Patients leave end-of-life care choice to medics, survey finds
The dying want to have a say - but few put on record how they want to be treated
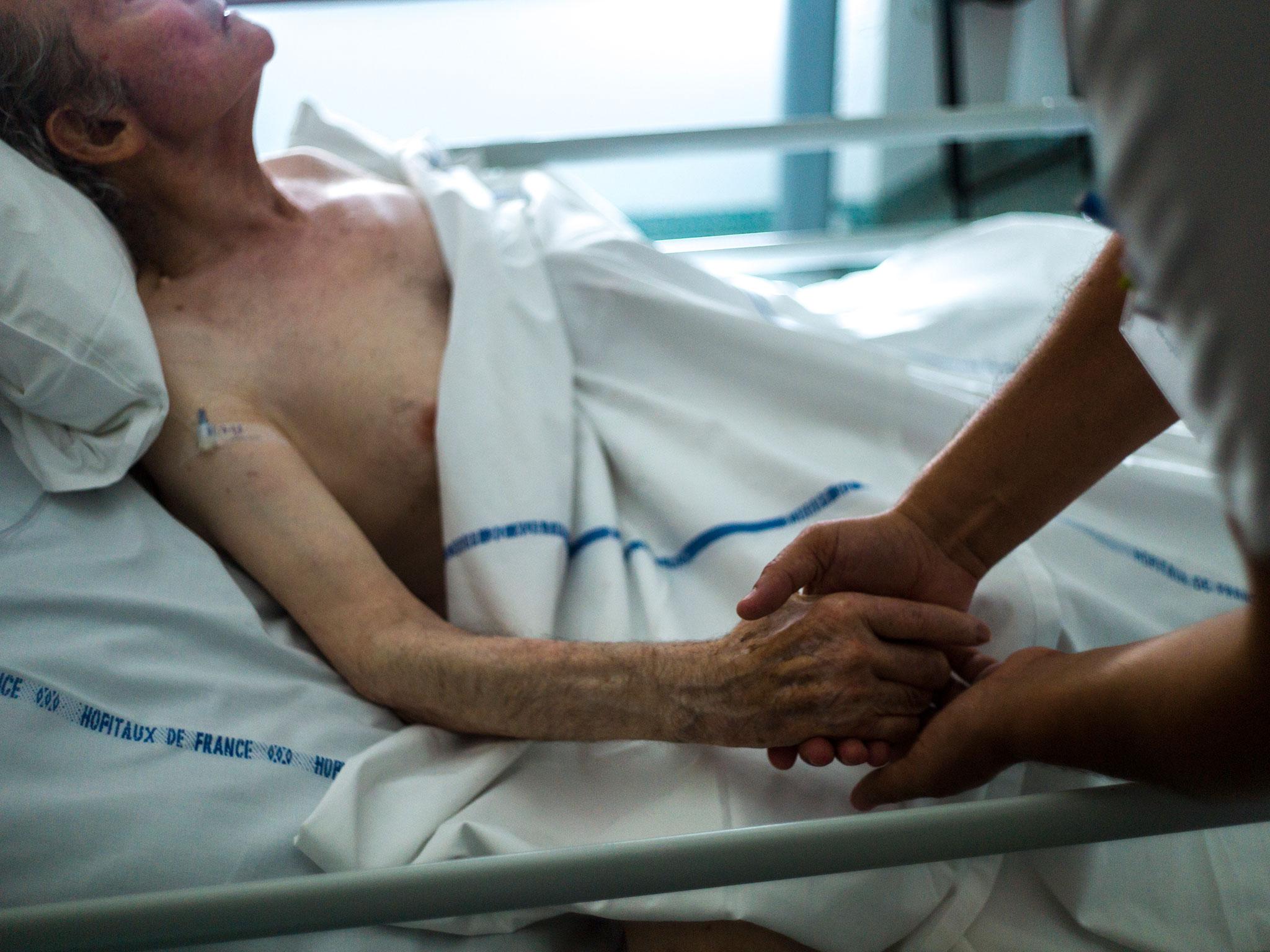
Major decisions about how people are cared for at the end of their lives are being left to doctors – despite fewer than one in 10 patients wanting this to happen.
Only 7 per cent of adults in Britain want a doctor to have the final say on their end-of-life care, according to research to be published this week. Despite this, only 4 per cent have either made a record of their preferences in an Advance Decision or appointed a Lasting Power of Attorney.
The research, by YouGov for Compassion in Dying, suggests the remaining 91 per cent have by default left these serious decisions to doctors, who may prolong their life against a person's wishes.
The charity says the Government should prioritise the issue of a "good death" and do more to make patients aware of their right to record their views on end-of-life care.
Davina Hehir, the policy director at Compassion in Dying, said: "The vast majority of people feel very strongly they should be in control of their own end-of-life care, or at least give the right for decision-making to an informed family member or friend. It will come as a surprise to most people that currently they do not legally have this right. It may come as a surprise too late for a patient to do something about it.
"It is vital that people communicate their wishes while they still have capacity. Doctors do a tremendous job of caring for people, but ultimately the patient should be able to say what they do or do not want in regard to their care.
"The Government needs to do more in prioritising end-of-life care and fully informing people about their end-of-life rights."
The findings come amid mounting evidence of a gulf between patients' wishes and the reality of dying in the UK. The Royal College of Physicians found in a recent audit that patients were not being fully informed about their end-of-life situation.
A Royal College of Nursing survey found that more than half of nurses reported instances where patients' wishes at the end of life were unable to be fulfilled. Anyone can complete an Advance Decision, a document that records what treatment – or lack of it – a person wants when dying if they lose the capacity to communicate with doctors.
Close family members or friends can also be appointed to have a Lasting Power of Attorney for health and welfare to make these decisions.
Esther Rantzen, a patron of the charity, said: "Being at the centre of your end-of-life care and being empowered to make your own decisions is hugely important in achieving a good quality of both life and death. However, all too often people aren't aware of their rights, and aren't supported to take the steps needed to make sure their wishes are respected. Understanding your rights and taking steps to plan ahead is vitally important to make sure you have the right experience for you at the end of life."
A Health Department spokesperson said: "We have commissioned an independently led review to provide advice on delivering greater choice and quality in end of life care." The review is expected to report early next year.
Subscribe to Independent Premium to bookmark this article
Want to bookmark your favourite articles and stories to read or reference later? Start your Independent Premium subscription today.

Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies