The hidden dangers of 'safe surgery'
Surgeons require 750 operations to perfect keyhole technique, study finds
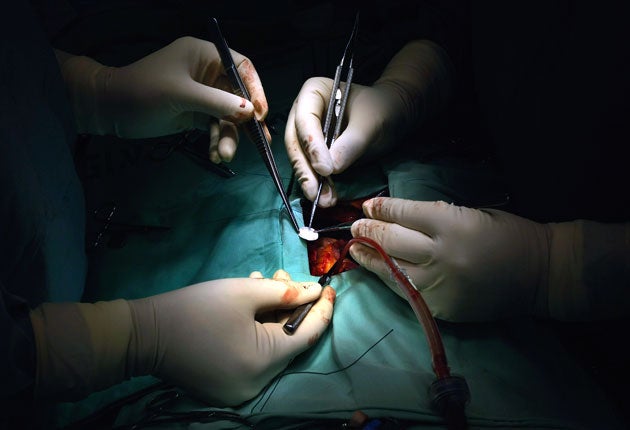
Surgeons may take as many as 750 operations to learn how to perform keyhole surgery safely. Those who used the keyhole technique took three times as long to acquire the necessary skills compared with the traditional open operation, a study has found.
No patient wants to be the first to go under the surgeon's knife but the discovery that it is wise to wait until the 750th place on the list will alarm those who find themselves at the front of the queue.
In keyhole surgery, the instruments are introduced via tiny incisions in the abdomen and monitored via a camera. In traditional prostate surgery, the abdomen is opened and the prostate gland exposed and surgically removed.
Keyhole surgery causes less pain and has quicker recovery times than traditional surgery but is harder to learn. Surgeons who began using the traditional technique and switched to the keyhole technique found the transition the hardest to make.
Researchers from the Memorial Sloan Kettering Cancer Centre, New York, said that the findings suggested that patients were better off being treated in specialist centres, where surgeons performed a large number of the same operation.
They added that, if the results were confirmed to be correct, "surgeons should not switch between open and laparascopic [keyhole] procedures without a compelling reason".
The study, published in The Lancet Oncology, was based on rates of cancer recurrence. Researchers monitored 4,700 patients operated on using keyhole techniques by 29 surgeons in seven hospitals in Europe and North America. The findings were compared with results from an earlier study of 7,700 patients who underwent traditional surgery. In both groups, patients were at increased risk of their cancer recurring if they were operated on by surgeons with less than the very highest levels of experience. For those performing the traditional operation, the chances of a recurrence dropped quickly with increasing experience, levelling off after 250 operations had been performed.
Keyhole surgeons had to carry out 750 operations, however, before they were able to achieve the same low level of disease recurrence. The sharp fall in recurrence rates with increasing expertise suggests that recurrence of the disease is "largely the result of limitations of surgical technique", the authors say.
"The only way to minimise the number of surgeons in the early part of the learning curve is to restrict the number who perform a particular operation. Clinical, educational and research initiatives are required in order to moderate the negative effects of the learning curve on clinical care," they add. *Screening for prostate cancer could more than halve advanced cases of the disease but would mean many men were treated unnecessarily, a study has concluded.
Cancer Research UK scientists, who studied 43,000 men given blood tests for prostate specific antigen (PSA) every two years, found that 54 per cent of cases of advanced prostate cancer could be avoided but that one in 10 men aged between 50 and 59 would be treated unnecessarily, rising to three in 10 aged 60 to 69.
Professor David Neal, of the Cambridge Research Institute, who led the study, said: "Overdiagnosis is a real concern. There is currently no way to tell whether a prostate cancer is aggressive or passive." The results have been published in the British Journal of Cancer.
Subscribe to Independent Premium to bookmark this article
Want to bookmark your favourite articles and stories to read or reference later? Start your Independent Premium subscription today.

Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies