Ashya King: Is proton beam therapy safe?
The NHS says it poses extra risk because whole spine needs to be radiated - but Czech experts insist this is simply not the case
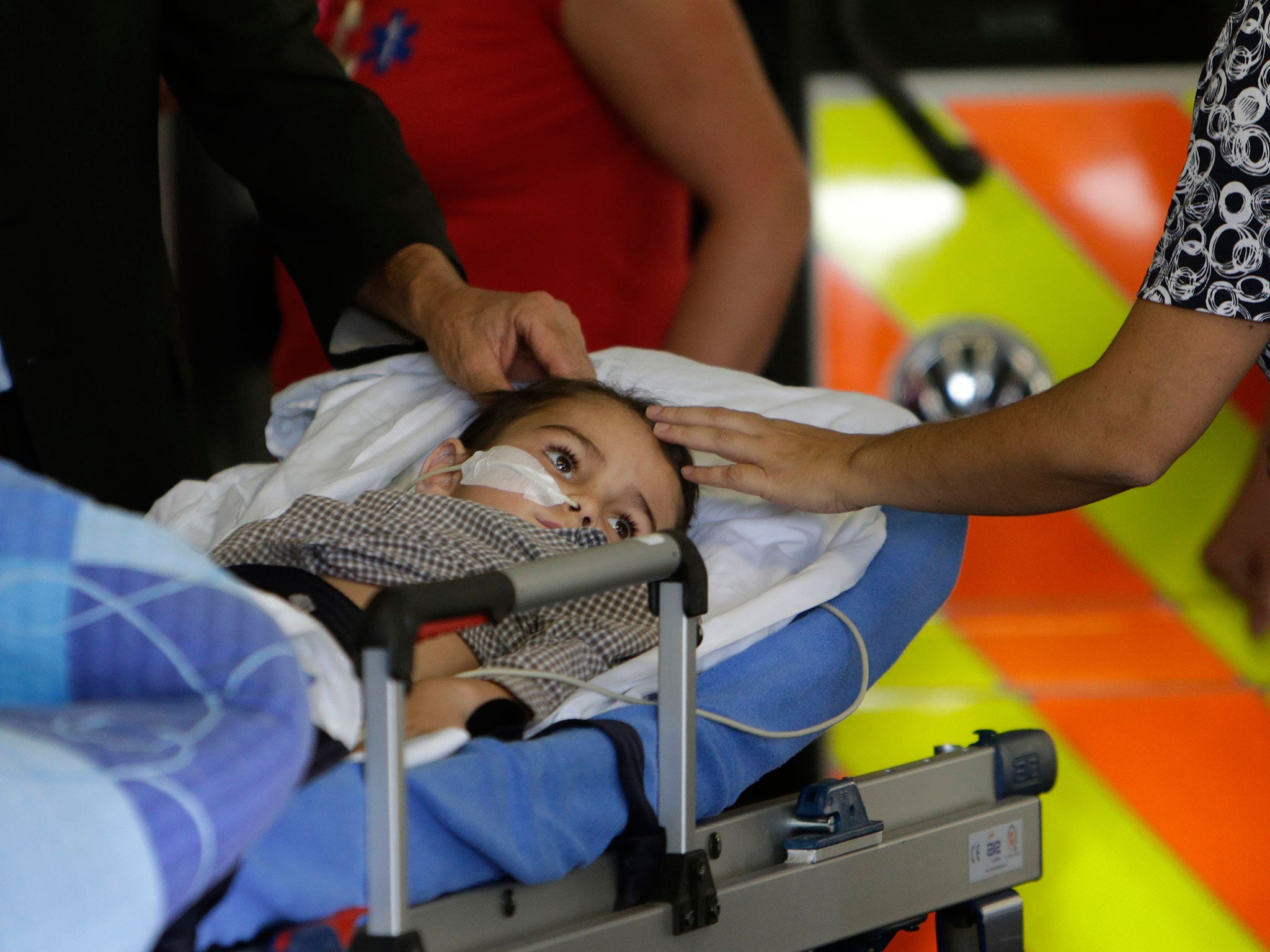
Ashya King, the five-year-old boy with brain cancer who was “abducted” from Southampton General Hospital by his desperate parents, is due to arrive tomorrow morning at the Proton Therapy Centre in Prague, where he is soon to begin the latest stage of his treatment.
Brett King, Ashya’s father, visited the centre to be briefed on Ashya’s proton treatment programme after the family was flown to the Czech Republic by private jet from Spain, where the child’s parents had been held and then later released following an abortive arrest warrant issued by Hampshire police.
Mr King had disagreed with Ashya’s doctors at Southampton, who wanted the boy to undergo conventional radiotherapy using high-energy X-rays rather than proton beams. Like many parents, Mr King had used the internet to research both kinds of radiotherapy and decided that protons would have fewer long-term side-effects.
The case has highlighted the increasingly fraught relationship that often develops between doctors and patients in the age of the internet. Many patients, and especially the parents of very ill children, are questioning everything that the medical profession had once believed, in a more deferential age, was solely their domain.
Even the most cursory internet search would reveal missing fragments of information about the risks and benefits of proton-beam therapy compared with conventional radiotherapy, which is not helped by the official sources of advice within Britain.
In pictures: Ashya King's case
Show all 22For instance, we asked the Department of Health why medulloblastoma, the type of cancer of the brain’s cerebellum suffered by Ashya, was not a recommended treatment for overseas proton-beam therapy – all cancer patients have to be considered by a special panel of seven experts because of the lack of facilities in the UK.
We were directed to the press office of NHS England which in turn directed us to a website run by the Children’s Cancer and Leukaemia Group, charitable foundation based at Leicester University. The inadequate information there was similar to the official explanation cited by University Hospital Southampton NHS Trust.
In a statement released last week, the trust said: “[Proton therapy] was explored with the family and they were informed that in Ashya’s case there is likely to be no difference in survival between standard radiotherapy and proton radiotherapy and overall no proven significant benefit. Therefore, the Trust considers there is no benefit to Ashya of proton radiotherapy over standard radiotherapy.”
Peter Wilson, head paediatrician at Southampton, said in a press interview over the weekend that proton therapy is not deemed to have any benefit because medulloblastoma requires the entire brain and spine to be irradiated, due to the risk of stray cancer cells seeping out from the original tumour into the cerebral-spinal fluid.
The implication was that proton therapy could not be used to irradiate the spine and brain. However, the Prague centre has successfully treated children with medulloblastoma, irradiating the entire spine in the process to eliminate any stray cancer cells, with less radiation delivered to the healthy tissues in front of the spine.
So clearly proton therapy can be used to irradiate the brain and the spine with fewer theoretical side-effects, so why is medulloblastoma still not a recommended treatment for proton-beam therapy overseas?
Nicky Thorp, a consultant clinical oncologist at the Clatterbridge NHS Cancer Centre finally provided an explanation. It is not about protons as such, it is about the delay that is involved with arranging treatment overseas, which in the case of medulloblastoma is critical for the chances of a cure.
“There is possibly a small advantage [with proton therapy], but it is not proven… but to see these benefits the child has to live and be cured,” Dr Thorp said. It is critical for children to undergo radiotherapy and chemotherapy within four to six weeks after surgery to limit the chances of metastatic disease – and overseas treatment can introduce life-threatening delays, she said.
“Why isn’t medulloblastoma on the list? This is because we always balance risk and benefit. The benefits of protons over X-rays are probably small. The risk when we don’t have a proton facility in the UK is that these children will have to travel overseas… but timing of radiotherapy is important,” Dr Thorp explained.
“You can lose this window of opportunity, and the biggest harm you can do to a child with medulloblastoma is to not cure them when you should be curing them. It might build in a delay to get definitive treatment,” she said.
“We have discussed putting medulloblastomas on the eligibility list many times. We made the decision not to because we don’t want to cause the greatest harm to these children by not curing them… When we have proton centres in Manchester and London in 2018, these tumours will be on the list,” she added.
“I would want my child to get timely radiotherapy. I’d give that priority over treatment with protons. My first priority would be to get a cure for the patient.”
Subscribe to Independent Premium to bookmark this article
Want to bookmark your favourite articles and stories to read or reference later? Start your Independent Premium subscription today.

Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies