Cancer: Low doses of chemotherapy 'may control disease more effectively'
Study suggests conventional approach of using high doses in the hope of killing all cancer cells may be counterproductive
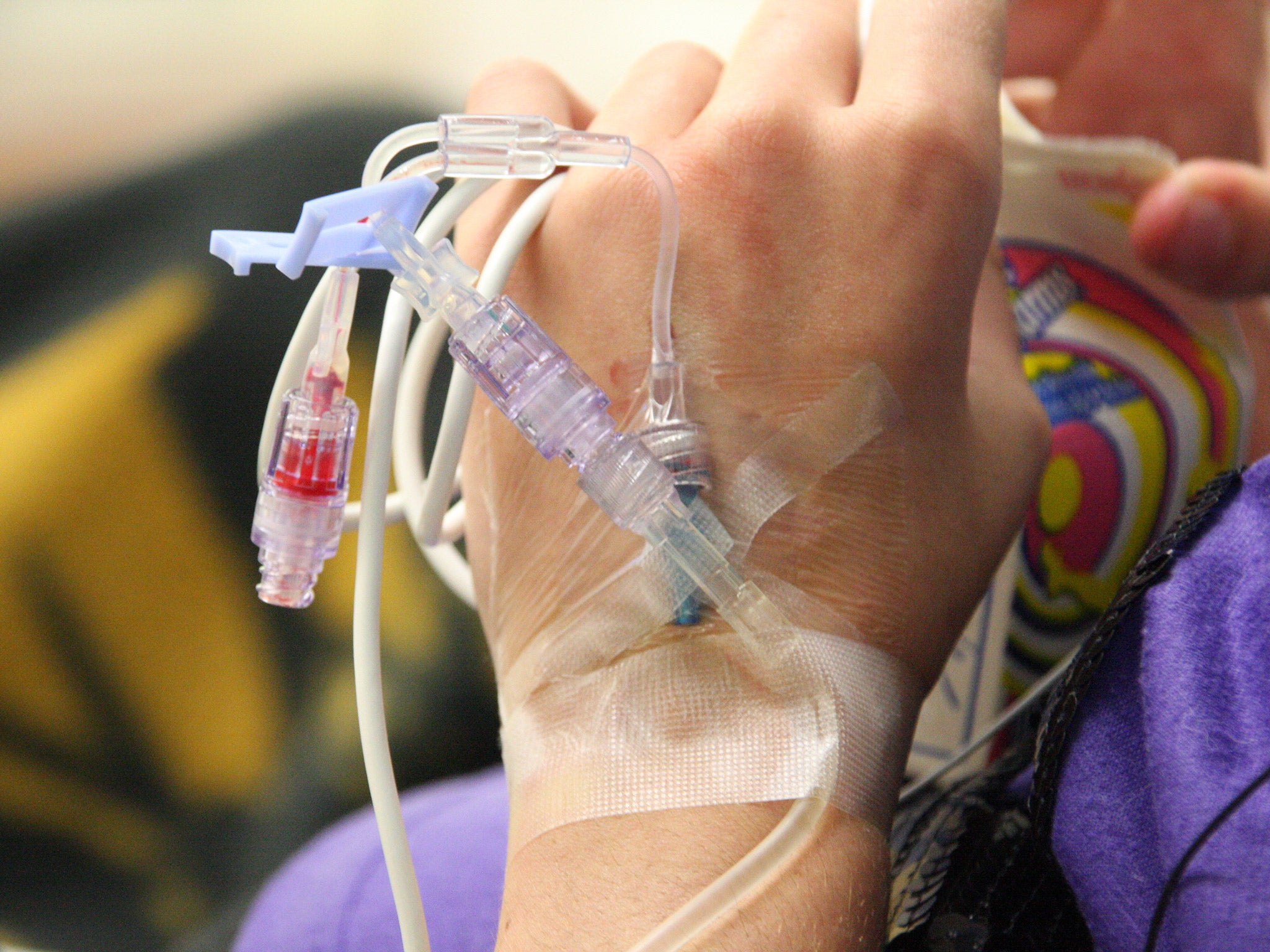
Cancer might be better controlled by administering low-doses of chemotherapy drugs rather than using toxically high doses that damage the body but still allow drug-resistant tumour cells to spread, a study has suggested.
An experiment on mice with breast cancer has shown that the conventional approach to cancer treatment, where high doses are used in the hope of killing off all cancer cells, may be counterproductive in terms of long-term survival.
The study found that aggressive treatment produces the best short-term results but is more likely to result in the return of the cancer compared to using lower doses that also result in fewer side-effects, scientists said.
Current cancer treatments often involve aggressive treatment with high doses chemotherapy in an attempt to wipe out as many tumour cells as possible with ultimate aim of a cure.
But complete eradication of metastatic cancer is rare, and the toxic side effects of chemotherapy can be highly destructive - not only leading to hair loss, nausea and extreme fatigue, but also crippling the body's immune system or triggering anaemia.
Some scientists believe that this conventional treatment allows drug-resistant cancer cells to survive the treatment and with no other cancer cells to compete with they can quickly replicate and return as a far more aggressive form of cancer.
The new approach, known as adaptive therapy, allows non-aggressive tumour cells to survive and they compete with the drug-resistant cells, so preventing the return of a far more dangerous disease, scientists said.

“The study is meant to question the conventional paradigm that has prevailed in cancer therapy for over 50 years – namely, that the best patient benefit is achieved by delivering drugs at the highest possible doses even when mortality of the treatment can reach 5 per cent,” said Robert Gatenby of the H Lee Moffitt Cancer Centre and Research Institute in Tampa, Florida.
“We propose that by eliminating all of the sensitive cells and leaving only the resistant cells behind, this approach actually results in the most rapid possible tumour progression. So, we use an adaptive therapy approach that uses smaller doses with the deliberate goal of leaving behind a population of cells that are still sensitive,” Dr Gatenby said.
Standard chemotherapy initially shrank the mouse tumours, but as soon as the treatment stopped they grew back – as monitored by MRI scans. Skipping doses whenever the tumour shrank was also ineffective and also resulted in eventual cancer progression.
Adaptive therapy - a high initial dose followed by progressively lower doses as the tumour responded - was much better at controlling cancer growth.
In fact the treatment was so effective that between 60 per cent and 80 per cent of the mice could be weaned off the drug completely over an extended period of time without suffering relapses, the study found
“When therapy is withdrawn the sensitive cells, which do not have the cost of resistance, have an advantage and suppress the growth of the resistant cells. This allows long-term control of the tumour using progressively smaller doses of drugs,” Dr Gatenby said.
“We think that patients will benefit from this approach because of the lower doses, improved quality of life and prolonged survival. In fact, the first clinical trial using adaptive therapy is now under way at Moffitt,” he said.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks