Don't scratch the itch: Scientists find substance that could be key to stopping the sensation
Researchers found that removing natriuretic polypeptide b causes an itch to disappear
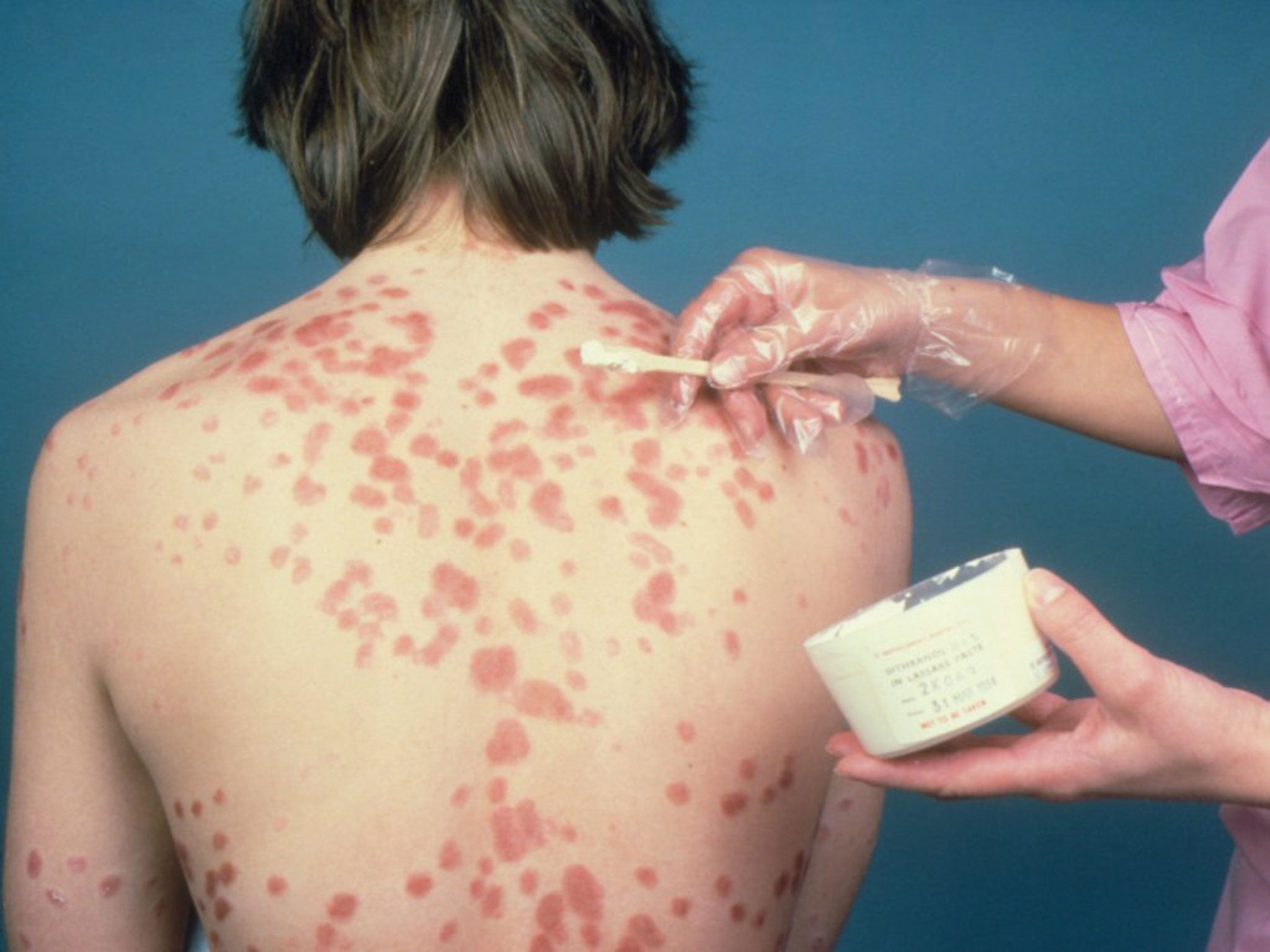
Scientists have discovered a key substance in the central nervous system responsible for transmitting the sensation of an itch from the skin to the brain – a finding that raises the prospect of new treatments for serious itching conditions.
Medical researchers have found that the neuro-transmitter, a small molecule that transmits signals between nerve cells, plays a crucial role in the perception of an itch, which in some people can lead to chronic, long-term scratching.
Removing the neurotransmitter – called natriuretic polypeptide b (Nppb) – causes an itch to disappear while replacing it within the spinal cord results in the re-appearance of the itch, said Mark Hoon, a lead investigator at the US National Institute of Dental and Craniofacial Research in Washington DC.
“Our work shows that itch, once thought to be a low-level form of pain, is a distinct sensation that is uniquely hardwired into the nervous system with the biochemical equivalent of its own dedicated land line to the brain,” Dr Hoon said.
“Overall, a better understanding of the biology of itch and the molecules involved can only mean we are closer to finding a treatment for chronic itching. Most people think of an itch as an inconvenience, but there are patients who have a poor quality of life because of chronic scratching,” he said.
Patients suffering from chronic skin disorders such as psoriasis and eczema often experience long-term itching, but it can also be brought about by a variety of temporary conditions such as fungal infections, scabies, sun burn or just dry skin.
There are a number of reports in the medical literature of very severe itching over long periods of time causing serious harm. Some patients have scratched their skin until it bleeds while others have scratched through to the bone, and even through the scalp to the brain.
The study, published in the journal Science, involved testing various neurotransmitters of the central nervous system to study their roles in the perception of temperature, pain and itching. They found that one, Nppb, appeared to be involved only in itch, said Santosh Mishra, a researcher in Dr Hoon’s laboratory.
Laboratory mice that had been genetically modified so that they did not have the gene for making the Nppb protein were incapable of responding to itchy sensations, although they were still capable of feeling other sensations such as pain and heat.
“We tested Nppb for its possible role in various sensations without success. When we exposed the Nppb-deficient mice to several itch-inducing substances, it was amazing to watch. Nothing happened. The mice wouldn’t scratch” Dr Mishra said.
The scientists also found that there were dedicated nerve fibres in the spinal cord that responded to the Nppb neurotransmitter. When their nerve fibres were removed, their ability to feel an itch was also eliminated, Dr Hoon said.
These findings are strong evidence to support the widely-held view that itch is not a special type of pain, but a unique sensation in itself that has its own neurotransmitter and dedicated “landline” to the brain, he said.
“We can see the differences between the sensation of pain and of itch in a laboratory mouse, which will scratch itself if it feels an itch but lick itself, gnaw at its skin or flinch at a painful stimulus,” Dr Hoon said.
“Now the challenge is to find similar biocircuitry in people, evaluate what’s there and to identify molecules that can be targeted to turn off chronic itch without causing unwanted side-effects,” he said.
“So this is a start, not a finish.”
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks