Superbug drug launched to fight growing threat of antibiotic resistance
New medicine will tackle 'exponential' increase in resistant bacteria in hospitals, say scientists
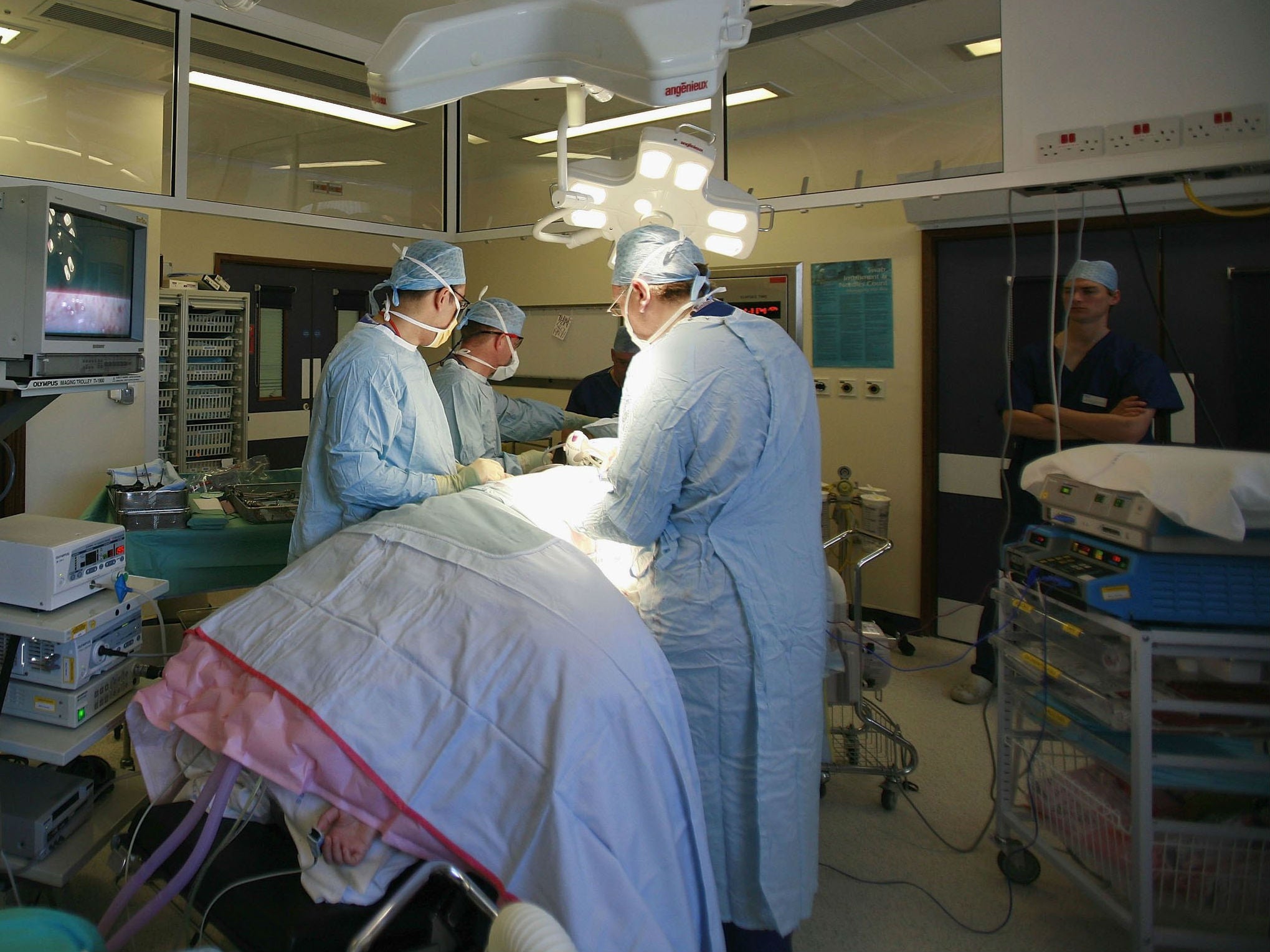
A new antibiotic designed to fight drug-resistant ‘superbugs’ has become available to patients in the UK.
Doctors are “running out of options” for treating common infections caused by bacteria which mutate to resist regular antibiotics, said microbiologist Matthew Dryden.
“Resistance is increasing, almost exponentially. It's a problem facing every emergency department in this country,” he told The Independent.
But innovative new drugs like Zavicefta, which combines a traditional antibiotic in the same class as penicillin with a brand new drug that attacks resistance mechanisms, are being introduced to tackle the growing threat of antibiotic resistance.
“One method of resistance is that the bugs have developed enzymes that destroy antibiotics,” said Dr Dryden.
“This antibiotic is a combination of the new and the old. It's combining two drugs, one that's entirely novel, avibactam, which inhibits the enzymes that cause resistance. That’s combined with a drug we're pretty familiar with, called ceftazidime, that we know is well-tolerated.”
Scientists are racing to develop a new generation of drugs capable of defeating even the most resistant superbugs, which represent an “increasingly serious threat to global public health,” according to the World Health Organisation.
Antimicrobial resistance is caused when bacteria, viruses, fungi and parasites change through continued exposure to drugs, which then become ineffective against them.
Over time, excessive use of antibiotics could lead to minor infections causing serious health complications, making surgery and treatment for diseases such as cancer much riskier.
Zavicefta, made by pharmaceutical giant Pfizer, will used to treat multi-drug resistant infections including complicated abdominal infection, complicated urinary tract infection and hospital-acquired pneumonia.
But while it will provide patients with considerable benefits, it does not represent the end of the fight against superbugs as bacteria can also become resistant to new drugs, said Dr Dryden.
“The threat hasn't gone away, so we have to have different solutions. New antibiotics is an important aspect of it, but to persuade the world to stop using more antibiotics is really difficult.”
Better education on the risks of antibiotic resistance, improved diagnostic tools and the development of alternative treatments could all be used in the fight against superbugs.
“We use antibiotics too much, not just in human health but in animal health, in livestock and agriculture,” he said.
In some areas, drug leakage from factories can mix with untreated sewage in rivers, causing a “primeval mix of bacteria and low-dose antibiotics” which encourages the bacteria to mutate and adds to the problem.
Conservative MP Kevin Hollinrake called the threat of antibiotic resistance the “new black death” ahead of a parliamentary debate last week over a new report on the issue.
The review, conducted by Jim O’Neill, predicted 10 million lives would be lost annually by 2050 as bacteria become more drug-resistant.
“We do need a solution because antibiotics are absolutely life-saving,” said Dr Dryden. “We can't envisage our children dying of simple bacterial infections that were readily treatable. It's a shocking vision of the future.”
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments