Dispatches from the Ebola zone: The traumas and successes of working in a Sierra Leone treatment centre
Behind the biohazard suits and masks in West Africa are volunteers who daily face the horrors of the disease and with the emotional consequences. One of them is Dr Javid Abdelmoneim from London, who writes here of his experiences

Ebola scared me. All summer I’d been procrastinating about going to West Africa. Then I got an email from Médecins Sans Frontières (MSF) which said: “We’re desperate” – something that had never happened before. I needed a nudge and that worked. So I said okay, though it would mean losing my holiday to Ibiza and missing my friend’s wedding.
Working in Haiti during the cholera epidemic was the first time I had ever been exposed to suffering on a large scale – wanton, unchecked, avoidable human death. In Sierra Leone, again, I was expecting to be emotionally harrowed and to see lots of people dying alone. I knew it would be traumatic, but I believed that this time I could deal with it.
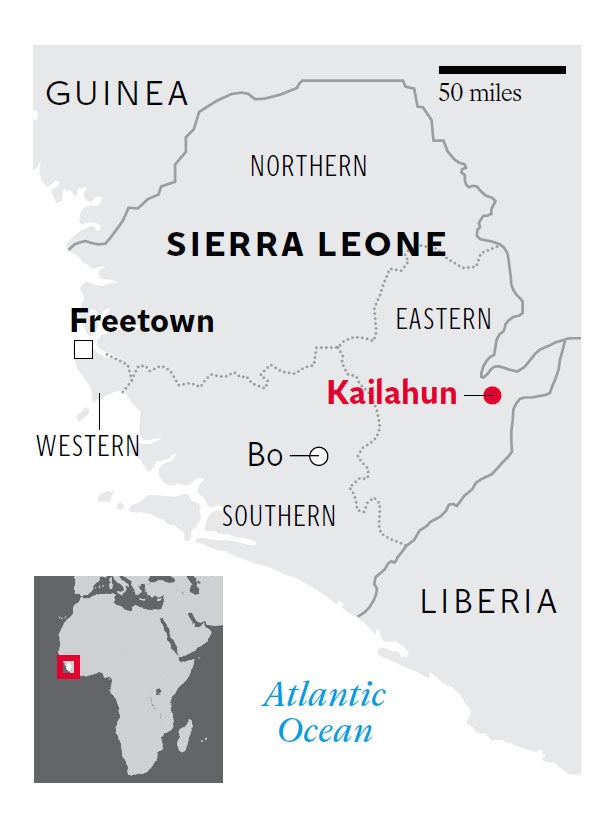
At our treatment centre in Kailahun, in the east of Sierra Leone, ambulances crammed with up to eight patients arrive every evening from districts such as Bombali and Tonkolili, having travelled for eight or 10 hours – which doesn’t include getting lost or getting stuck in the mud on the way. The journey time is long because, even now, there are just three or four treatment centres open in the whole country. And most districts have just two ambulances for hundreds of thousands of people.
One night I opened the ambulance door to find three people inside – a dead woman and two patients who were alive but who were now definitely cross-contaminated. They must have watched this poor woman die a wretched death, and now they were probably expecting to die this way too. And if the woman’s body rolled out of the ambulance, I would have had to leave it to fall to the ground because it was a biohazard.
The patients who are going to die from Ebola usually die quickly. They are already moribund, they have no energy to talk – to all intents and purposes they are a body on a bed. You attend to their suffering and administer painkillers, but you don’t get to know them as people. And maybe also you protect yourself emotionally: you know this person is going to die and you don’t let yourself get too close. Why get attached if you are only going to get hurt?
You can rarely be there to hold the hands of those who die from Ebola – and that’s dreadful – but at least you can sedate them and make sure they have no pain at the end; that’s the best you can do.
But it’s different with survivors. The patients who are going to survive have got a bit more energy, even at the beginning. The average time between being admitted and being cured is 15 days – so you have about two weeks to get to know them.
In the first few days, patients go through the awful “Ebola dip” – they are listless and lethargic, with no energy or appetite – even if they wanted to eat, they couldn’t lift a spoon to their mouths. They’re so weak that they can’t even stand up, and they wet themselves and vomit on themselves. You just have to hope that, with good nursing care, you’ll be able to help them through that day and the next.
After four or five days, their immune systems kick in. A patient lifts his head up and says, “I’m hungry”, and you think, it’s okay, he’s going to survive. Recovering Ebola patients have got voracious appetites – I’ve never seen anything like it. Soon they’re calling out your name across the fence when you arrive in the morning and the children are asking you to bring them toys.
I watched this happen to John. When I first met him he was bedridden, with severe pains all over his body. He had oral thrush, which made it painful to swallow and left a horrible taste in his mouth. He wouldn’t eat, and was under-nourished and emaciated. I managed to get him stronger painkillers, and brought in medication from MSF’s other Ebola centre in Bo, and he started to recover. John told me that he had lost both his parents and three of his brothers to Ebola, but his wife and child were waiting for him at home. When I left Kailahun, John was getting stronger by the hour, and I knew that he would soon be discharged.
I came home feeling elated, filled with a really strong sense of achievement. But the elation was short-lived.
First there was the upsetting stigma to deal with – friends I have known for more than 20 years refusing to even see me for 21 days. Then, when I was back working in A&E, there were people with little wrong with them, complaining that they’d waited for two hours and hadn’t been given a cup of tea, and I wanted to scream at them: “This isn’t a restaurant. You have no idea of how good you have it.”
For 40 years, the West ignored Ebola because it only affected people from Africa. Having finally woken up to Ebola, research institutes and drug companies have swung into accelerated action, with three treatment trials about to start in West Africa. We’ve learnt the lessons for Ebola very painfully; at the very least I hope we will apply these lessons to the other neglected killer diseases, like Ebola’s cousin, Marburg, and less bloody but equally fatal infections like multidrug-resistant TB. If, as humanity, we finally change our approach to diseases of the poor as a result of this horror, then perhaps people will not have died completely in vain.
Dr Javid Abdelmoneim is a London-based A&E doctor who has worked in crisis zones with Médecins Sans Frontières since 2009, working in Iraq, Haiti, Lebanon, South Sudan and most recently Sierra Leone.
‘Panorama: Ebola Frontline’ will be shown tonight at 10.35pm on BBC 1.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments