Cancer screening leads to burden of over-diagnosis
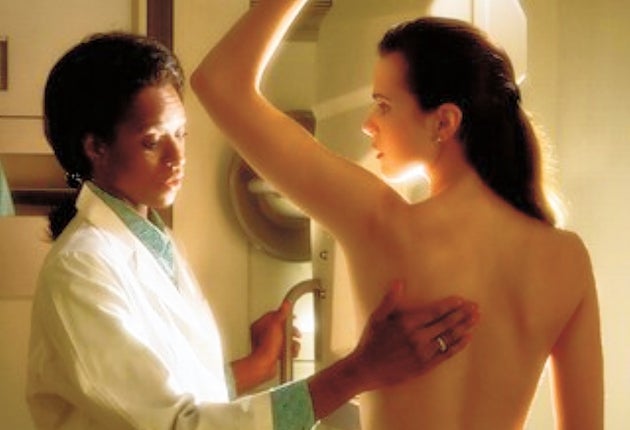
Screening programmes for cancer are leading to over-diagnosis of the disease, causing some people to live under the shadow of the diagnosis without gaining any benefit, specialists have warned.
In some cases, patients undergo unnecessary treatment causing pain and suffering in addition to the psychological burden of the diagnosis. The disease may be harmful, but so can the knowledge that a person has it.
The cancer detected in screening may sometimes not need treating, either because it resolves naturally or because it is very slow growing. In other cases, a test result may wrongly indicate the presence of cancer or identify a "pre-cancerous" lesion which never develops into a cancer.
A review of large randomised screening trials for a range of cancers shows that up to 25 per cent of breast cancers detected on mammograms and about 60 per cent of prostate cancers detected with the prostate specific antigen (PSA) blood test are over-diagnosed.
In a lung cancer screening trial, based on X-rays and sputum tests, half the cancers detected were overdiagnosed. More sophisticated techniques, such as spiral CT scans which provide more detailed pictures, found almost as many lung cancers in non-smokers as smokers. It is now recognised that it is better to ignore lung nodules detected by CT scans, most of which are non-cancerous.
Gilbert Welch and William Black from America's Dartmouth Hitchcock Medical Center, say in the Journal of the National Cancer Institute: "Whereas early detection may well help some it undoubtedly hurts others. Often the decision about whether or not to pursue early cancer detection involves a delicate balance between benefits and harms. Different individuals, even in the same situation, might reasonably make different choices."
For five cancers – thyroid, prostate, kidney, breast and melanoma – data from the past 30 years show an increasing number of new cases but not an increase in deaths. In each of these cancers, an increase in screening or imaging tests has been associated with an increasing rate of new diagnoses, they say.
The authors say education of patients about the risks and benefits of screening should be a priority. The threshold at which a screening test result is labelled "abnormal", or at which further steps are taken, could be raised. For instance, investigators could test whether it was better to ignore small abnormalities detected on imaging tests, as is now the practice with lung nodules.
In the case of the PSA test, two out of three men with a raised PSA will not have any cancer cells in their prostate biopsy. Conversely, up to one in five men with prostate cancer will have a normal PSA result. Even if cancer is diagnosed it is not necessarily life threatening.
The problem of overdiagnosis is so great with prostate cancer that routine screening is regarded as unwise in the UK though it is widespread in the US. In breast screening, overdiagnosis is a lesser problem so it is considered worthwhile offering it to women.
An editorial in the journal says the problem of overdiagnosis must be addressed. "What we need now in the field of cancer is the coming together of physicians and scientists of all disciplines to reduce the burden of cancer death and cancer diagnosis," it says.
Breast cancer screening
45,000 new cases diagnosed each year. Incidence has risen 50 per cent in the last 25 years.
12,000 deaths a year.
82 per cent of patients survive 5 years.
66 per cent survive 20 years.
50 per cent of deaths are in women over 70.
Death rates have fallen by a third since peaking in the late 1980s.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments