Malaria: The beginning of the end?
A discovery by British scientists has transformed the fight against the world's deadliest disease
You wait for years for a breakthrough in the battle against malaria, and then two come along in two weeks. But the advance announced yesterday by scientists at the Wellcome Trust Sanger Institute in Cambridge is potentially far more significant than last month's news of an experimental vaccine made by GlaxoSmithKline (and part-funded by Bill Gates), which showed partial success in early clinical trials. Scientists involved in those trials emphasised that the vaccine would only be able to contribute to the control of malaria.
The Cambridge scientists' discovery offers hope of something far more thrilling: the complete global eradication of the disease.
That tantalising goal is significantly closer, thanks to the discovery of the critical component of human red blood cells that appears to be vital for the malaria parasite to complete its lifecycle within the human body. In effect, the deadly parasite's "Achilles heel" has been identified.
This means that it should be possible to design a vaccine that blocks the parasite's development within an infected person – which, researchers believe, should prevent both the disease and its mosquito-borne transmission.
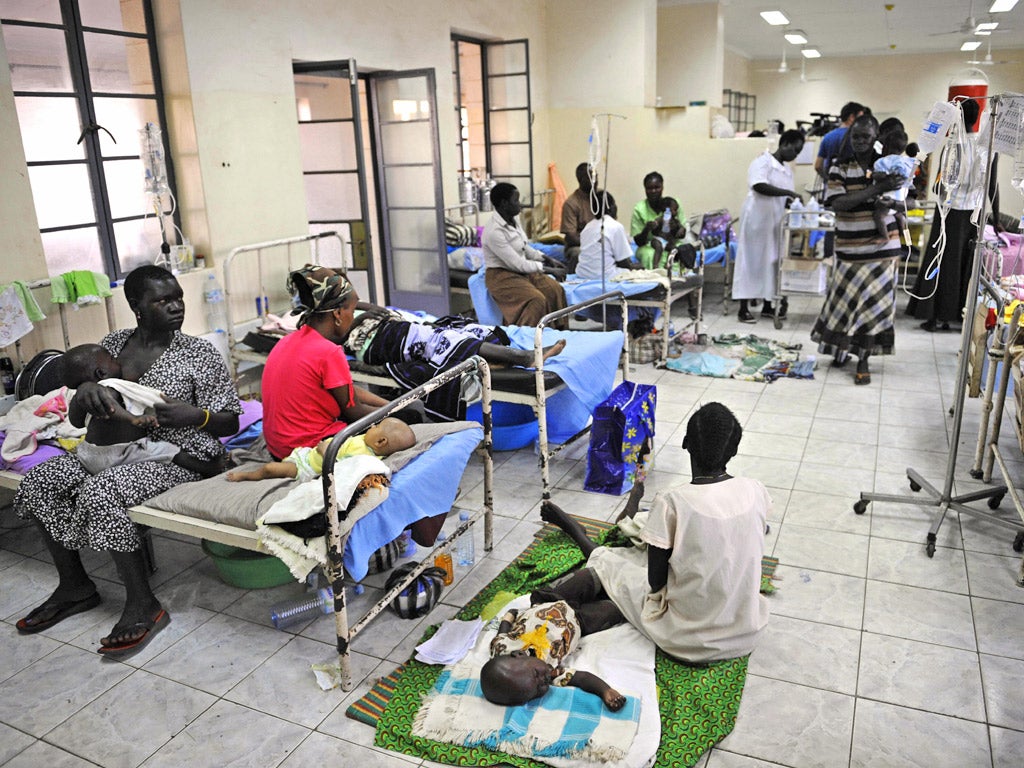
Malaria is one of the world's biggest childhood killers. Nearly a million people a year die from it, mostly children under five living in sub-Saharan Africa. Scientists have spent decades trying to devise vaccines which protect people against infection or can control the parasite's development once it is inside the body. However, the complexity of the parasite's lifecycle has frustrated the design of effective vaccines.
But now, said Julian Rayner of the Sanger Institute, the crucial protein "lock" on the surface of human red cells that allows the mosquito to insert its "key" and gain entry has been found.
"The interaction [between malaria parasite and red blood cell] that we have found has the potential to be the basis of a vaccine that would save millions of lives," Dr Rayner told The Independent. "This is possibly the most exciting vaccine target for the past 10 years."
The work behind the breakthrough, published in the journal Nature, focuses on the second phase of the malaria lifecycle in the human body, after it leaves the liver to invade the red blood cells during its "merozoite" stage.
Scientists at the Sanger Institute were able to identify a human protein, called basigin, on the surface membrane of the human red blood cells that the parasite appears to need to unlock the membrane and invade the cell.
"The malaria parasite shuttles between mosquitoes and humans. But the stage that actually causes the symptoms of the disease is where the parasite invades human red blood cells," Dr Rayner said. "It has to get inside a red blood cell to divide, spread and multiply – it's essential for the parasite's survival. But it's also a potential target for attack."
Once the scientists had identified the key protein "receptor" on the membrane of the red cells, they devised experiments to see if it was possible to block the interaction between malaria parasite and cell. They succeeded with antibodies designed to recognise and stick to the corresponding receptor protein on the parasite – blocking the "key" used by the parasite to unlock red cells.
"We can show that if we use antibody against the receptor we can completely block all detectable invasion by the parasite," said Gavin Wright, whose laboratory at the institute devised the techniques for making pure malaria parasite proteins. "We have done experiments where we've raised antibodies against the parasite protein and again we've shown very strong inhibition of the invasion process. As a starting point for vaccine development, you couldn't hope for better."
Professor Adrian Hill of the Jenner Institute in Oxford said the breakthrough could improve future vaccines.
"Reports of positive results from ongoing trials in Africa are encouraging, but in the future more effective vaccines will be needed if malaria is to be eradicated," he said. "The discovery of a single receptor that can be targeted offers the hope of a far more effective solution."
Case studies...
'By the time doctors caught it, it was too late'
Jim Thompson runs a building business in Banchory, near Aberdeen. His daughter Debbie died after contracting malaria during a visit to Zimbabwe. He has since raised thousands of pounds for Malaria No More
"Debbie went out to South Africa for a break before coming back to be a bridesmaid at a friend's wedding," he said. "She wanted to have a good time so she went to spend three or four months with her cousins. We think she contracted malaria in Zimbabwe. She went to a doctor in South Africa who thought she had tonsillitis or a virus. By the time they got her to hospital it was too late. She never came out of her coma. We think of her every day and we don't want anyone else to suffer what my wife and I went through. That's why fundraising is so important."
'The mosquitoes were in love with me'
Lisa Scappaticci, 27, a programme officer with children's charity Plan UK, contracted malaria for the third time while on a field trip to Burkina Faso in September
"It was the end of the rainy season so there were lots of mosquitoes and they were in love with me, especially my feet, so I got bitten a lot," she said. "I was taking anti-malarials but I recognised the symptoms: strong back pain, fatigue, nausea, headache, difficulty concentrating and strong stomach pain. It wasn't as bad as before, but I was very sick for three days and very tired for another week. I am OK but it is a terrible burden in Africa; a vaccine could save millions of lives."
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks