The cancer equation: Mathematically modelling the cure
A group of scientists hopes to tame the chaos of cancer in a bold new way – by using maths. Does this approach add up?
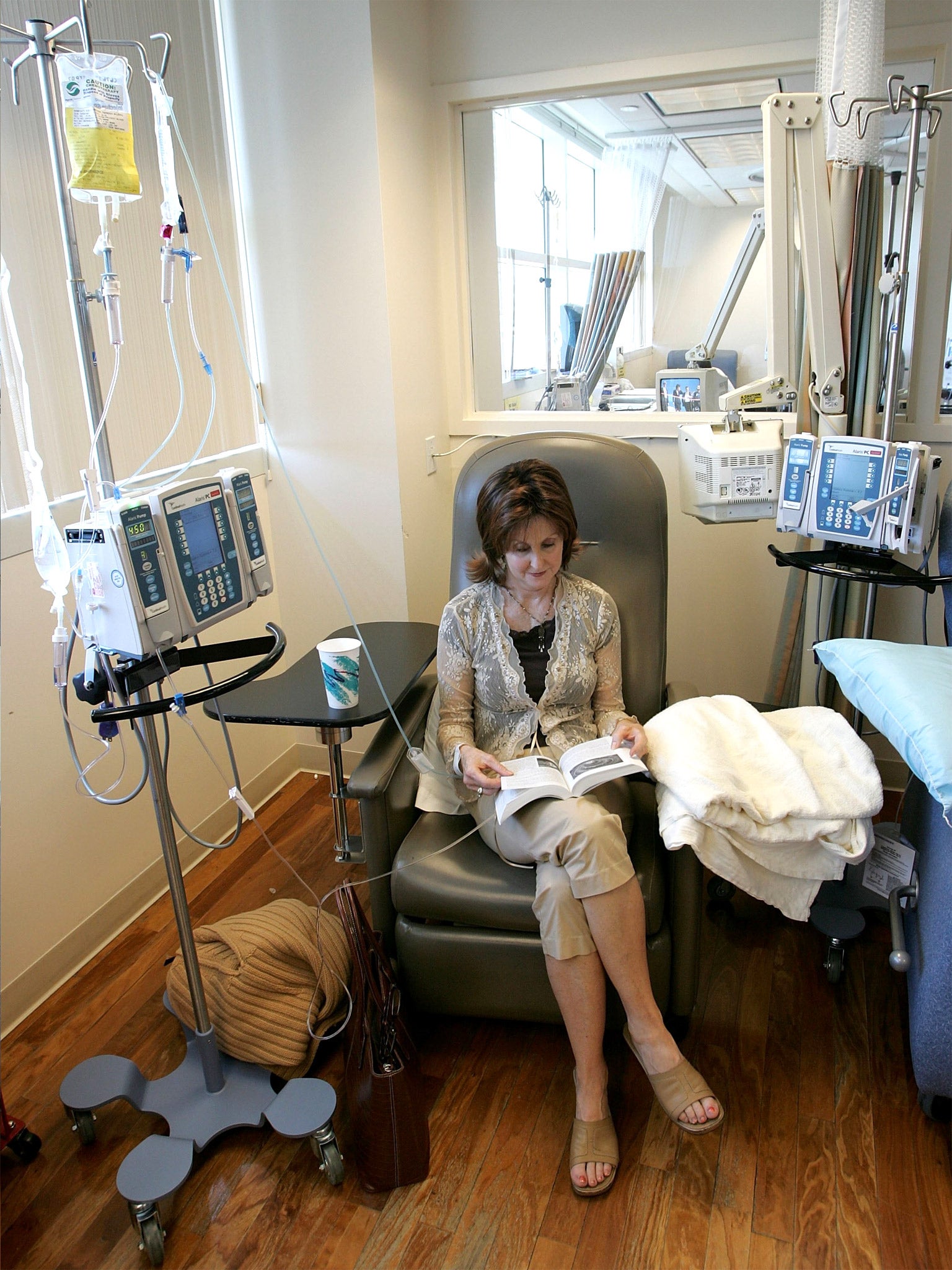
From his fourth-floor window at Tampa’s Moffitt Cancer Center, Robert A Gatenby can look down to where patients stand waiting for valets to retrieve their cars. They have gone through chemotherapy, biopsies, radiation. They are pale, anxious, resolute. Some will live and some will die: a young woman with short hair, clutching her partner’s hand; an older man, alone.
Gatenby says he sometimes sees patients retching after chemotherapy, which reminds the 62-year-old radiologist that his Integrated Mathematical Oncology Department – the only full-scale outfit of its kind in the US – does not have the luxury of time. Mathematics is not generally known for urgency. Few lives hinge on proof of the twin prime conjecture, but the mathematicians and oncologists that Gatenby has assembled in Tampa are trying to tame the chaos of cancer in part through the same differential equations that have tortured so many generations of calculus students. By mathematically modelling cancer, they hope to solve it, to make its movements as predictable as those of a hurricane. The patients down there, fresh from treatment, need shelter from the storm.
Gatenby’s small corner of Moffitt bears little resemblance to a medical centre: there are no white-coated doctors rushing to save patients or synthesising miracle cures deep into the night. You might think you’ve found yourself in a sleepy academic department, where abstract ideas are kicked around like a football on a school playing field.
Which is a pretty accurate description of what goes on in Gatenby’s lab, though not at all a pejorative one. The mathematicians in his employ are convinced that we do not really understand cancer and that, until we do, our finest efforts will be tantamount to swinging swords in utter darkness.
We have been fighting the War on Cancer since 1971, when President Richard M Nixon declared that the “time has come in America when the same kind of concentrated effort that split the atom and took man to the moon should be turned toward conquering this dread disease”. Four decades later, 1,665,540 Americans per year hear the dreaded diagnosis, and about 585,720 die annually from some variety of the disease, according to the American Cancer Society. Modern oncology makes incremental advances, with a melanoma drug that extends survival by three months passing for a major breakthrough.
Gatenby is tired of a fight we keep losing. After 30 years, he has come to the uneasy conclusion that cancer is cleverer than we are, and will find ways to evade our finest medical weaponry. The weary warrior wants to make peace with cancer’s insurgent cells – though on his own terms; terms that would spare the lives of many more patients. To some within the medical establishment, this might seem preposterous, but Gatenby relishes the role of the outsider.
He grew up in Pennsylvania, where 12 years of Catholic school instilled in him “an incredible hatred of dogma”. At Princeton University, he studied physics with some of the greatest scientific minds of the 20th century. Figuring he wasn’t fated to join the physics pantheon, Gatenby turned to medicine. But medical school at the University of Pennsylvania was dismayingly similar “to the rote learning of catechism” he remembered from school. It felt like he was “going backwards”.
Gatenby specialised in radiology and, after receiving his medical degree in 1977 and completing a residency, went to work in 1981 for the Fox Chase Cancer Center in Philadelphia. It was home to David A Hungerford, one of two researchers responsible for discovering the Philadelphia Chromosome, a major clue to cancer’s birth within the human genome.
Among its current éminences grises is Alfred G Knudson Jr, whose “two-hit” hypothesis holds that cancer is triggered by an unfortunate accumulation of errant genes, harmful outside events (too much sun, too much red meat) or a combination of the two.
The study of genes did not interest Gatenby then, nor does it interest him now, even though much of medicine is now in the thrall of genomics. Gatenby wanted to discover cancer’s “first principles”, the basic ideas behind the seemingly sudden explosion of cells that want to kill the very body that nourishes them. He sought to understand cancer with the same totality that Newton had understood gravity.
As with Newton’s laws of motion, mathematics seemed to hold the key. Maths had been used to model the weather and financial markets which, like the human body, are fickle and incredibly sensitive to outside forces. Gatenby saw no reason why the same could not hold true for cancer. He spent a year reading maths, which puzzled his colleagues. Then, he took a sheet of stationery and started scratching down equations he thought could get him closer to cancer’s fundamental truths.
“To say they hated it would not do justice,” Gatenby says of the response of his Fox Chase colleagues. Other oncologists told him that “maths modelling is for people too lazy to do the experiment”, and that “cancer is too complicated to model”. The latter is a refrain that, 30 years later, still dogs Gatenby and his staff at the Integrated Mathematical Oncology Department, which includes five mathematicians with no formal experience in medicine.
Among those is Sandy Anderson, a young Scotsman who dresses as if he were on the way to a Beck concert. There is a bottle of single malt on his desk. “Of course, cancer is complex,” Anderson tells me. “But how can you say it’s too complex? That complexity should be viewed as a challenge that we have to try and tackle. And just because there’s complexity doesn’t mean there aren’t simple rules underlying it.

“What we’d love to do is have everybody’s own little hurricane model for their cancer,” he explains. This is less a metaphor than you may imagine. Anderson shows me computer models of a breast cancer’s growth, the cells spreading like a malicious green cloud across the screen. Different versions of the model show what happens when different treatments are applied: sometimes the cancer slows, but sometimes it explodes. This seems like an intuitively rational approach to the disease, predicting how it responds to a variety of treatments. But it isn’t common. There are about a dozen drugs for breast cancer approved by the Food and Drug Administration. Depending on which form of the disease is diagnosed and at what stage it’s discovered, there’s a maddening number of viable drug combinations. Best practices exist, but these can be anecdotal, doctors simply doing what they think works. The war on cancer is fought by competing bands with their own weapons, cancer’s chaos exacerbated by our own dismaying disorder. Anderson would like to provide the onco-soldiers with battlefield maps.
Weather often came up during my time in Tampa. In 1961, Edward N Lorenz of the Massachusetts Institute of Technology tried to create computer models for weather, only to stumble into the field of chaos theory. He saw that weather was entirely dependent on initial conditions, so that if he altered his inputs by even a fraction of a percentage, the weather model would fluctuate to an unexpected degree, in unexpected directions. Yet patterns did emerge. This would come to be called “deterministic chaos”, for the way that complex adaptive systems – the weather, the global economy, maybe cancer – can both hew to our expectations and routinely subvert them. Sometimes, autumn acts like autumn. But once in a while, in Lorenz’s famous formulation, a butterfly causes a hurricane.
One refrain I heard several times at Moffitt was that “all models are wrong, but some are useful”, a quip by the late mathematician George EP Box. A mouse injected with melanoma is only an imperfect model of human cancer; if it weren’t, you wouldn’t be reading this article today, for, as Anderson acidly notes: “We’ve solved cancer in mice a hundred thousand times.” This is a model, too: [insert the complex equation here]
If that freaks you out, don’t worry – it freaks out a lot of clinicians. Gatenby and his team are doing the maths for them, convinced that their models of cancer strike the right balance between specificity and universality.
The other option is to keep chasing errant genes and trying to snuff them out, but that seems to many like a futile enterprise, like trying to plug a leaking dam with wads of cotton. A tumour that weighs just 10 grams, Gatenby says, contains more cells than there are humans on earth. Nor are those cells a uniform gray mass, as the popular conception of cancer has it. As the tumour grows, different mutations may come to the fore. The cells of a single cancer differ within a single patient and the same types of cancers differ from patient to patient.
“It’s almost like it’s an intelligent opponent,” says Donald A Berry, who heads the biostatistics department at the MD Anderson Cancer Center in Houston. “It has many, many paths that it can take.” Mathematics, Berry says, can “provide answers where biology runs into a wall”.
One of those walls is the sheer amount of information that cancer researchers would need to map every genetic mutation possible for the 200 cancers that can ravage the human body. Researchers have spent $375m to create the Cancer Genome Atlas, which is based on the screening of 10,000 cancer samples for the responsible genes. Some think that until we’ve sorted through about 100,000 samples, the cancer gene compendium will be woefully incomplete. “It would be crazy not to have the information,” the geneticist Eric S Lander told the New York Times.
But information brings its own delusions. Gatenby laments the “vast industry that’s developed over molecular data”. He is frustrated by the narrow focus of many of his colleagues. The bookshelves in his office don’t hold the standard medical tomes; they are lined with rare physics texts from the early 20th century, including several volumes of the Annalen der Physik, which published the pioneering work of Einstein, Hertz and Planck.
Gatenby knows that all his equations will mean nothing if they don’t help patients. Ultimately, he will have to convince the very clinicians who frustrate him that his abstractions can have real-world benefits. In 2000, Gatenby went to the University of Arizona and was named the head of radiology at its College of Medicine in 2005. It was here in the desert of Tucson that he had an intellectual conversion. He began to understand the role that evolution plays in carcinogenesis. The first principles of cancer that he had been trying to find, Gatenby surmised, lay in the Darwinian concept of natural selection.
His insight was brilliantly counterintuitive: cancer is really, really good at evolution. So good that our bodies nourish it, even as it hijacks blood vessels and nutrients. It fools the immune system, nestling so deep within normal tissue that we can’t easily extract it. And then, in what amounts to suicide, it kills the very body in which it has taken root. Maths could provide a map of cancer’s movements; Gatenby understood that only Darwin could explain why that movement was so hard to arrest. We were unwittingly helping that evolution along, turning all too many cancers into hurricanes. Worst of all, we were doing it in the name of saving lives.
The war on cancer sold the public (and much of the medical establishment) on the idea that cancers must be vanquished, that no stalemate was possible. Thus the rounds of chemo a patient faces today, killing good cells with the bad. Treatment, in other words, may aggravate a cancer’s growth by stripping away easy-to-kill cells and leaving behind hardened carcinogenic warriors.
“Evolution will win this game,” Gatenby tells me. Malignant cells will eventually evolve beyond the capacity of any drug to hold them at bay. The question is whether a mathematical understanding of how cancer progresses can lead to treatments that are less prone to aggravating resistant cells into proliferation.
Some oncologists are sceptical of Gatenby’s approach. Robert Weinberg, the MIT cancer researcher who discovered the first cancer-causing gene, does not believe mathematical oncology is a fruitful pathway because it “lacks predictive powers that extend beyond predictions made from simple, intuitive assessments of future behaviour”, as he told me in an email.
Others say that while Gatenby’s evolutionary portrait of cancer is a clever analogy, it is not instructive for treatment of the disease.
Marc B Garnick, a urologic cancer specialist at the Beth Israel Deaconess Medical Center and Harvard Medical School, says Gatenby’s ideas mirror the practice of metronomic therapy, which “has been around for decades”. Gatenby disputes this claim.
But for clinicians frustrated with the current pace of progress in the war on cancer, Gatenby at the very least offers a new way of thinking about a disease that has perplexed humanity for thousands of years.
In Tampa, Gatenby and I went to dinner at a Cajun restaurant with Anderson and Silva, two of Moffitt’s mathematicians. Downing his first drink, Anderson indicated his distaste for most of what passes for oncology today: “We keep measuring shitt without getting anything out of it.” Everyone laughed.
“I’ve never seen a dogma I didn’t hate,” Gatenby says. That was true at the Catholic school in Pennsylvania. And it is true today, at the hospital in Florida, where the cancer patients are waiting.
A version of this article appeared in ‘Newsweek’
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments