One in ten people dying from cancer 'given inadequate pain relief in final days'
Data from Macmillan Cancer Support equates to more than 12,500 people spending their last 48 hours in pain
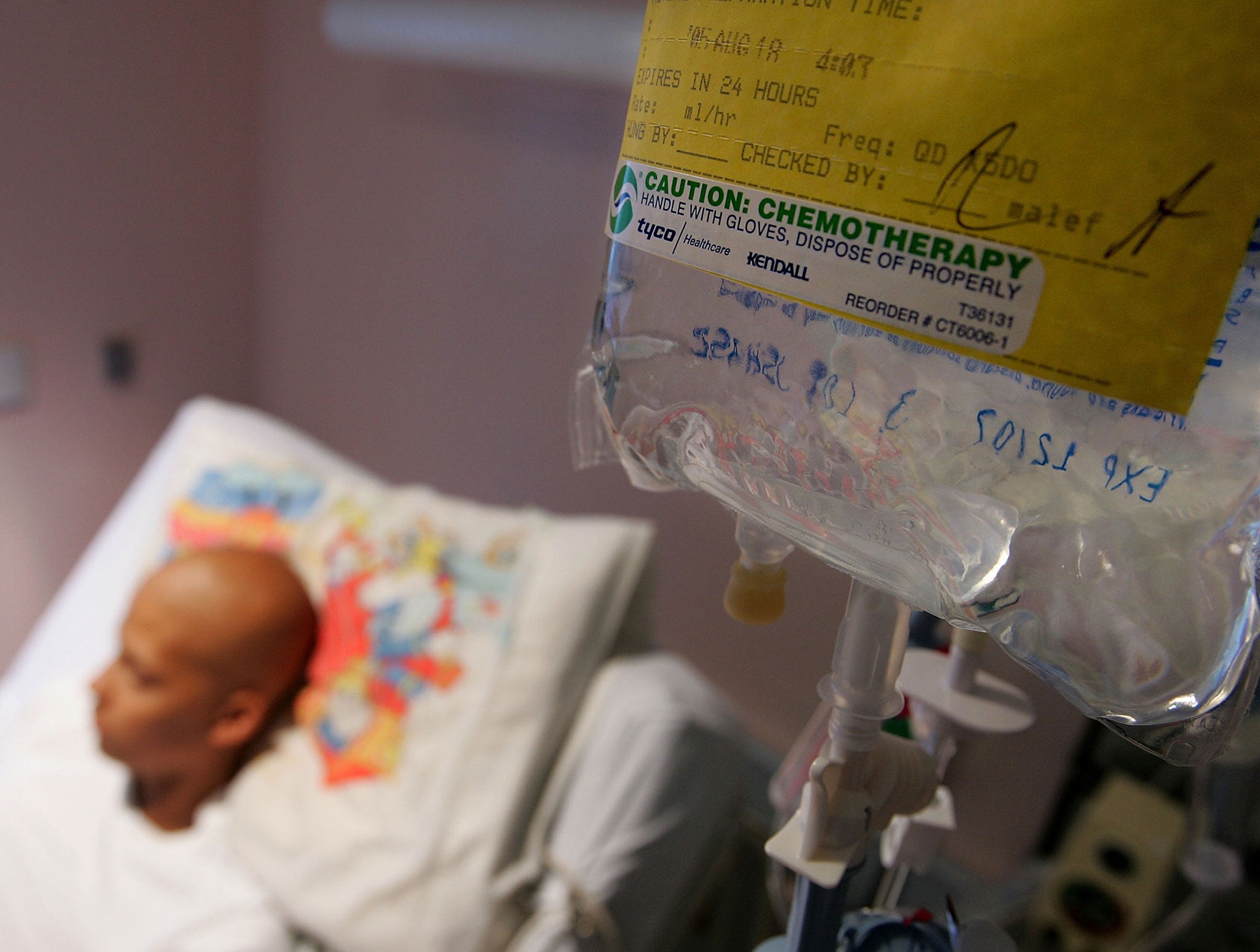
Nearly one in every ten people who died with cancer in England in 2014 spent the last 48 hours of their lives without adequate pain relief, according to shocking new research.
The data, commissioned by Macmillan Cancer Support, equates to more than 12,500 people spending their last days in pain.
Those patients are also twice as likely to die somewhere they do not want to that charity said. Previous Macmillan research shows that 73 per cent of people with cancer would prefer to die at home yet recent figures from the Office of National Statistics shows only a minority (30 per cent) are able to do so.
Data from the Care Quality Commission revealed last week the differences across England where eight hospitals were rated as outstanding for their end-of-life care – three of them are children’s hospitals (Alder Hey, Great Ormond Street and Sheffield) – and 94 were classified as good. However, 67 hospitals require improvement and seven were rated inadequate.
The charity called on the Government to carry out a major overhaul of palliative care to prevent further “pain and heartbreak”.
Publishing their results today (Sat), based on the latest information from the National Survey of Bereaved People, Macmillan said it is concerned that a lack of support at home, including pain relief, means that people with cancer at the end of life do not have enough choice over where they would like to be cared for and many are spending their final days in oversubscribed hospital beds against their wishes.
The charity urged the government to fix England’s ‘dismal’ variation in the quality of end of life care, by funding improvements recommended in a major independent review of choice at the end of life published in February 2015. Recommendations for measures yet to be implemented include access to 24/7 nursing, a record of a person’s preferences and fast and free access to social care.
Ann Osborn, 63, from London, who cared for her father when he was diagnosed with terminal bowel cancer in 2010, said: “The experience was awful, a lot of the time he was in terrible pain. My father wanted to die at home but there just wasn’t a way to make that possible.
“Alone in the early hours of the morning, he would call me in agony and I was eventually given the liquid morphine to make him more comfortable. Near the end, he was scared.
“We couldn’t cope and had to put him in a residential care home. I appreciate people should have the choice to be at home but there needs to be better social support to make this happen.”
Lynda Thomas, Chief Executive of Macmillan Cancer Support, said: “Quite simply, in the 21st century people should not be spending their final hours in pain in this country because the support is not there. It is tragic for the individual and distressing for family and friends who witness their loved one in pain.
“The review of choice at the end of life published last year set out a comprehensive set of recommendations that would help improve the end of life care in England. The government must fund and implement the recommendations of the review; we cannot carry on with the way things are.”
Dee Sissons, Director of Nursing for Marie Curie, joined Macmillan’s call for urgent improvement.
“Lack of anticipatory prescribing – which ensures medicines are readily available, and little support out of hours, are issues that need tackling,” she said. “It is also essential that staff have the right training around medicine management. It is possible for pain to be managed at home when people have the right support in place.
“Urgent improvements to the availability of high-quality community care and 24/7 palliative care are needed to ensure people can die at home in comfort and with dignity.”
An NHS England spokesman said: "This survey found that three quarters of bereaved people rate the overall quality of end-of-life care for their relative as good or better. However, we know that there are variations in the care and services that people receive and we want to continue improving people’s experience of care, including relieving symptoms such as pain, which is why the NHS locally is working hard to build on the strong foundations that have made the UK internationally recognised as leading the world in end of life care."
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks