NHS crisis worsens after new figures show three-quarters of hospitals warned about dangerous staff shortages
Exclusive: New immigration rules can delay or even scupper visa applications from foreign-trained nurses
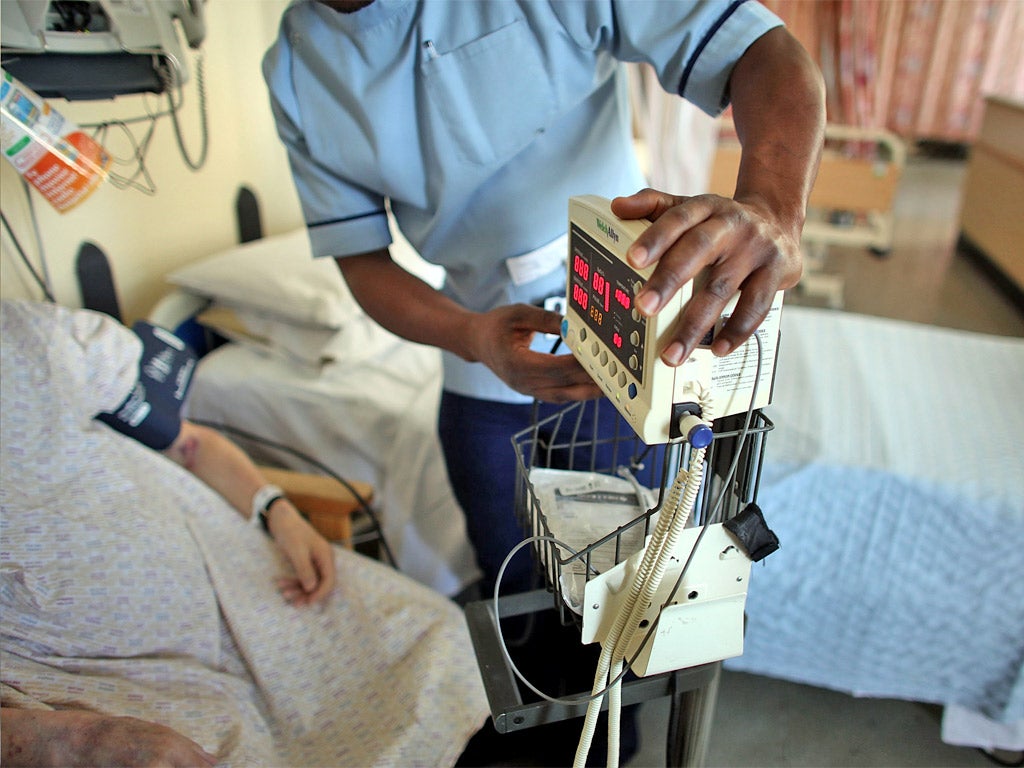
The severity of the staffing crisis engulfing the NHS has been revealed by new figures showing that three-quarters of hospitals have been warned about potentially dangerous staff shortages.
An analysis by The Independent of Care Quality Commission (CQC) inspection reports of acute hospitals from 2014 and 2015, found that of 89 hospitals, 68 had issues raised about short-staffing on one or more wards. In several cases, inspectors reported that staffing levels put patient safety at risk. Richard Murray, director of policy at the King’s Fund think-tank, said that tension between staffing and finances was now “the big dilemma affecting the NHS”.
The renowned Addenbrooke’s Hospital in Cambridge has become the latest to be branded “inadequate” by the CQC. Staff shortages in key areas, including critical care, were identified as being one of the chief problems.

Despite the warnings from inspectors, hospitals are under intense pressure to limit staffing costs to avoid going into the red. The whole hospital sector is anticipating a £2bn deficit this year.
In an effort to avoid an embarrassing bailout from the Treasury, the Department of Health has imposed a cap on spending on temporary agency staff and ordered hospitals to get a grip on their budgets.
Monitor, the financial regulator, wrote to hospitals last month to warn that financial plans for the year ahead were “unaffordable” and to only fill “essential” vacancies.
Meanwhile, new immigration rules mean that many hospitals that have turned to overseas recruitment in an attempt to staff their wards have found that visas for new nurses trained abroad have been delayed or rejected.
The NHS Employers organisation made a rare intervention earlier this month, warning the Government that if hospitals were unable to recruit nurses from outside the EU, it would harm their ability to meet safe staffing levels and provide effective care in the busy winter months.
Mr Murray said that, without new funding, hospitals may seek to reduce pressure on wards, admitting fewer patients and driving up waiting lists. He added that there was “real frustration” among managers about the dual restriction on agency staffing and immigration. Responding to The Independent’s analysis, Professor Sir Mike Richards said that judgements about safe-staffing could be based on numbers but also on skill-mix, and that staffing problems were often confined to areas such as A&E or maternity.
He said: “It’s not surprising to see staffing highlighted in so many of our reports, as it’s clearly a fundamental issue. The challenge for trusts – and ultimately for the NHS – is to get this right so that they can deliver safe and effective care to patients.”
The NHS has increased staffing numbers in recent years, as hospitals sought to improve safety in the wake of the Francis Report into poor care standards at Mid Staffordshire NHS Foundation Trust.
However, demand from an ageing and growing population, combined with cuts to council-funded social care that increase demand for hospital beds, have led to ever greater demands on staff. Janet Davies of the Royal College of Nursing said that attempts to “catch up” in the past two years had involved short-term measures, but that agency and overseas staff would be “absolutely crucial to get us through the coming winter and some years to come”.
Staffing and funding pressures on wards has led to widespread discontent among the NHS professions, with unions angry over pay proposals that will see public sector pay rises capped at 1 per cent a year.
Meanwhile, junior doctors have threatened strike action over a proposed new contract that could see their pay cut. On 21 September, The Independent revealed that, in a three-day period last week, 1,644 doctors had registered an interest in moving overseas.
Pressure on the Government over the junior doctor contract increased after the Royal College of General Practitioners (RCGP) said the proposals could undermine the Conservatives’ flagship election pledge to recruit 5,000 more GPs.
Dr Maureen Baker, chair of the RCGP, called on the Health Secretary Jeremy Hunt to make a “cast iron guarantee” that the contract would not see cuts to trainee GP pay.
A Department of Health spokesman said: “Making sure we have the right number of staff is vital, which is why we have prioritised and invested in the frontline. There are already more than 20,600 extra clinical staff, including 8,800-plus additional doctors and more than 7,100 additional nurses on our wards since May 2010. We know that the environment is tough but we are investing the additional £8bn that the NHS has said it needs to implement its own plan for the future.
“We are also supporting the NHS to employ the staff it needs at a fair price by introducing cost-control measures to clamp down on rip-off staffing agencies and we’re identifying billions of pounds to be saved through improved procurement and rostering.”
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments