Britain lags behind in the telemedicine revolution
It saves lives and money, and patients like it. So why isn't the NHS taking it up?
NHS savings of £1bn a year, a 40 per cent reduction in hospital admissions and improved patient care are some of the benefits promised by telemedicine, according to medical experts who describe it as the future of healthcare. Patients will benefit from faster life-saving treatments for a range of illnesses from strokes to diabetes, regardless of where they are.
Despite the revolutionary potential of telemedicine – the use of information and communication technology to assess, diagnose and monitor patients who are thousands of miles from a doctor or consultant – both here and abroad, Britain is failing to exploit the advantages, a new report warns.
A Royal Society of Medicine conference, which starts tomorrow, will highlight the extent of telemedicine's potential, showcasing projects from the Scottish Highlands to Swansea and Somaliland that demonstrate its impact on healthcare, from psychiatry and speech therapy to cardiology.
One trial, on the Isle of Bute, saw monitoring systems in the homes of people suffering with chronic bronchitis or emphysema. The project, run by Telehealth Solutions together with NHS Highland and Aberdeen University, led to hospital admissions being reduced by 91 per cent. Telehealth's Charles Lowe said: "Information provided by our systems can be interpreted and used to head off a pulmonary incident. We cut the numbers of admissions right down. That's £2,500 to £3,500 [per] admission."
Telemedicine is not limited to connecting geographically remote patients to medical resources. It can also be used to streamline the delivery of clot-busting drugs for patients suffering strokes. Dr George Crooks, medical director of NHS 24, responsible for Scotland's telemedicine provision, said it was vital that such drugs were given within four hours of a stroke occurring. "We speed up that process by having a doctor consult via videolink. Not only does this have the potential to completely reverse the paralysis a stroke can cause, it could represent a real-life saving of £20m over 10 years," he said.
Telemedicine can also have an equally important but less dramatic impact on other conditions. The NHS spends 70 per cent of its budget on 15m people with long-term illness such as diabetes, heart and lung diseases. More than two-thirds of acute hospital beds are filled with people with these conditions, often because consultants see them too late, according to diabetes specialist Dr Richard Pope, from the Airedale NHS Foundation Trust Hospital.
Under new plans set out by the Secretary of State for Health, Andrew Lansley, acute hospitals face financial penalties every time a patient is re-admitted to hospital within 30 days of discharge. Dr Pope says telemedicine would improve patient care and reduce costly re-admissions. His trust is monitoring diabetics at home using a simple system that works via their TV. "Patients love it because they don't leave home, pay for public transport or parking costs. We see them on our office computers, so it frees up space in the outpatient clinics. Our vision is that this will become the default way of seeing outpatients," he said.
Although the clinical and economic advantages are clear, experts say a sluggish uptake of telemedicine means the UK is falling behind other countries such as the US, Australia, India and China in exploiting them.
A report recently published by 2020health, a right-of-centre think-tank, said the Government must be more "proactive" and "drive" the roll-out of telemedicine across the country. A government study into telemedicine is expected to report next spring.
A Health Department spokesperson defended its record, stating: "We fully recognise the potential of telemedicine to save lives ... we are publishing standards for use across the NHS to enable different information and technical systems to work together ... We are also actively involved in developing international standards."
For some, the revolution cannot come quickly enough. Professor Richard Wootton, editor of the Journal of Telemedicine and Telecare, said: "We know that patients like it, and it has great potential to save lives and money. Why hasn't it happened in the NHS? NHS inertia is one reason."
While the potential of telemedicine in the UK is enormous, others are excited about its use in the developing world. Lord and Lady Swinfen set up the Swinfen Charitable Trust in 1998 with four British doctors volunteering to advise doctors in Bangladesh.
The trust now has 471 specialists worldwide, ready to help 199 hospitals in 60 poor countries to deal with complex cases. A laptop and a digital camera are provided to doctors who email referrals with attached scans and video clips. Working from home, Lady Swinfen, a former nurse, then sends the referral to the most qualified specialist. "This is terribly simple, but it has a global impact."
Additional reporting by Matt Thomas
Transforming care
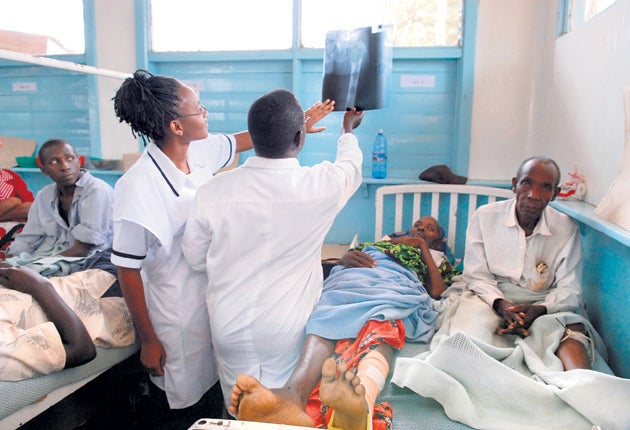
Telemedicine's benefits are seen most starkly in places such as East Africa, where technology can dissolve distances and bring medical expertise to an estimated 30 million people. Dr Johnson Mussomi, a Kenyan physician, says a PC, scanner and a digital camera can transform a hospital. Patients can be diagnosed, supplies ordered, and theatres prepared before specialists arrive. "To put it more simply, it saves lives," he said.
Airedale NHS Trust
For the past three years, doctors and therapists from Airedale NHS Foundation Trust in West Yorkshire have been seeing prisoners in the North-east using teleconferencing technology, for regular outpatient-type appointments for diabetes, heart disease and physiotherapy, and emergency consultations for sports injuries, stabbings and heart attacks. Dr Richard Pope, a diabetologist at Airedale, said: "I saw four prisoners from my office this morning – a couple will need to come in but the others don't, so that saves them the trip and frees up outpatient appointments. This is absolutely possible within the NHS."
Dean Wilcox
Dean, 22, from Rainham in Essex, was left severely disabled after a heart attack when he was 19 which starved his brain of oxygen. Doctors wanted an expert opinion from the National Hospital for Neurology and Neuroscience at University College London (UCL), because Dean was suffering from severe spasticity, or stiffness, in his arms and legs, making him increasingly uncomfortable and difficult to manoeuvre. He was assessed by a specialist doctor at UCL through a new teleneurology venture called NeuroResponse from his local hospital. His father, Kevin Wilcox, said: "The journey to London would have been a nightmare; Dean is not a good traveller, he gets car sick, and he would been really uncomfortable. The teleneurology was ideal, and it felt as if the doctor was in the same room."
Valerie Taylor
Ms Taylor, a British physiotherapist, founded the Centre for Rehabilitation of the Paralysed in Favar, Bangladesh, which inspired Lord and Lady Swinfen to set-up their telemedicine charity. Ms Taylor adopted her daughter Poppy, now 25, when she was five years old. Poppy has secondary dystonia, a congenital neurological condition. Ms Taylor sent a short video of Poppy, along with a description of her symptoms and medication, to Professor Victor Patterson, now a retired neurologist in Northern Ireland. "He was able to recommend a safe combination of drugs at the right doses. There was nowhere to turn here, so it was wonderful being able to email him with daily reports."
Yang Fu Bing
Abandoned when she was a few days old in January, she turned blue every time she cried and weighed only 4lbs. Karen Norman, an Australian registered nurse, works for International China Concern at an orphanage for children with disabilities in Hunan Province. There are no doctors at the project and the local hospital has little specialist knowledge. An ultrasound revealing the baby's heart defect was emailed to Dr Karen Rheuban, a paediatric heart specialist in Virginia, who has been providing long-distance help.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments