The NHS must improve care for patients suffering from 'multimorbidity', says study
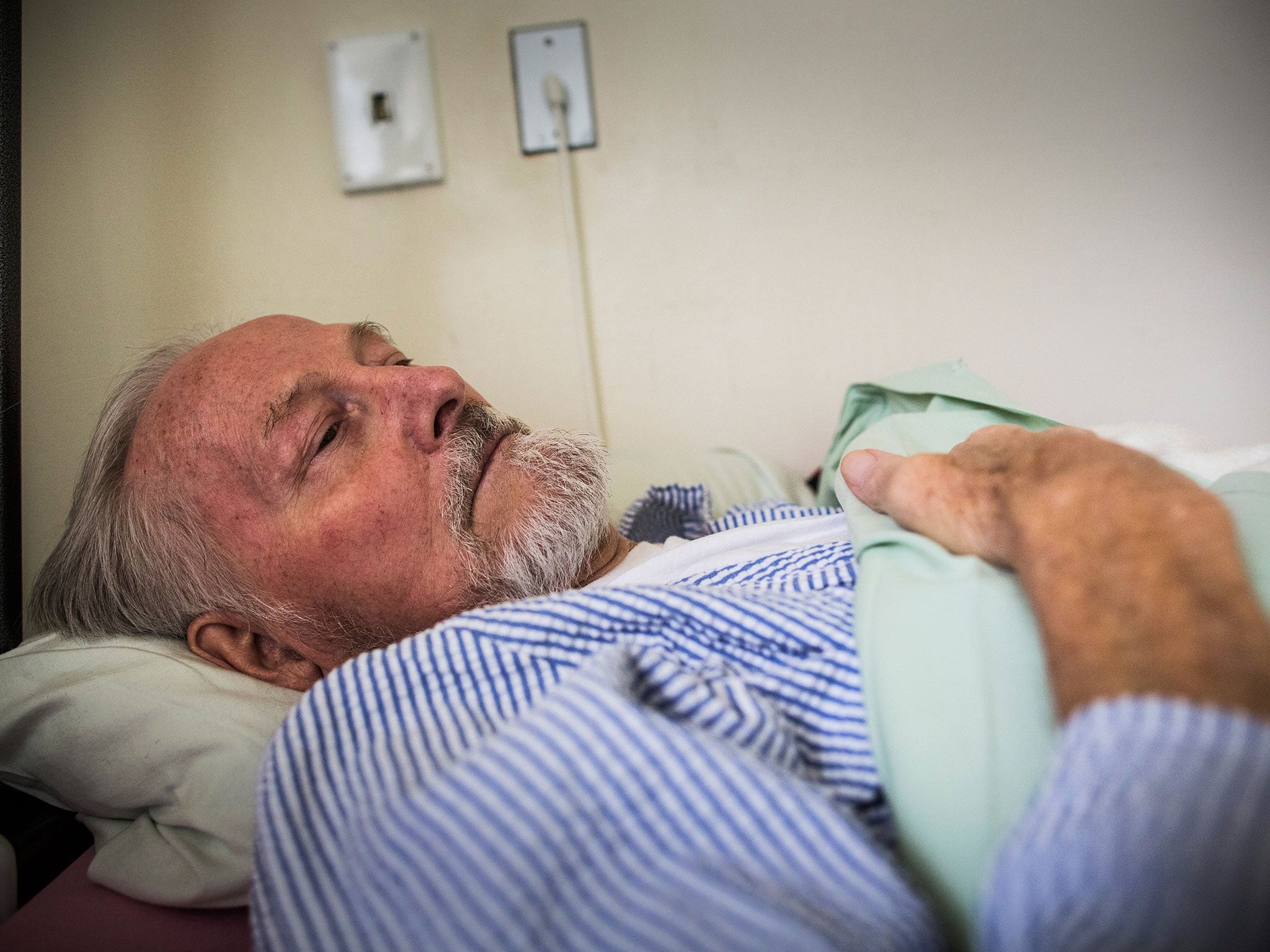
The study of nearly 40 patients in their final year of life found that some were taking as many as 10 medications a day
Patients simultaneously coping with more than one fatal illness face a “bewildering” range of treatments and services which are often poorly co-ordinated and impersonal, according to a study.
Researchers found that the National Health Service needs to improve the care it provides when patients who are entering their last year of life are suffering from multiple life-threatening illnesses dealt with by different hospital units and clinicians.
With life expectancy rising and the population ageing, the study warned that such “multimorbidity” will become increasingly the norm for the elderly in the last months of life and excessive burden was being put on carers and patients as they try to navigate the different services and difficulties presented by their conditions.
The study of nearly 40 patients in their final year of life, published in the journal BMJ Supportive and Palliative Care, found that some were taking as many as 10 medications a day and having to cope with the shifting demands of conditions ranging from lung cancer and renal failure to dementia and other neurological conditions.
One carer said: “There is no consistency in terms of seeing the same doctor all the time. So many changes, so many different doctors…. Each of them is very considerate but clearly clueless about the uniqueness of the patients.”
Carers and patients reported that support was often “impersonal” and “challenging” with doctors failing to grasp the difficulty of explaining multiple symptoms and conditions. The researchers suggested GPs need to provide “holistic” management of patients, noting that many patients put more emphasis on treatment aimed at maintaining the quality of remaining life.
The study said: “More and more of us will face many years living with multimorbidity: the challenge is to make those years as healthy as possible.”
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments