The <i>IoS</i> Christmas Appeal: First cholera. Now it's malaria and anthrax
Our special correspondent reports from Mashonaland West, where Zimbabwe's hard-pressed doctors are doing all they can to stop the spread of disease
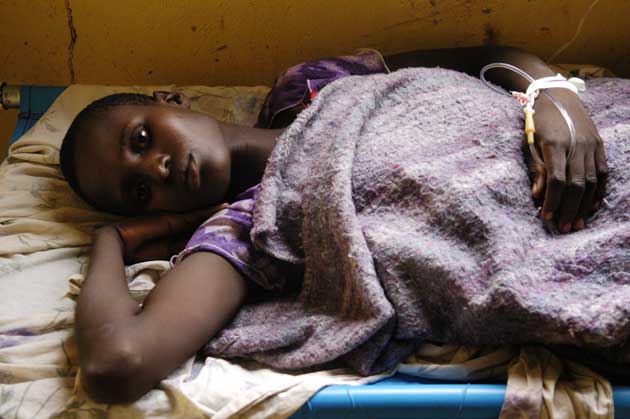
The folding bed on which the cholera patient lay was the only piece of furniture in the room. The bag of 5 per cent dextrose fluid going into her arm had to be tied to the metal window frame, in which half the panes were broken, because the isolation camp had no drip stands. But 19-year-old Kitty was fortunate, in more ways than one.
The high-school student was the only cholera patient in the camp, set up in two derelict brick houses in a remote area of the Zambezi River valley, to have a bed. Other patients had to lie on the floor, with just a blanket between them and the bare concrete. Save the Children had donated two special cholera beds, which can easily be disinfected between patients, but a 60-year-old woman had died in the other one earlier in the day. Her body lay on the floor in another room, wrapped in blankets.
Cholera is extremely infectious – Kitty and her grandfather, also a patient in the camp, had both contracted the disease at the funeral of another victim – but easily treatable if caught in time. "I feel better already," said the young woman, just over 12 hours after she was admitted. Nobody had the heart, however, to tell her that her grandfather was not expected to last the day. Like many older patients, he had suffered kidney failure, caused by acute dehydration.
It is a measure of Zimbabwe's collapse under President Robert Mugabe that cholera has been allowed to get out of control. Last week his government finally stopped playing down the worst epidemic in decades, and declared a national emergency. More than 12,000 people have been infected, and nearly 600 have died, according to official figures, but health professionals believe the real totals are much higher. Food shortages and economic collapse have crippled the country's health services so badly that many unrecorded deaths are thought to have occurred in remote areas, beyond the reach of treatment.
Nor is that the only reason why the disease has taken hold. In several cases, starving rural people have failed to report suspected cases of cholera, because they know that the authorities will immediately ban public gatherings, and wrongly believe that this will extend to food distributions. Only when victims start dying does the news get out, and by then infection has spread far and wide.
Cholera is endemic in parts of Mashonaland West, and there are well-established procedures for dealing with the disease, which usually makes its appearance much later in the rainy season, in March or April. Isolation camps are immediately set up at the scene of an outbreak, and are not closed until 14 days after the last case is declared over. But one rural doctor said there was simply not enough food for the staff, let alone the patients, to set up the number of camps required in his area. "We are just firefighting," he said.
Steady rain was falling as we arrived at Kitty's isolation camp, set up next to a clinic that had never been completed, because desperate local people had stolen building materials to sell for food. Before entering, we had to retie our shoelaces to ensure they did not brush the floor, and afterwards our shoes were disinfected. Only a timely donation of maize meal from Save the Children had allowed this camp to stay open, but Kitty's luck did not end there.
Unlike one family, in which a woman lost her mother and three of her four children in two days, the 19-year-old had recognised her symptoms straight away, and when she arrived, the camp had enough intravenous fluids and antibiotics to treat her. The doctor said he knew of at least two cases of patients dying because supplies of fluid had run out, and after the first few cases, the local laboratory had exhausted its supply of the reagents needed to test patients for cholera. "I must be the most frustrated doctor in Zimbabwe," he said.
If anything, conditions are even worse in the urban areas. Roughly half the deaths have been in the capital, Harare, where sewage runs down the streets in many poor districts. The water supply has been cut off to much of the city, because the municipality cannot pay for the chemicals to treat it. With monthly salaries for medical staff barely covering the cost of a single day's bus fare to and from work, all Harare's hospitals have ceased functioning. Last week riot police broke up a demonstration by doctors and nurses demanding better pay and conditions.
Even if a massive infusion of international aid brings the cholera outbreak under control, however, doctors fear that an equally fatal epidemic of malaria will soon follow. In a tropical country such as Zimbabwe, some cases of malaria can be expected every year. But in the low-lying Zambezi Valley there used to be a network of modestly paid community health workers who would cut the grass in which mosquitoes breed, and spray each house ahead of the summer rains, helping to keep the disease under control. That system broke down a couple of years ago, and the number of cases shot up last summer. With this year's rains, the sitation is expected to be even worse.
Another deadly disease, anthrax, has already made an appearance in north-western Zimbabwe, and has spread from animals to humans, because hungry villagers have eaten the meat of infected cattle. At least three people have died in the worst anthrax outbreak since the liberation war of the 1970s. More deaths are likely, because administrative disarray means the strict quarantine and slaughter system needed to defeat the disease is unlikely to be implemented. Inoculation of livestock against the disease all but stopped five years ago.
All these health disasters are on top of the ravages of HIV/Aids. Zimbabwe has one of the highest infection rates in the world, but progress was being made. Thanks to huge efforts by the Global Fund, anti-retroviral drugs have been widely distributed, but they are ineffective unless the person taking them is adequately fed.
In every case it is the children who are most vulnerable. David and Tambu's nine-year-old daughter Sarah showed symptoms of cholera at 4am, and by the same evening she was dead – probably, according to a doctor, because she was undernourished and had latent malaria as well. "She had been playing with children from a village where there was cholera," said David, who carried Sarah on his back for three hours to reach the nearest clinic. "We all went to church on Sunday, and on Monday she was dead. If the clinic here had still been running, perhaps she might have lived, but it closed a long time ago."
For Tambu, who was heavily pregnant with another child, the cruellest blow was that her daughter's body was returned to them encased in heavy plastic, to prevent infection. "If I had at least been able to see her one more time, it would have helped me grieve," she said. "I don't know how to tell the other children what has happened." Her fears for the family are growing, because they are dependent on food handouts. "We have traded our cooking pots for something to eat, and have nothing left to barter with," she said. "If no more food comes, we will die."
The doctor, who had been unable to save Sarah's life, said: "Cholera, malaria and deaths in childbirth are all easily preventable. Save the Children is a very strong pillar for us – compared with other districts, we lose far fewer people to these causes." Never, though, have the ordinary people of Zimbabwe been in greater need than now, and we are their only source of hope.
Some names have been changed
Anatomy of a killer
* Cholera, a bacterial infection, results from poor hygiene and contaminated water or food. It is common in crowded, insanitary environments, such as pre-20th-century London.
* One of the earliest breakthroughs in public health came when a cholera outbreak was traced to an infected well in Soho, London, in 1854.
* The disease causes massive diarrhoea and vomiting in its most virulent form, leading to dehydration and kidney failure. It can kill in as little as three hours if not treated.
* Cholera is easily treated by oral rehydration and antibiotics. But the disease will kill more than half those infected if left to run its course.
How you can help
Our Christmas Appeal has already raised over £10,000, but much more is still needed.
£5 will buy a mosquito net to protect a child from malaria.
£40 will buy a kit to treat a cholera patient with a drip, fluid and drugs.
£66 will build a safe toilet to prevent disease spreading.
£230 will fund a borehole and water pump so a village has clean water.
£660 will set up an isolation camp to treat cholera victims safely, and stop the disease from being spread.
You can also pledge at www.independent.co.uk/iosappeal
Subscribe to Independent Premium to bookmark this article
Want to bookmark your favourite articles and stories to read or reference later? Start your Independent Premium subscription today.

Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies