MS drug trial 'a fiasco' – and NHS paid for it
The most expensive publicly funded drug trial in history is condemned today as a "fiasco" which has wasted hundreds of millions of NHS cash and raised fresh concerns about the influence of the pharmaceutical industry.
The scheme involved four drugs for multiple sclerosis launched in the 1990s which were hailed as the first treatment to delay progression of the disabling neurological condition that affects 80,000 people in the UK.
It was set up in 2002 after the National Institute for Clinical Excellence (Nice) unexpectedly ruled that the drugs were not cost effective and should not be used on the NHS. To head off opposition from patient groups and the pharmaceutical industry, the Department of Health established the largest NHS "patient access scheme", to provide patients with the drugs, costing an average £8,000 a year, on the understanding that if they turned out to be less effective than expected, the drug companies would reduce the price.
The first report on the outcome was due after two years but was not published until last December, seven years later. It showed that the drugs failed to delay the onset of disability in patients – defined as walking with a stick or using a wheelchair – and may even have hastened it. On that basis, the drug companies would have had to pay the NHS to use them to make them cost effective.
Despite this finding, the price was not reduced and the scientific advisory group monitoring the scheme advised that "further follow up and analyses" were required. It said that disability may yet improve, the disease may have become more aggressive and the measure of disability used may have underestimated benefit. There were 5,583 patients in the scheme at a cost to the NHS of around £50m a year, amounting to £350m over seven years to 2009. The Multiple Sclerosis Society said twice as many patients were using the drugs outside the trial. That implies a total NHS cost of £700m for a treatment that does not work.
In a series of articles in today's British Medical Journal, experts criticise the scheme. James Raftery, professor of health technology assessment at the University of Southampton and an adviser to Nice, said the scientific advisory group included representatives from the four drug companies, two MS groups, and the neurologists treating patients, all of whom had lobbied for the continued use of the drugs on the NHS.
"The independence of this group is questionable," he said. "Monitoring and evaluation of outcomes must be independent. Transparency is essential, involving annual reports, access to data, and rights to publish. Any of these might have helped avoid the current fiasco."
Professor Christopher McCabe, head of health economics at the University of Leeds, writing with colleagues in the BMJ, said: "None of the reasons for delaying the price review withstand critical assessment." Professor McCabe told The Independent: "We should be asking questions about paying for these drugs. In terms of disability avoidance, the evidence is not there."
Alastair Compston, professor of neurology at the University of Cambridge, defended the scheme. He said that despite a disappointing outcome, the scheme had "advanced the situation for people with multiple sclerosis" by improving understanding and care of the disease. Neil Scolding, professor of neurosciences at the University of Bristol, said the proportion of British patients treated with drugs (10-15 per cent) was tiny compared to France and Germany (40-50 per cent). He said the scheme had also led to the appointment of 250 multiple sclerosis nurses.
"[Though] expensive and flawed, if it turns out to have been no better than a clever wooden horse, then the army of MS healthcare specialists it delivered may make it more than worthwhile," he wrote. The MS Society claimed success for the scheme up to 2007 but after publication of the results last December, withdrew its support.
MS: why the drugs don't work
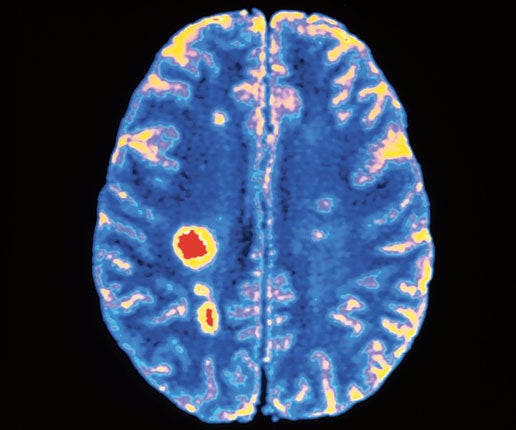
Multiple sclerosis is a chronic disease. It may take 40 years to run its course. In developing drugs to slow its progression, doctors have used brain scans to show lesions which the drugs appeared to prevent, and gave quicker results. Some experts thought the lesions were the disease but little effort was made to check. But preventing lesion formation does not prevent disability caused by the condition. The drugs deal with the lesions, not the disease.
Jeremy Laurance
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments