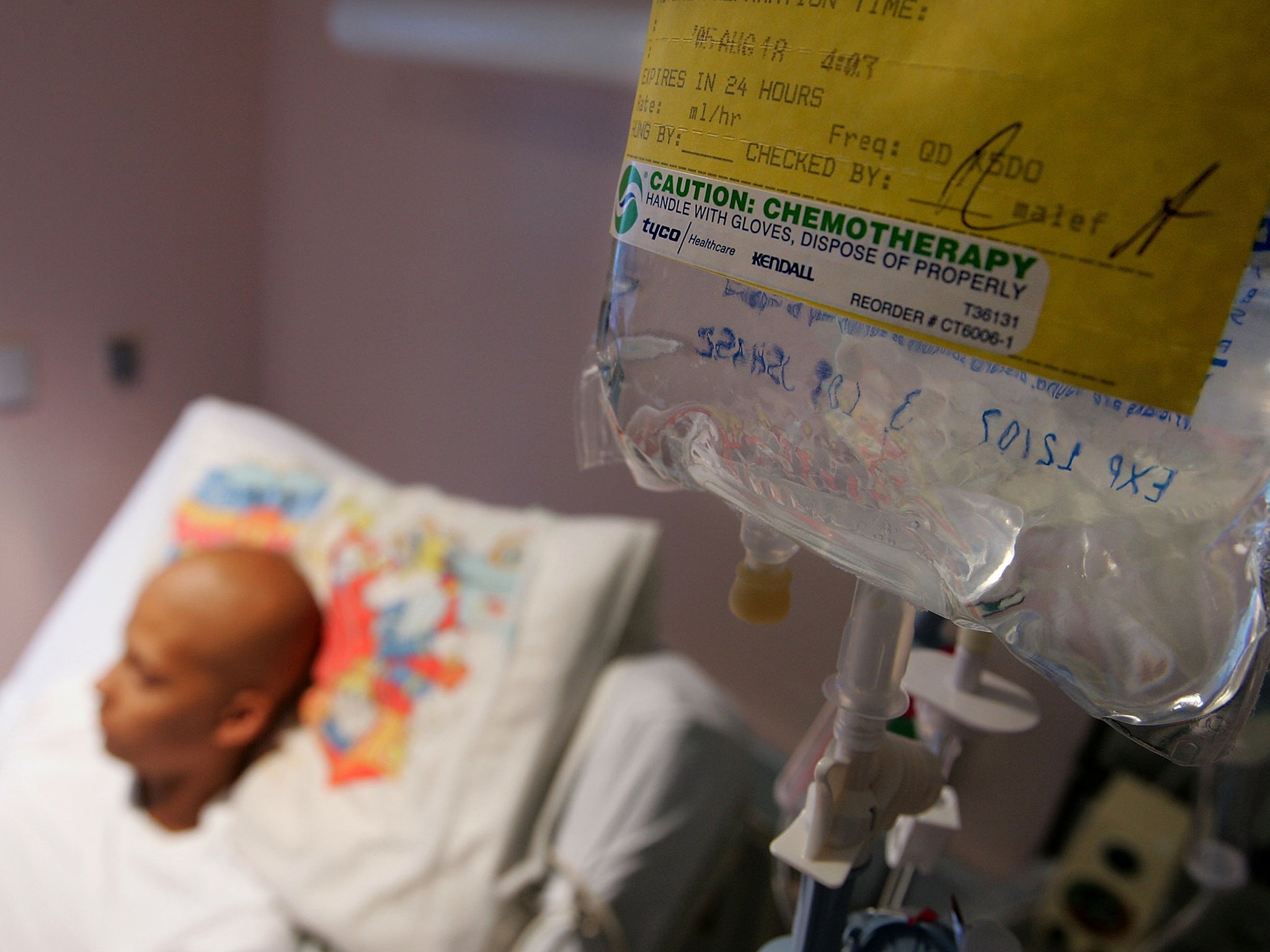
A record 2.5 million people are now living with cancer or the after-effects of it, threatening “a crisis of unmanageable proportions” for the NHS, a leading charity has warned.
Macmillan Cancer Support said improving survival rates had created a growing number of people who had not returned to full health because of serious side effects.
Better detection of cancers and the increasing success of treatments have led to half of cancer patients today expected to survive the disease.
But Macmillan said the long-term burden of side effects would put “huge pressure” on the NHS, and called for political parties to commit to “urgent action” on cancer care in their manifestos
Around one in four people face ill health or disability following treatment for cancer.
Lynda Thomas, chief executive of Macmillan, said that improvements in survival rates were “great news”, but warned that progress had been “a double-edged sword”.
“As numbers surge, the NHS will soon be unable to cope with the huge increase in demand for health services and the support that organisations like Macmillan provide will become even more urgent and important,” she said.
Among the over 65s, the number living with cancer has gone up 23 per cent in five years, Macmillan said. Big rises have been seen in prostate cancer rates, up 27 per cent in five years, while the number living with breast cancer has gone up 21 per cent in the same period.
Macmillan said that all parties should commit to delivering survival rates that match the best in Europe, and invest in delivering “recovery packages” to all cancer survivors that addressed their long-term health needs.
Fran Woodard, the charity’s director of policy and research, said that recovery packages should include an assessment of a patient’s psychological and physical requirements, and if they needed financial support.
GPs should also be given full summaries of a patient’s treatment and should carry out a review six months after completing treatment, she said.
“Macmillan believes that everyone should have health and social care at the time they need it… because it leads to better outcomes,” she said.
Election manifestos should include plans to ensure patients are treated with dignity and respect, and end of life care is guaranteed by free social care for the terminally ill, the charity said.
Survival rates for different types of cancer vary. Nearly 80 per cent now survive for 10 years after a breast cancer diagnosis, up from 40 per cent in 1970. Testicular cancer patients have a 98 per cent chance of surviving for 10 years, and people with malignant melanoma have an 89 per cent chance.
However, only one per cent of those with pancreatic cancer will survive 10 years, and only 5 per cent of lung cancer patients. Lung cancer remains the biggest cancer killer, accounting for 22 per cent of the 160,000 cancer deaths in the UK every year. Oesophageal cancer and brain tumours also have poor survival rates.
Macmillan said that keeping people informed about symptoms, ensuring GPs were vigilant, and improving waiting times for NHS treatment would improve survival rates.
Sean Duffy, national clinical director for cancer at NHS England, said: “We are diagnosing and treating more people with cancer than ever before, and as result more people than ever are surviving. We need to take action on three fronts: better prevention, swifter access to diagnosis and better treatment and care for all. If we get this right it will help to address the pressures we’re facing.”
Case study: John Pearson
John Pearson, 47, from Kent, was diagnosed with bowel cancer in 2006, aged 39. In remission since 2011, he still suffers from serious nerve damage, a side-effect of his chemotherapy.
I had to go in for surgery very quickly to have most of my bowel removed, which is debilitating in itself.
Then I had a very severe reaction to the chemotherapy, with massive spasms in my chest that would stop me from breathing, I never experienced such excruciating pain.
That went on for six months. Chemotherapy is such an intense time. Then you get to the end and are told: ‘Off you go.’
I was left with peripheral neuropathy, which is a side-effect from the drug and affects all the nerves in the outer extremities of your body. You have nerve pain, particularly in the hands and feet.
With that, the fatigue and the effects of having most of my bowel removed, I was finding it difficult to get back to work and 18 months after my diagnosis, I had to retire from my job in the Sainsbury’s business centre. I just did not have the energy levels required to do the job.
Now, I go for colonoscopies every two years, get a pain relief prescription from the GP every month, see my neurologist at Guy’s Hospital once a year, and pay to see a private physio, who is also an osteopath and acupuncturist.
Only at the weekend I took the dog out and was in a huge amount of pain because it was cold out, which exacerbates the nerve damage.
I could sit indoors like a hermit all day – but then you’d ask the question, what was the point of surviving it? You’ve got to get on with life.
Subscribe to Independent Premium to bookmark this article
Want to bookmark your favourite articles and stories to read or reference later? Start your Independent Premium subscription today.

Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies