Study highlights dangers of IVF treatment overseas
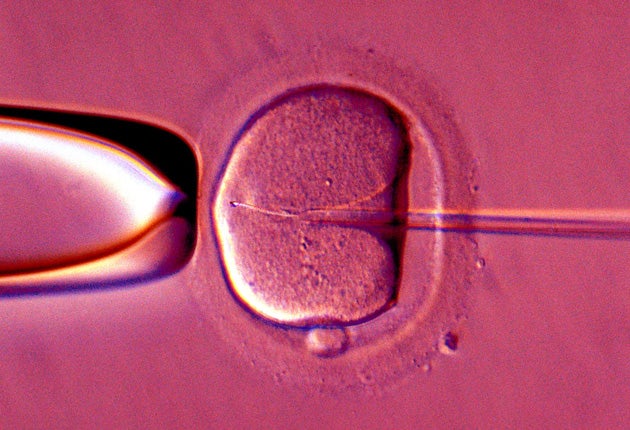
A global survey of fertility treatment covering more than 100 countries has revealed wide variations in international laws governing IVF which are fuelling the growth of "fertility tourism".
At least 10,000 people go abroad each year to seek help to have a baby because the laws are too restrictive in their home country or the cost of treatment is too high. No other field of medicine is subject to such wide differences in clinical practice, which are driven by social and religious attitudes rather than scientific evidence. Experts at the World Congress on Fertility in Munich will today announce a code of practice on cross-border care, to be published by the European Society of Human Reproduction and Embryology and the International Federation of Fertility Societies later this year. Professor Ian Cooke, education director of IFFS, said: "What is considered acceptable varies from country to country. How carefully do they screen donors? How do they screen for multiple pregnancies. Do you want to come back with quadruplet? That's madness." Both international organisations support the right of patients to go abroad. But they call for the harmonisation of national standards to increase safety.
From the UK, the chief reason for patients travelling is the shortage of egg donors, with waiting lists up to two years in some clinics. Favoured destinations are Spain and the Czech Republic where egg donors are paid €900 and €800 respectively. In Britain, regulations limit clinics to paying a maximum of £250 in compensation for lost earnings to egg donors.
Sperm donors are also in short supply in the UK, since donor anonymity was ended in 2005. Some couples travel abroad to obtain anonymous sperm.
Cost is also a factor, with an average price of more than £3,000 per cycle of IVF treatment in London. "It may well be cheaper to go to Barcelona or Prague and have a cycle of treatment there," Professor Cooke said.
Francoise Shenfield, co-ordinator of the ESHRE committee on cross-border reproductive care, said multiple pregnancy posed the biggest threat to patients. The UK restricts clinics to replacing at most two embryos in women up to the age of 40, but other countries allow up to four. Evidence shows multiple pregnancies carry higher risks for mother and babies.
"There is a striking difference between patients who had been abroad and those treated at home in terms of multiple pregnancies. Every clinic should have a strategy to reduce them," Dr Shenfield said.
Clinics wanted to improve their success rates and couples wanted an instant family. Cost savings were also a consideration. But the risk of prematurity and handicap increased in multiple pregnancies.
The global survey revealed the rapid expansion of fertility treatment around the world with over 500 clinics in India and more than 600 in Japan. In two- thirds of countries the practice is controlled by law or professional regulation but in a third it is uncontrolled.
In Catholic countries such as Spain, Italy and Poland, manipulation of embryos or experimentation on them is outlawed because of strict rules identifying the start of personhood with the moment of conception.
The donation of eggs and sperm is banned in Islamic countries. In Iceland, stored sperm must be destroyed when the donor dies. One third of countries ban surrogacy and this can create legal problems for couples who travel to a country where it is permitted and then return home with the child.
IVF laws: How fertility is controlled around the world
Germany
Freezing of embryos banned. Couples must produce fresh embryos for a second attempt with IVF.
France
Lesbians are not allowed access to donor sperm. In Norway, homosexuals can be accepted for infertility treatment.
Italy
a requirement that all embryos produced for IVF must be replaced in the womb was reversed earlier this year following a legal challenge that it was not best medical practice. Doctors in other countries select only the best embryos for replacement to increase the chances of success.
New Zealand
The requirement to consider the welfare of the child no longer means it must be raised in a nuclear family. The Maori idea of the family includes the practice of guardianship.
South Africa
bans surrogacy for non-residents. UK couples looking for a woman to carry their baby will be disappointed in this country.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments