The cost of NHS health care: Deciding who lives and who dies
Bowel cancer sufferer Simon Hawkins’s life was saved by the drug Avastin. But from this week, it will no longer be available to NHS patients because it is considered too costly. Jeremy Laurance explores a medical dilemma

You may not be familiar with the name, but there is a strong likelihood you soon will be, in the coming election battle over the NHS. It is that of Simon Hawkins, a 59-year-old cancer survivor from Winchester whose encounter with David Cameron a little over a year ago could come back to haunt the Prime Minister.
Mr Cameron met Mr Hawkins in September 2013 at the John Radcliffe Hospital, Oxford, where the Prime Minister announced a two-year extension to the Cancer Drugs Fund and, in Mr Hawkins's words, "paraded me as a success of the fund and made assurances to me that … his government was committed to empowering the clinicians, doctors and oncologists to make the life-saving decisions."
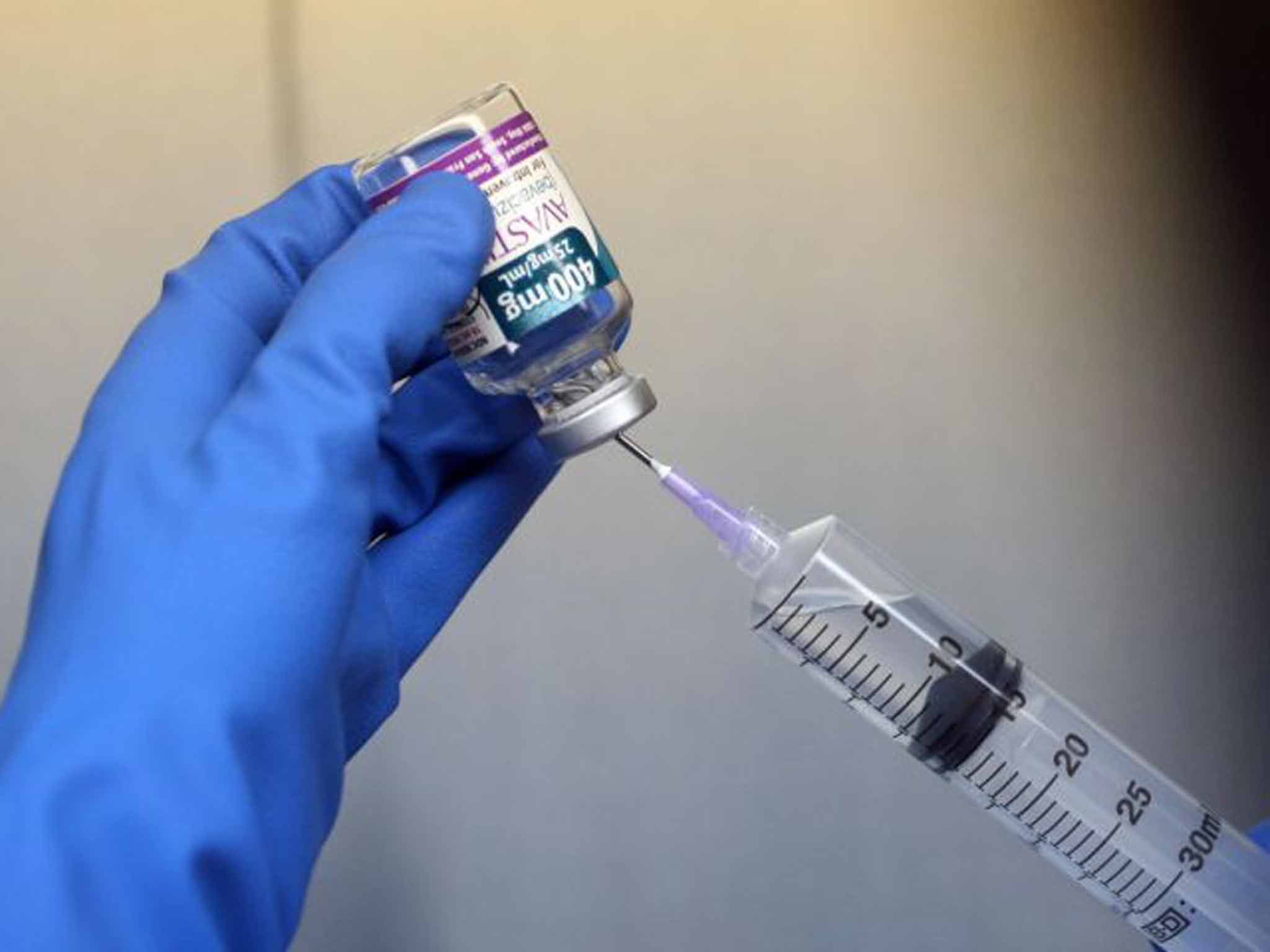
On Thursday, however, Mr Cameron will renege on that promise when the Cancer Drugs Fund cuts Avastin, the very drug that saved Mr Hawkins's life, from its approved list. Along with 16 other drugs, Avastin (chemical name: bevacizumab) will no longer be available as a first-line treatment for new NHS patients with advanced bowel cancer because it is judged too costly for the benefits it brings.
Mr Hawkins is not impressed. He had been told in 2010 that his bowel cancer had returned and he had just 18 months to live. But, after a course of Avastin, his tumour shrank enough for surgeons to remove it and, almost five years later, he remains well.
He has launched a petition, which has so far gained more than 4,000 signatures, claiming that the promise Mr Cameron made to him 16 months ago has been broken.
"How do you think I felt when I discovered that the drug that saved my life would no longer be available to cancer patients? Appalled and disgusted. More than that, it scared me that I had been incredibly lucky to be ill at the right time. The treatment of this awful disease should not be a matter of luck," he wrote on The Huffington Post.
Mr Hawkins's distress is widely shared. There is a deep revulsion at the idea that patients may be prevented from accessing an effective, potentially life-saving, treatment merely because of cost. It undermines the NHS's founding principle of providing universal care according to need, and amounts, the critics say, to putting a price on life.
But if that principle held when the NHS was founded in 1948, it is no longer sustainable today. Huge changes in demography, technology and the pattern and burden of disease have put the NHS budget under immense pressure. The priority has changed from providing all the care that patients need – never, in fact, a realistic prospect – to dividing up the care that is available (or the budget for it) so that it is distributed equitably.
Many people find it difficult to accept that questions of money should enter life-and-death decisions about health care. But the NHS has a fixed budget this year of around £110bn in England. The issue is, how do we spend that money wisely, for the benefit of the whole population? Does the cost of a cancer drug such as Avastin deliver as much benefit as, for example, investing more in health visitors to reduce the infant mortality rate? Or, more directly, would the cash spent on buying cancer patients a few extra months with the drug be better used to fund improved palliative care for them at the end of life?
The body tasked with making these Solomon-like judgements is the National Institute for Health and Care Excellence (Nice), established under Labour in 1999. Although not at first explicitly acknowledged, its chief role is to ration the care available by deciding which drugs to approve for use on the NHS and which to restrict. (Alan Milburn claimed he was the first Health Secretary ever to acknowledge the necessity of rationing, but that was several years later.)
Since March 2000, Nice has conducted 328 "technology appraisals" and made 500 recommendations, mostly giving the green light to the NHS to use the new treatments. But in 15 per cent of cases, it has ruled against the new drugs.
The refusal rate for cancer drugs has been higher – almost a third (32 per cent) of the 116 appraisals and 162 recommendations have ended with a 'no' – and a further five per cent have been recommended for use only in research trials.
It is the refusals, naturally, that grab the headlines and provoke the protests – especially when they have involved cancer drugs. In one case, members of a kidney patients' group invaded Nice's central London HQ and accused the organisation of "barbarism" after it gave the thumbs down to a new treatment.
The drug industry regularly protests, too, with figures such as Sir Andrew Witty, chief executive of GlaxoSmithKline, threatening to remove its business from the UK and decamp to the US. But though the companies hate Nice, they need it, too. Once the organisation has given its imprimatur to a drug, it can boost sales around the world.
The perverse aspect of the protests from charities and patient groups is that they ignore the drug industry's role. For them, there is only one villain and that is Nice. Yet when a drug is rejected, the company involved will often return to the negotiating table and offer the NHS a substantial discount on the cost. By turning their fire on Nice, and neglecting the other player, charities are effectively saying that protecting drug-company profits is more important than protecting the NHS.
To take the heat out of these disputes, the Government intervened five years ago to create a separate organisation with a separate budget to pay for the very expensive cancer drugs that were starting to become available.
The Cancer Drugs Fund, set up by ministers in 2010, exists to provide stopgap funding for drugs either rejected or not yet assessed by Nice, where they are prescribed by a cancer specialist for an individual patient.
In bypassing Nice, it bypassed the principles of fairness and value for money on which Nice was founded and has been roundly criticised for doing so.
For a while, however, it worked. It defused what would otherwise have been an increasingly desperate situation in which some patients were told they could not have the drugs their cancer specialist had recommended.
But now the Cancer Drugs Fund itself has run out of money. Its annual budget of £200m has been increased to £280m, but it warned last year that it would rise to £340m without cuts. In January, it announced that it, too, would begin rationing treatment by culling 16 drugs prescribed in 25 indications from its approved list, including Avastin, the drug that Mr Hawkins says saved his life.
The move is another marker that cancer treatment is becoming unaffordable. Cancer drug prices have risen at four times the rate of inflation, a rate that is hard to justify. That is why we need Nice, to ensure that the NHS is getting value for money.
The scale of the challenge is daunting. As populations age, more people are developing cancer, they are surviving longer with it and treatment costs are soaring. There were 331,000 new cases of cancer diagnosed in 2011 in the UK, up by 23 per cent among men and 43 per cent among women since the mid-1970s. The bill for treating them was put at £5.6bn by an Oxford University study published in 2012. It is projected to rise by more than half in the UK over the next decade at a time when the NHS is facing an unprecedented period of austerity.
It is a poor nation that cannot afford to spend £10,000 (or even £100,000) on a drug to ease the suffering and extend the lives of cancer patients. But it is a foolish and irresponsible nation that does not look critically to see that that £10,000 buys the maximum possible benefit for the patients whom it is intended to help.

Who lives, who dies? How the decisions are taken
Decisions about who will live and who will die are taken behind the "blood-stained portals" (as one irate cancer specialist put it) of a glass office block in central London. This is Nice's headquarters, where the organisation rations care by convening appraisal committees to consider new treatments referred to it by the Department of Health.
The committees comprise a couple of dozen health professionals and patient representatives who meet to weigh up evidence collected over months from the drug company, patient groups and other interested parties and including, crucially, an economic assessment of cost effectiveness.
The drugs that Nice considers have already been licensed by the European Medicines Agency for use as safe and effective treatments. That they work is not in doubt – the issue for Nice is: do they deliver value for money? Nice's job is to answer the question: is the benefit they bring worth the cost, or could the money be better spent buying, for example, extra nursing care?
To do that, it relies on what are acknowledged to be bafflingly complicated calculations based on economic models around which dispute swirls. The bottom line for Nice is that a treatment must deliver an improvement in quality and/or length of life at a reasonable price. That price is set at £20,000-£30,000 per Quality Adjusted Life Year (Qaly) – a measure of the improvement in either the quality or quantity of life that treatments can bring.
This is not a firm limit, however. For truly innovative treatments, Nice allows a higher price. Glivec, for example, the first of the targeted biological therapies for cancer was calculated to cost more than £40,000 per Qaly but was still approved. In recent years, it has also accepted a higher limit for patients with terminal conditions for whom an extra few months means more than for other patients. The limit for end-of-life treatments is set at £50,000 per Qaly but can rise as high as £80,000.
There is much dispute about whether Qaly's are an accurate measure of a drug's benefits and whether, in individual cases, they have been accurately calculated. They were criticised last year by the European Consortium on Healthcare Outcomes, which said that they failed to reflect variations in people's views of illness and disability. But they are the best we have. They provide a value-for-money measure of the benefit a treatment provides that allows it to be compared with the value for money offered by other treatments.
This is the only way we have of ensuring that spending decisions in the NHS are fair and equitable. If a drug costs too much for too little benefit, the NHS must be able to deny it to patients. Otherwise, the market will push drug prices ever higher, threatening health care for us all. Denying a patient a life-saving drug is bound to make them and their loved ones angry. But providing the drug to one person means that someone else is denied the care they need.
When the Nice appraisal committee is ready to make its decision about a drug, yellow slips are distributed round the table and members of the committee record their votes. The slips are collected, counted up and delivered to the chair who declares the result (and has the casting vote in the event of a tie – which has happened). It is the culmination of a bureaucratic process that takes months, involves complex calculations and often heated debate. It is necessary and important work, but also heart rending. There is no escaping the impact the decisions have on individual patients' lives.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments