The $15bn gamble to cure mankind of polio
After 25 years, a stunningly ambitious bid to eradicate a disease that once killed millions is within a few hundred cases of total victory. Can we finish the job?
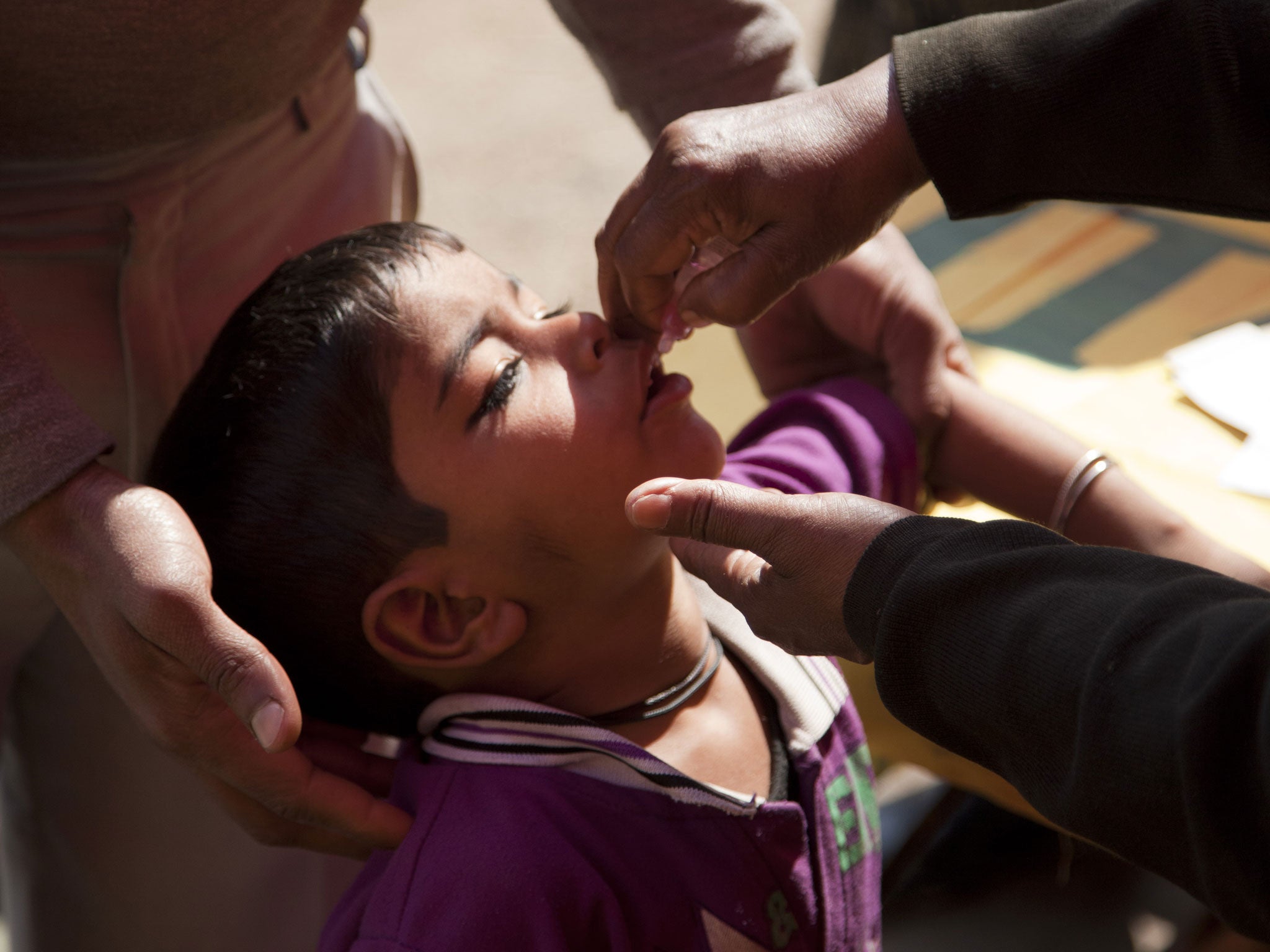
On a muddy street in the northern suburbs of Delhi dotted with neat piles of human excrement, barefoot children cluster round a white van temporarily converted into a mobile vaccination clinic. Sarita, a local health worker, squeezes two drops of a pink vaccine into their open mouths in what has become a $15bn gamble – to end polio and spare future generations the suffering it has caused.
At a meeting in Abu Dhabi next month, governments and bodies including the World Health Organisation (WHO), the Bill and Melinda Gates Foundation and Rotary International will meet to plan the final phase of a 25-year campaign against the nerve-destroying virus. If it succeeds, some say it will rank as mankind's single-most ambitious accomplishment.
The goal is tantalisingly close – after a quarter century of eradication efforts the number of cases has fallen more than 99 per cent – from 350,000 in 1988 to 222 in 2012. There are now just three countries where the disease is still endemic – Pakistan, Afghanistan and Nigeria –down from more than 125.
But there are major barriers in the way. Nine female polio vaccinators were shot and killed in northern Nigeria last month, and 16 vaccinators and clinic workers were killed in Pakistan before Christmas.
The killings are believed to be the work of terrorists spurred by religious leaders who have for a decade spread rumours that the vaccine is part of an American plot to sterilise all Muslims and wipe them out.
The fake CIA hepatitis vaccination campaign in Pakistan that helped to locate Osama bin Laden in 2011 and the disastrous failure of a meningitis vaccine trial in northern Nigeria that cost the US pharmaceutical company Pfizer millions of dollars in compensation have fuelled suspicions. Muslim leaders and WHO officials are set to meet in Egypt next week to seek a way forward.
But terrorism is not the only threat. Even worse is the threat of failure. So far the "End polio now" campaign is estimated to have saved five million cases of severe paralysis – a spectacular humanitarian achievement which has protected a generation of children from devastating disability and death. But the programme has cost at least $9bn (£6bn) – almost $2,000 for each case averted. By comparison, the total health budget for India for 2012 was less than $5 a head.
Experts have calculated that a further $5.5bn is required to finish the job – halting transmission in 2015 so the world can be declared polio-free three years later in 2018 – and Bill Gates is now seeking philanthropists to join the cause (Michael Bloomberg signed up this week with a pledge of $100m). The total means the cost per case averted is set to rise to $25m – and for the very last case it could be as high as $200m.
More lives might be saved by spending the money on other projects, such as improving sanitation. The Hindustan Times reported this week that 1,000 children a day are dying in India from diseases caused by water contaminated with sewage.
But to give up now and see the resurgence of polio would mean sacrificing the billions already spent. It would mean giving up on Sarita, and health workers like her who have spent the last decade and a half searching urban slums, and travelling to the most distant villages to bring the vaccine to every child.
Double or quits? That is the billion-dollar bet the world is being asked to make in a campaign that has become too big to fail.
Confidence that it can be done comes from India's success in eliminating the disease – the last case was recorded in 2011. In one of the most chaotic, densely populated and deprived nations on earth, that is an astonishing achievement. In a slum in the Madipur district of Delhi, Poonam shows how it was done. Squeezing through the narrow alleyways of the roughly hewn, illegally built houses, the neighbourhood worker pushes past dogs and children, dodging buckets of waste and ducking electric cables.
Clutching a ledger with names and addresses, she is accompanied by Mamta, who carries the insulated box containing the vaccine nestling on a bed of ice – half a dozen vials each enough for 20 children. The pair have 400 houses to visit over four days with a fifth day reserved for "mopping up" – revisiting those where children were missing or away. For this the neighbourhood workers receive a salary supplement of 375 rupees (£1 a day).
They begin knocking on doors, calling up to upper floors, summoning families by name or crying out "Polio drops". Dark-eyed children emerge from cell-like rooms – earth floors swept clean – ready for the drops. They are familiar with the drill by now – India has been doing this since 1995. Even though polio transmission has been halted here, there is the ever-present risk that it could be re-imported from elsewhere.
The secret of India's success is contained in a two-inch thick ring binder sitting on Dr Sucheta Bharti's desk, the vaccine co-ordinator for Madipur in the nearby maternity centre. This is the "microplan" – hundreds of pages of coloured maps that detail every corner of the district, with its allocated health workers. The yellow section marking the slum we have just visited contains 18,000 houses covered by 28 teams of vaccinators, each with their designated route.
Dr Bharti, dark ringlets falling either side of her face, is a fervent supporter of the polio eradication programme. "Each paralysed person is a burden on themselves and on society," she says. But she is already looking beyond it. "This is the only programme that has reached to every doorstep. We have the vital statistics [for the country]. We can use this for anything."
Top of her list is to expand the vaccination programme against measles, hepatitis and other diseases which critics say has been unfairly neglected. It is an aspiration shared by Bill Gates, the WHO and Rotary International, the first organisation to tackle polio on a global scale in 1985, who look forward to using the vaccination networks for "other life-saving solutions".
But driving polio out of its last reservoir will not be simple. The Independent Monitoring Board for the Global Polio Eradication Programme, chaired by England's former Chief Medical Officer , Sir Liam Donaldson, warns in its latest report that success is "far from assured".
"There is one vital ingredient that is still missing in the remaining endemic countries (Pakistan, Nigeria and Afghanistan) – absolute ownership: from parents demanding the vaccine and from local leaders grasping the challenge of wiping it from their areas," it says.
But the message has fallen on deaf ears. There is a reluctance to involve parents in running the programmes, Sir Liam says, and no enthusiasm for greater public access, such as by placing internet cameras in operations centres to allow people to see what happens.
"The programme is resistant to some of these ideas. They are very slow to respond," he said. Does he think polio can be beaten? "I do think it is feasible. But the final cases – squeezing the last one out – will be incredibly difficult."
The challenge: the final push
If history is any guide, the final push against polio will demand a superhuman effort. Past attempts to eliminate diseases have almost all failed. In his book Better, Atul Gawande recounts how in the early part of the 20th century billions of dollars were spent on successive campaigns to eliminate hookworm, yellow fever, yaws (which causes purulent skin ulcers) and malaria – all without success.
The shining exception was the battle against smallpox, eradicated in 1978 following a mammoth campaign that was, even so, much simpler than the one against polio. Smallpox is marked by a distinctive rash. When it occurred, a team could be dispatched to vaccinate everyone the victim may have had contact with, in a technique known as “ring immunisation.”
The same method is not available with polio because for every case of paralysis there are at least 200 who suffer, at worst, a fever and an upset stomach. They soon recover but remain silently contagious for weeks after their symptoms disappear. Ring immunisation would require a huge target area. And as the oral vaccine does not always “take”, especially in children with diarrhoea whom it may pass straight through, repeat vaccination is required.
Rotary’s role a £30m crusade
The first body to tackle polio on a global scale was Rotary International, the humanitarian organisation with 1.2 million members worldwide, drawn from the business and professional communities, whose motto is “Service above self”. In 1985, it launched a programme to immunise the world’s children against polio by 2005, its centenary. Three years later, it joined with agencies including WHO and UNICEF and national governments to form the Global Polio Eradication Initiative. Rotary UK has since contributed over £30m to polio eradication. Rotary International hosted The Independent’s visit to Delhi.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments