Born with congenital heart disease: The battle to save my newborn son's life
Richard Hammond recalls the lows and then highs of the crucial first few weeks

The night of 23 December. It's some time in the late evening, it's hard to be exact: time, for the parents of babies clinging to life in a paediatric intensive care unit, turns thick and sticky, its edges lose definition and hours disappear. Tonight is my turn on watch while my partner Emily looks after our older son. Alarms are pinging and jagging into hearing.
I am staring into my 13-day-old baby's eyes and watching death course through his body, hunting opportunities to finish its cruel work. Outside of my boy's cot, a team of seven medics have appeared from out of thin air. "When a baby gets into trouble, we're like dogs smelling sausages," says a nurse. The consultant takes exception to her analogy, but it perfectly describes the extraordinary speed at which this team has formed. Over the next three hours, they will fight to bring little Ptolemy Hammond back to safe shores.
The consultant is the commander of a warship under fire: pacing around the bridge, stalking the stats, constantly issuing commands, adapting strategy, balancing threats and nipping in with a nimble attacking stratagem whenever opportunity presents itself. It is exhilarating, shocking and agonising all at once.
I feel detached and am physically wavering, until eventually I can watch no more. I retreat to an empty waiting room.
Ptolemy is critical. I spend the wait steadying myself for when the consultant comes to tell me he's gone. This lasts half an hour, then an hour, then two. The hospital around me gets smaller and smaller and quieter and quieter, until it seems only to exist as an abstract idea.
In the earliest hours, the door to the waiting room swings open and in walks the consultant and a nurse. Before either have time to say anything, before the door has swung back into its frame, I know that the consultant is going to tell me my son has died. The consultant is exhausted, his face seems to suggest defeat.But as I think these things, I notice the nurse is smiling. Not the sad smile of bad news but one that has joy in it, maybe. Relief, certainly. My heart restarts. The consultant is speaking: we've stabilised him. He's ill but we've got him back up to a viable position.
We've clicked past midnight. Ptolemy has been alive 14 days now. One day older. He will fight on.
My fourth child, my second with Emily, was born in Oxford's John Radcliffe Hospital on 10 December. We had no prior warning that he, or she, was anything other than a healthy, average baby. He arrived with the full set of limbs and digits. We gave that relieved release of held breath all parents will recognise.
Our as yet unnamed bundle of joy – we'd drawn a complete blank on names – was the normal purple, screwed-up faced, gelatinous muddle of chubby love. Within a minute or two, the midwife had him on Emily's chest for their first proper hello. It would be another three days, and another city away, before either of us would hold him again.
That's when a quiet voice began to chime in my head: "Something isn't right, the way he's breathing… too much effort? Something?" I asked the midwife what was going on, expecting to be told that everything was normal and to be given that gentle and kind treatment nervy dads are so reassured by. She began to do just that, but then I saw a change in her body language and that was the moment I felt the floor, walls and ceiling rush away. She took our son from Emily and called over a doctor. Within moments, a tiny oxygen mask was on our baby's face and the theatre team's mood had dropped. The doctor asked for an oxygen saturation monitor to be brought to theatre.
It arrived and they attached a monitor line to our boy's hand, the first line of dozens that would snake themselves out of the mythology of medicine and into his body over the coming month. The numbers told an instantly bad story: his newly functioning lungs were taking in air, but he was failing to take enough of the oxygen from it to maintain life.
The doctor listened to his heart. Our first taste of the unreality of life-changing, emergency medicine: a taste sugared through the gentleness of the word chosen to describe what the doctor had discovered. "I can hear a murmur in his heart." Not break or tear or crisis or failure. Just a murmur.
Our world dissolved into a controlled rush into neonatal intensive care.
Within hours, we had a diagnosis: pulmonary atresia with intact ventricular septum. A form of congenital heart disease (CHD) in which Ptolemy's heart is unable to efficiently run the process of oxygenating and circulating his blood. It is basic and fundamental to life. We are transferred to Southampton General Hospital, home to one of Europe's finest paediatric cardiac teams.
The seriousness of Ptolemy's illness revealed itself in progressive chunks of new information: like a horrific fold-out poster, where each day, a newly revealed section pushed his chances of living further and further away from us. We moved from our home in Oxford to the strange new world of a hospital in a city we didn't know. We lived in the hospital for five weeks.
Ptolemy's first major procedure is an attempt to open up his heart valves. The valves are expertly teased open but Ptolemy's heart fails to cope with changes this new circulation brings about. Within days, a Blalock-Taussig (BT) shunt is fitted, 3mm of Gore-Tex tube stitched to the outside of his beating heart, further modifying his circulation. The shunt is functioning but Ptolemy becomes critical. For the night of 23 December, he tugs at the strings of death.
As parents locked in the closed world of a hospital, we do not choose when to eat. We do not choose when to sleep. Our reality is a series of stats on which our will has no impact.
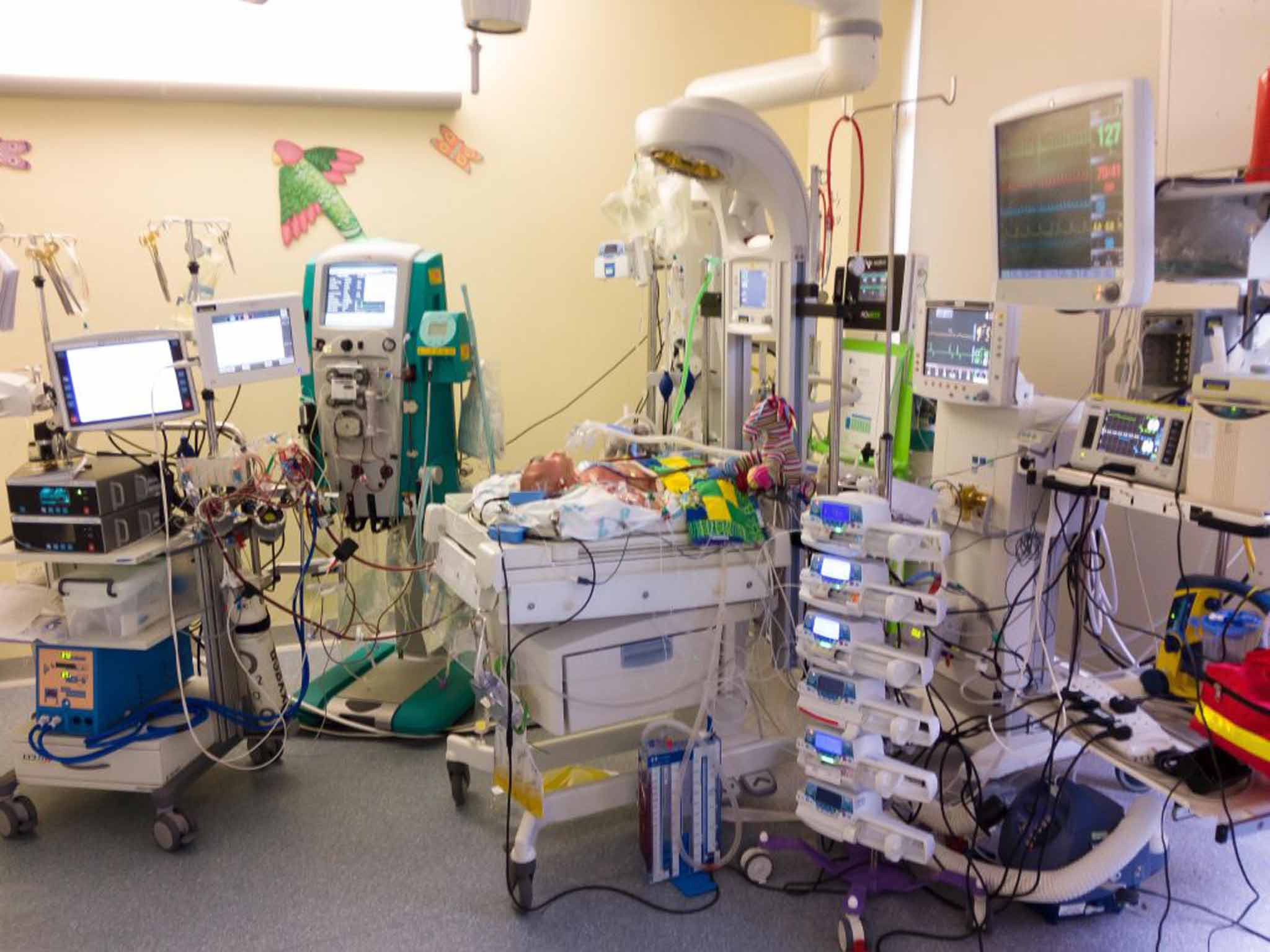
2.4ml/h Dinoprostone, 40 per cent oxygen, SAT at 65-75, target SAT at 75-85, GLu 6.1, Lac 3.3, ph 7.37, FIo2 ltr/min .21, 68/47, 144 broken-heart-beats/min, 66 breaths, 9lbs and half an ounce.
These stats, these are the currency of the ICU – constantly, hawkishly monitored. They are the numbers of life for Ptolemy.
On Christmas Eve, he is no better. An operation to tie off his pulmonary artery is planned. We sign yet another consent form reminding us of risks that include death and severe disablement. The brilliant team pull him through and are able once again to stabilise our boy, to the point where we go to bed on the night before Christmas with a fearful, prickling sensation of optimism.
But early on Christmas Morning, his numbers fall away from normal ranges. His blood turns to poison and his organs begin to fail. The optimism of the previous night has evaporated and he undergoes an emergency operation that will see many of Ptolemy's systems transferred to machines. Afterwards, he lies motionless in a cot, a clay doll. His chest is open and tubes take his blood directly away from his heart and into a bypass machine. His lungs are replicated by pumps and his renal function now takes place outside of his body.
He is brain, muscle and bone while his heart is rested in the hope that this will give it a chance to recover. They set a deadline of two days: no improvement and Ptolemy will not see 2015.
It is 28 December. Ptolemy is awake, lively even, as lively as a morphine-stuck baby can be. I am holding his hand. It is a hand filled with oxygenated blood provided by his own working heart, his own working lungs.
A consultant tells Emily: "You've been given a Christmas present."
Ptolemy is no longer critical.
On 16 January, we are back home. Our son will have many hurdles to jump as he fights his way from here. A major operation awaits this year to re-plumb his heart more permanently. It will leave him with a system that stands a strong chance of getting him to adolescence. What happens then is anybody's guess – he has a 15-year head-start on technology in an area of medicine that is rapidly progressing.
For now; every second falls to us as drops of crystal time filled with hope and love and optimism. Life has changed, and it is scarier than it was before but it is also more beautiful and the imminent loss of it a dark misery I now understand well. Our boy is strong. Thanks to the NHS, an astonishing group of surgeons, nurses, consultants and specialists, but also to our society's choice to invest in the possibility of life, without caveat or consideration of social position – thanks to these things he is alive, smiling and filling nappies with a vigour you wouldn't believe.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments