Half of GPs believe they cannot guarantee safe care to their patients
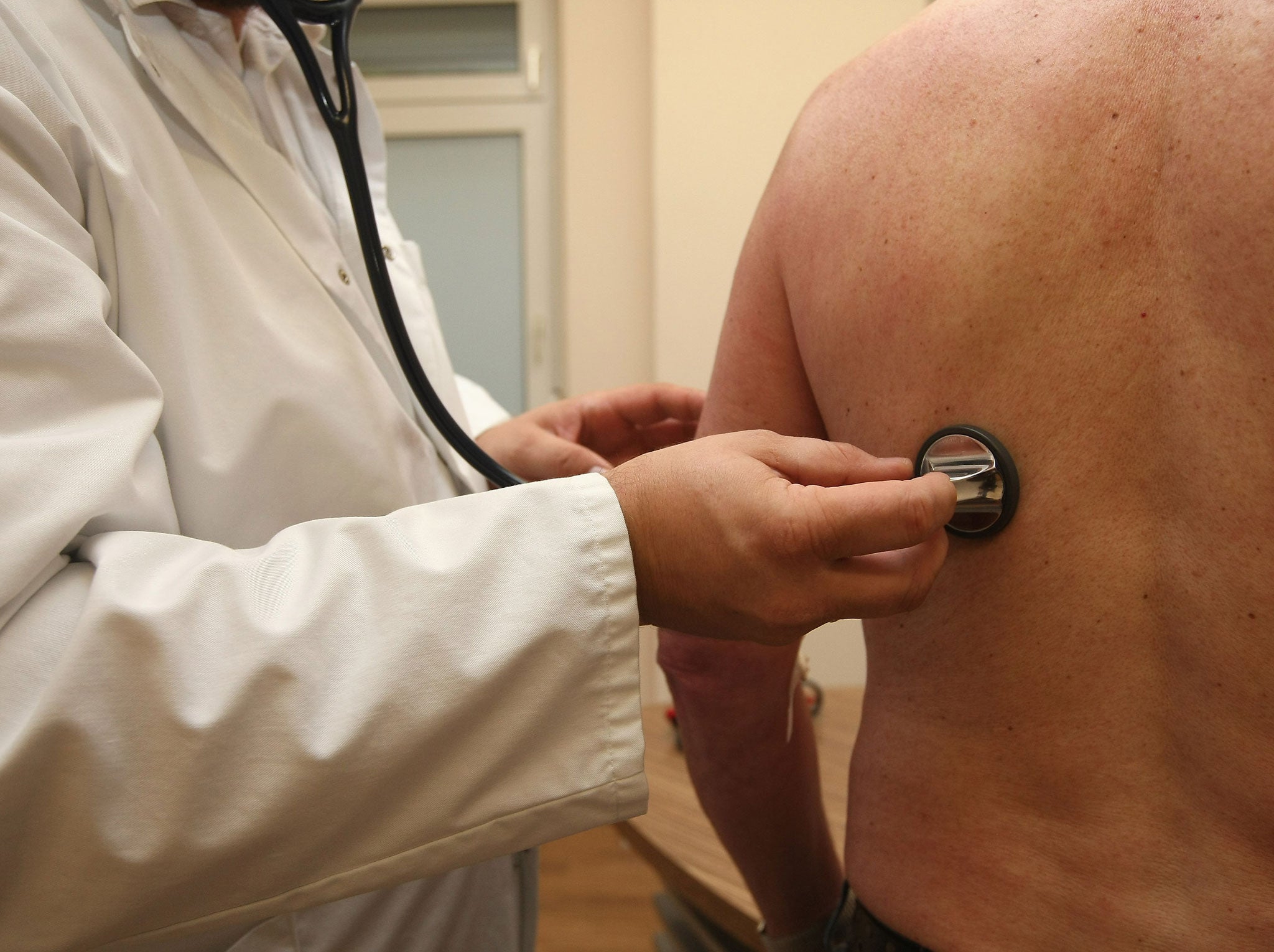
One in two family doctors believes that they “can no longer guarantee safe care to their patients” as pressures on GP practices countrywide continue to mount.
In a poll conducted the Royal College of General Practitioners (RCGP), 85 per cent of GPs said that their profession was “in crisis”, while 93 per cent said that working in general practice had become more stressful in the past five years.
The 2004 GP contract, which saw family doctors opt out of much of the out-of-hours care they once provided, has been blamed for soaring waiting times in A&E units by the health secretary Jeremy Hunt. However, 84 per cent of GPs said that their own workload had increased “substantially”. The Royal College is now calling for 10,000 new GPs by 2022, and a 10 per cent leap in funding for general practice.
The RCGP’s chair Dr Clare Gerada called the findings of the poll, of 258 family doctors, “truly shocking”.
“The findings… explode the myth, peddled by certain people in recent weeks, that GPs are somehow working less hard than other professionals across the health service,” she said.
“General practice has radically altered over the last five years, with ballooning workloads, and more and more patient consultations having to be crammed into an ever expanding working day – as the patient population grows older and increasingly suffers from an increasing range of ailments.”
Nine of out ten contacts the public has with the NHS are through GPs, but general practice only receives nine per cent of NHS funding.
The Department of Health acknowledged that GP surgeries had become extremely busy, while Labour said that doctors’ surgeries were “paying the price of David Cameron’s broken NHS promises.”
Relations between Mr Hunt and the powerful GP lobby were severely soured by his assertion that the 2004 GP contract, which saw family doctors hand over responsibility for much out-of-hours care to agencies, urgent care units and A&Es, had been “disastrous”. Leading doctors called his attack “childish and superficial”.
However, Dr Gerada appeared to offer an olive branch last week when she suggested GPs could take back responsibility for the round-the-clock care of a small number of patients who disproportionately require A&E and out-of-hours care, including the frail and elderly and those with complex health problems and those who require mental health services.
More than half of GPs said that they already worked until at least 7pm, and saw between 40 and 60 patients every day. Forty-six per cent said they spend at least 11 hours a day in surgery.
“Patients are now struggling to get appointments and GPs are forced to juggle the needs of fifty patients per day,” said Andrew Gwynee, Labour’s shadow health minister. “Ministers must put in place a plan to stop the deterioration in primary care services. Patients are paying a high price and they deserve better.”
An NHS England spokesman said: “General practice makes an enormous contribution to people’s health and well-being. We also know that the majority of people rate their overall experience of their GP practice as good and they have confidence and trust in their GPs. However we recognise that the way primary care is delivered is changing and that a complex range of factors are causing pressures on GP services. We want to explore with the profession how we can best enable GP practices to continue to provide a quality service and we look forward to working with the RCGP to identify how best to achieve these goals."
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments