Stop laying into GPs. We don't deserve it
GPs are used to being scapegoated, but I cannot sit back and allow my profession to be held responsible for the problems in A&E as a result of opting out of out-of-hours care
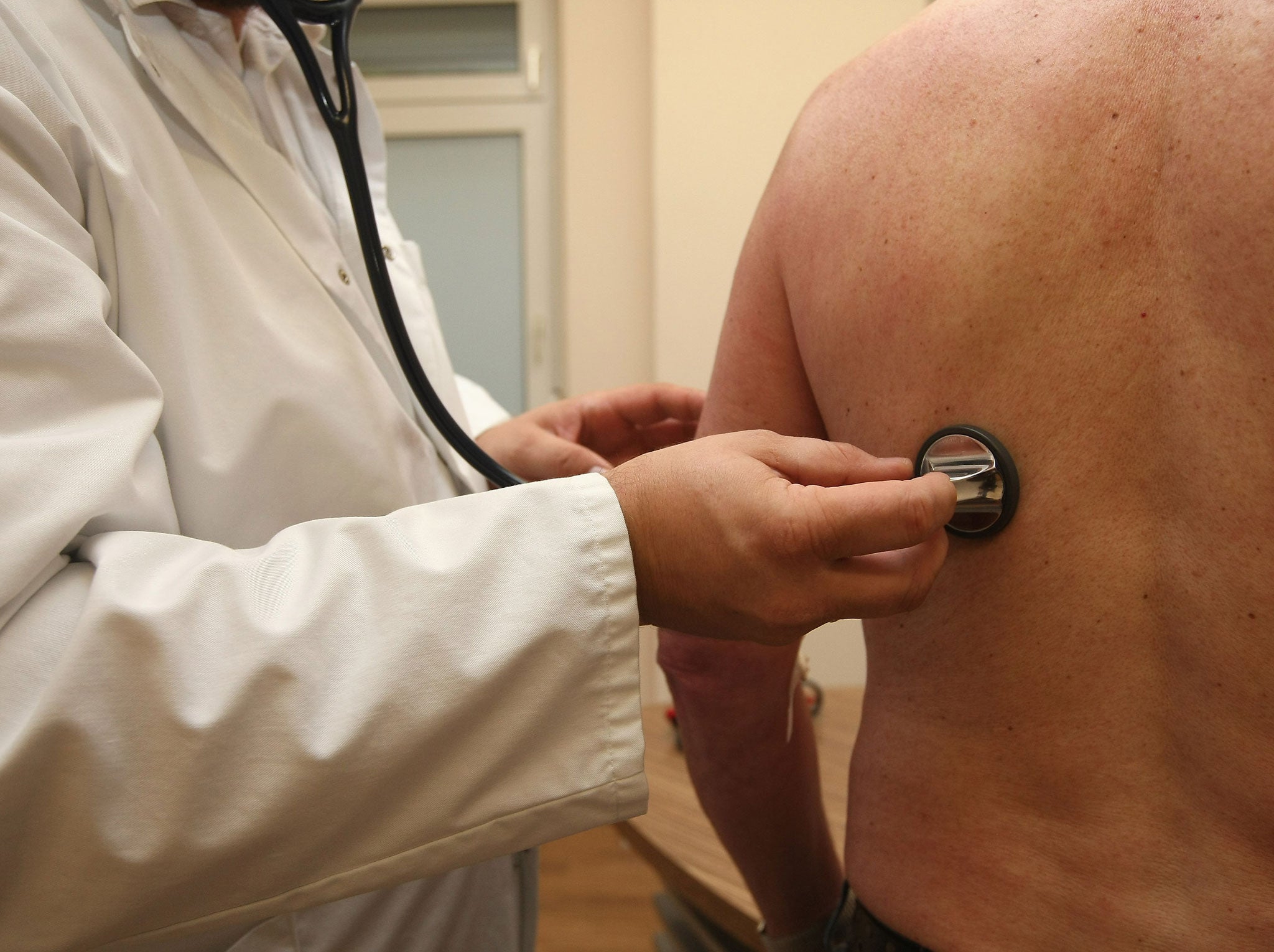
More than one million people across the UK will visit their GP practice today. Yet we GPs are being portrayed as lazy, uncaring doctors who spend all day twiddling our thumbs and abandoning our patients at 5pm sharp. This is not true and it is doing a great disservice to general practice and to our patients.
GPs are used to being scapegoated, but I cannot sit back and allow my profession to be held responsible for the problems in A&E as a result of opting out of out-of-hours care nearly 10 years ago. There are numerous reasons why our colleagues working in emergency departments (ED) are currently under pressure – but GPs are not one of them. Indeed, the Department of Health’s own data has shown that ED attendances have actually been relatively stable over the last few years, and in fact in London have decreased slightly. Overall, ED has experienced around a 1 per cent increase year-on-year in attendances, in line with population increases.
There was a sharp jump in recorded attendances before the 2004 contractual changes, and this continued immediately afterwards. But this was due to changes in recording, and to less serious work being carried out in minor injury services and GP-led services located in the emergency department (yet coded as an ED attendance). This accounts for the “massive” increase in ED attendances.
There is no evidence to suggest that access to GP out-of-hours services is poor. Nearly 80 per cent of patients responding to the GP Patient Satisfaction Survey (GPPS) rated the “ease of contacting the out-of-hours GP service by telephone” as “very easy” or “fairly easy”. Some 82 per cent of patients said that they “definitely” or “to some extent” had confidence and trust in their out of hours clinician.
Of course improvements can be made and we must look at ways of doing so. But GPs have continued to provide out-of-hours care, and changes to our contracts have meant that most practices now offer extended hours while continuing to provide out-of-hours care through GP cooperatives, walk-in clinics and, more recently, urgent care centres. Today over 90 per cent of all activity – in and out of hours, urgent and routine care – is undertaken by GPs and their teams.
Throughout the A&E debate, GPs have also been constantly criticised for being “overpaid and not working hard enough”, and I think it’s important here to bust a few myths once and for all. General practice is becoming increasingly challenging and complex – we have an ageing population and patients who present with more complex and multiple conditions. It is this epidemic of chronic and complex diseases that is placing the biggest pressure on our health service, and management of such conditions for their patients is what GPs do best.
GPs have seen consultation rates explode in recent years and family doctors are now facing ballooning workloads with record hours being worked in surgeries. We routinely see up to 60 patients on a daily basis whereas even 10 years ago this would happen only in exceptional circumstances, such as a flu outbreak.
GPs make the NHS safe and effective and we represent incredible value for money. Our patients still trust us more than any other professionals in the NHS. A year of care by a GP practice for one patient is around £100 to £150 – equivalent to one or two attendances at the local emergency department and less than one 999 ambulance call out.
So, what’s the answer? Going back to 2004 when GPs were working unsustainably long hours, often to the detriment of their own health, is simply not an option. It is neither affordable, nor logistically feasible and there is no evidence to suggest that it will improve care for patients. Patient needs have changed and the challenges we face are different. Patients do not want tired GPs doing night shifts and then not being available for consultations the next day.
We need to find a way of addressing the problems of continuity of care, in and out of hours, and in and out of hospital while ensuring that we provide accessible urgent care for all. A mixed model is needed to provide this, with GPs and other practitioners playing their equal part. A fully functional and properly funded NHS 111 service will help address the confusion about which service to call out of hours and should provide a single point of contact that sits between GP in-hours services and A&E.
We need to ensure the system works smoothly for individual episodes of care, where patient access to appropriate services generally takes priority. But at the same time, we need to ensure the growing number of people with long term conditions – who need on-going support rather than single episodes of care – are able to rely on a joined up system that delivers continuity of care. At the moment there is a lack of integration and continuity, with many different access points for urgent care. What we need to do is to simplify access and ensure that there are bespoke solutions to special populations, such as the frail elderly and those at the end of the lives.
I am thick-skinned but it has been really difficult to witness the vilification in the media and elsewhere of hard-working GPs who are doing their best for their patients. With greater investment and support – including more doctors – we can do even more. GPs are the solution to problems in the NHS, not the cause.
Clare Gerada is chair of the Royal College of General Practitioners
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks