The rise of Robodoc
Many operations are becoming less invasive and more efficient due to the growth of cyber-surgery. Nina Lakhani on a British medical success story
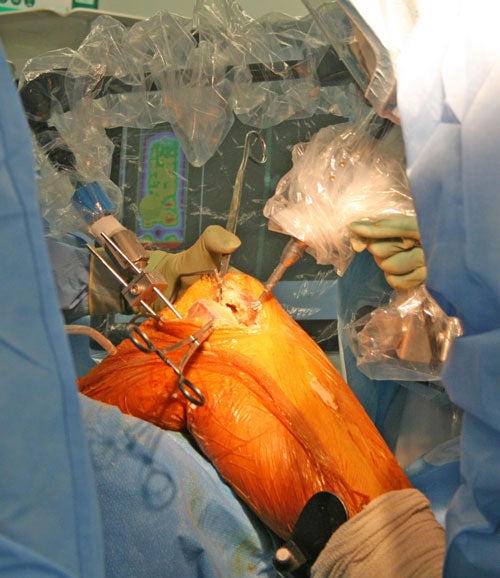
While surgeons are often criticised for their brusque bedside manner, few could accurately be described as robots. This is going to change as surgical consultations increasingly involve robotic systems to help diagnose, plan operations and reassure patients.
The development of robotic systems, both active and passive, is enabling surgeons to use keyhole techniques in hard-to-reach areas not previously thought possible. Britain is at the forefront of many advances. Collaborations between NHS surgeons, universities and private companies enable Britain to develop robotics more quickly and cheaply than North American and European counterparts.
Keyhole surgery is widely recognised as the greatest surgical advance since the arrival of anaesthetics in the 19th century. Less invasive techniques and technological developments that have created tiny cameras with telescopic lenses capable of being inserted into the body have brought radical improvements over the past 20 years.
Surgical specialists are constantly looking for ways to spread the benefits – less pain, minimal scarring, fewer complications and faster recovery – of minimally invasive techniques, from relatively simple procedures such as gall bladder removal to much "riskier" areas such as the repair of blood vessels. Practically every operation on blood vessels is now done from the inside: an aneurysm in the aorta, for instance, can be repaired through a small incision in the groin.
Some robots simply hold and direct a camera. Others participate much more actively. They work alongside computer systems to help plan what should be done in theatre and then ensure the execution is exact.
Robotics has proved invaluable for joint surgery where there is very little space for surgeons to move around. Neil Parkyn, 65, a retired builder from Bedford, was one of the first to undergo computer-navigated partial knee replacements to repair damage caused by osteoarthritis. Before the surgery last August at Charing Cross Hospital in London, he could hardly walk. Each partial replacement took only two hours and required much less physiotherapy than a total knee replacement. Mr Parkyn said: "When Professor Cobb went through the procedure, I was taken aback by a robot doing it, but when you stop and think about it, it's very accurate. Now I can walk two miles every day, I cycle and I swim. I've got my old legs back." Mr Parkyn is unlikely to need surgery again as the materials used should last a lifetime.
According to John Black, president of the Royal College of Surgeons, the next decade will see keyhole techniques develop in complex areas such as cardiac surgery. It is unclear whether developments in robotics will provide surgery with another eureka moment, but they have the potential to make surgery safer, easier, less traumatic and more reliable for thousands of patients each year.
Scar-free neck surgery
First developed by the US army in the 1980s to treat soldiers remotely, the da Vinci system is a sophisticated robotic platform increasingly used for complex surgical procedures.
It consists of a surgeon's console, a second console with a screen and a patient cart with four robotic arms – which holds three specially designed dexterous instruments and a 3D camera system. These are inserted into the patient's body through tiny incisions which the surgeon sees as a magnified, high-resolution 3-D image while sitting at the console. As the surgeon moves the console controls with his hands, state-of-the-art robotic and computer technologies scale and translate his hand movements into precise micro-movements of the wrist-like instruments inside the body. This allows operations to be performed with great precision and control.
Professor Neil Tolley and his researcher Asit Arora based at St Mary's Hospital and Imperial College London are the first to develop a robotic assisted technique for patients with an overactive parathyroid gland which avoids an unsightly scar on the neck. A 2cm incision is made below the collar bone on a site easily covered by a V-neck top. The camera and robotic instruments are inserted through three additional tiny incisions made in front of the armpit. Over the last year the team has successfully operated on six carefully selected patients. In each case, the abnormal parathyroid gland was removed with no complications, virtually no blood loss, and no scar. The team, backed by former health minister Lord Darzi, is now investigating its application for patients with obstructive sleep apnoea and snoring.
Weight-loss surgery
Hundreds of operations such as the gastric bypass are carried out every week as the number of severely obese Britons continues to rise. The FreeHand robot is a flexible white arm which holds the telescopic camera inserted into the patient's abdomen, acting as the surgeon's eyes in areas hidden by layers of fat.
It is controlled by an infrared sensor located on the surgeon's forehead: to move the camera left or right, the surgeon turns his head accordingly. To zoom in or out, the surgeon touches a foot pedal to confirm an arrow change and then nods until the laparoscope has panned in or out as required.
The new slicker version of a camera-man robot clamps on to the operating table and takes only minutes to set-up. Surgeons previously had to deal with inconsistent assistants because some trainee surgeons were better than others at this tiring but skilful job, according to Professor Peter Sedman, an obesity expert from Hull and East Yorkshire Hospitals.
Urologists have started to use the FreeHand surgeon for tricky prostate operations which can take up to six hours. The robotic camera means the surgeon can sit down and take his time without worrying about the camera holder tiring out.
Near-perfect knees
This month's launch of the Acrobot Robot, which helps orthopaedic surgeons to carry out computer navigated partial knee replacements, is the culmination of 19 years' work for Professor Justin Cobb and his team at Imperial College London.
Because everyone walks and stands slightly differently – some people are a little bow-legged like David Beckham, others are very straight-legged like Kate Moss – different parts of the knee joint wear out as we get older. Until now, patients would undergo an operation to replace the whole joint, even though only a small proportion was damaged. This new system using a semi-active robot enables the surgeon to partially replace the joint incredibly precisely because the whole procedure is planned in conjunction with the robot beforehand.
The patient gets a CT scan which projects 3D images on to the computer within 45 seconds. On the screen, the surgeon then files down the worn-out area and replaces it, virtually, using the integrated computer software: any surprises or mistakes are ironed out at this stage. On the operating table, the robot will not allow the surgeon to deviate from the plan so absolute accuracy is virtually guaranteed as the robot is always right. The partial replacement feels like the old knee, something never achieved in a total joint replacement.
The next step, to transfer the technology for use in partial hip replacements, is under way; other parts of the skeleton such as the shoulder and elbow will follow.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments