What the final months of my mother’s life revealed about the NHS
Is the service showing sufficient care in the way it treats the information it has on patients?

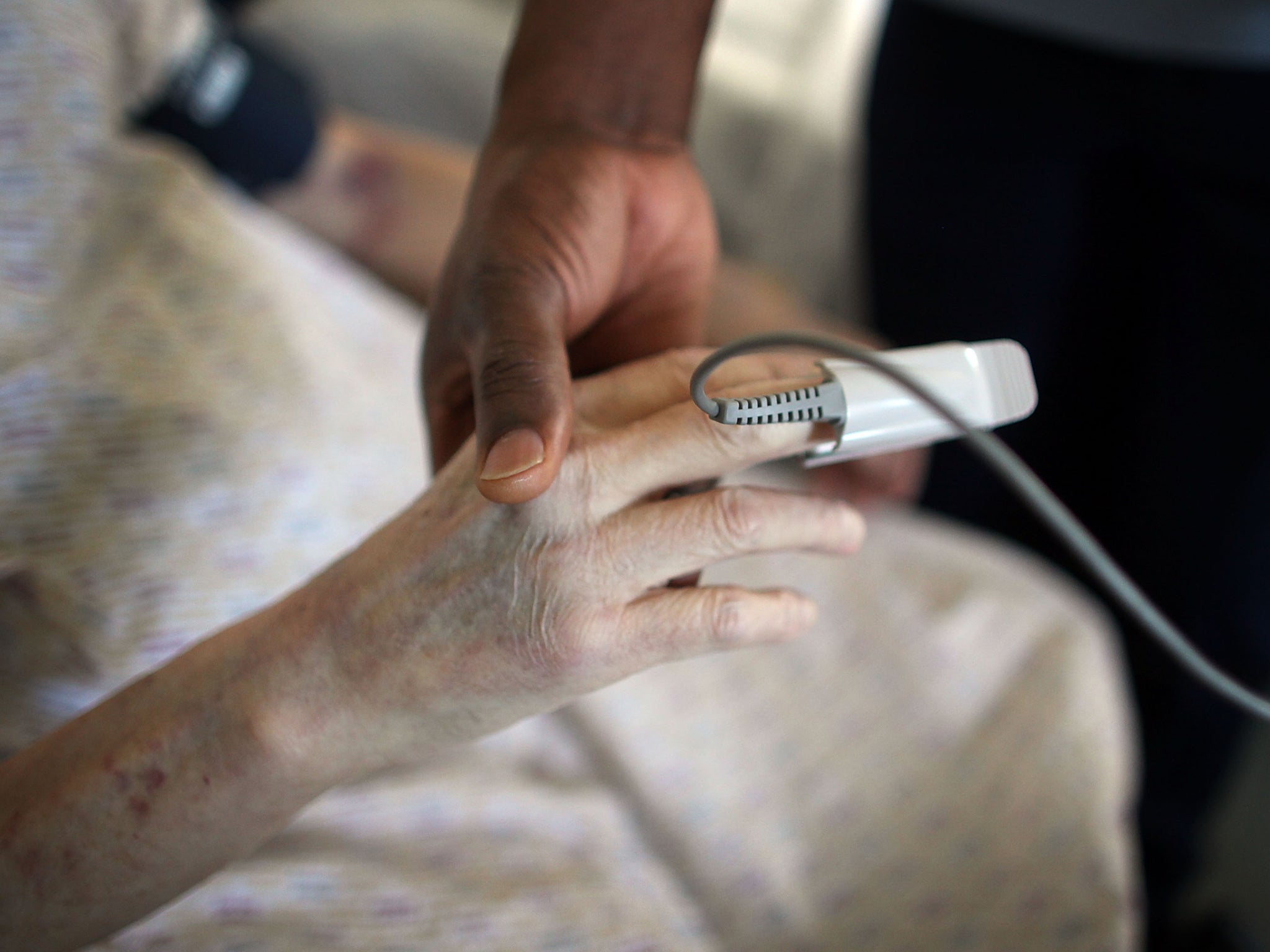
The NHS in England has announced that it will go ahead with the selling of patients’ data, despite fierce – and to my mind, ill-informed – public opposition on grounds of privacy.
The NHS holds a huge amount of information that makes it a treasure trove both for scientists and commercial companies. Given the amount of personal data that is currently sold – which includes, scandalously, local councils’ electoral registers – it seems reasonable to let the NHS make some money, too, so long as the records are rendered strictly anonymous.
Any income will hardly close the looming hole in the NHS budget, which The Independent has highlighted this week. But the lack of commercial acumen has left the NHS worse off than it could be. Let me set, though, one condition to the sale of medical data. Such a change presupposes that those with access to confidential information treat it responsibly. This, alas, cannot be assumed. I am not thinking here primarily of the few who sell sensitive data that comes their way – which is a crime – but of the many who simply don’t treat other people’s information with the care it requires.
The experience of my late mother shows some of what is wrong. Last year, a few months before her 91st birthday, my mother’s already indifferent health took a sharp turn for the worse. She had been operated on, successfully, for a melanoma on her foot many years before, and the sudden deterioration led us to suspect that the cancer might be back.
So my brother and sister-in-law, who were looking after her, requested a scan in good time for her next routine oncology appointment, which was duly done. At the outpatients’ clinic two weeks later, she was seen by a junior doctor, who looked at her notes, asked some standard questions, said she was doing fine, and asked her to come back in six months’ time.
This seemed consoling. But the deterioration in my mother’s condition continued. And the more my brother and sister-in-law thought about it, the more they wondered what the scan had shown and whether, indeed, the doctor had even seen it.
They managed to contact the specialist nurse whom my mother had seen at some previous appointments. The nurse eventually tracked down the scan, and saw at once what it showed: the cancer had quite suddenly and rapidly spread. For weeks, everyone concerned with my mother’s care – the GP, the district nurse, the hospital – had insisted that her deterioration was just temporary. The scan showed, on the contrary, that her various complaints were not isolated, and were not going to go away.
If the scan had been read when it should have been, both my mother and those caring for her would have received the sort of specialist help that the GP, the district nurse and others had insisted was not yet needed. The rest of the family would also have known the score.
It was only because my brother and sister-in-law – both lawyers – knew who to contact at the hospital informally, that they found out what the scan had shown. All the effort that had been applied to making the most of my mother’s routine six-monthly appointment at the skin cancer clinic – at, it should be said, one of the country’s best-regarded teaching hospitals – had been a complete waste of everyone’s time (and NHS money).
After trying, and failing, to get some sense out of the hospital as to whether and how the scan had gone missing – a verbal explanation would have been fine – my brother submitted a complaint. As a lawyer he knew how to do this – and the sort of language that would have the best chance of eliciting an answer.
The hospital’s first response was an estimate of how long it would take to answer the various questions raised. As the estimated deadline for the reply passed, the hospital said it still had points to clarify. A month later, after more prodding and a couple of emailed apologies for “any distress or anxiety the delay has caused” – the delay, note, not the mislaid scan – the official response arrived.
Amid all the defensive jargon – which included this gem: “It is usual that consultants, registrars and senior house officers see patients in Mr X’s clinic… Within the NHS we often work as teams, which mean [sic] that we can see more patients and also provide training” – it emerged that the scan results had not been included in her notes in time for her appointment at the clinic, or at all.
In his complaint, my brother had also asked whether there was any “guidance or standard procedures” governing the disclosure of scan results to patients and their GPs. “Unfortunately”, the reply went, “there is not a document … that contains specific guidance and procedure… The process has been developed over many years in relation to technology changes and service improvements.”
So that would be a “No”. And note that use of “improvements”.
The letter closes with the hope that “you feel we have taken your concerns seriously and addressed all the issues raised”. Well, we sort of did. A lot of time (three months) had been spent and a lot of soothing words deployed. But we sort of didn’t, either. So my brother tried again. He received a reply in late November. This time the language was less bureaucratic and more direct.
Within what sort of time could patients expect to receive the results of a scan? It transpired that while there are NHS targets for new cancer referrals, “there is no specific target for follow-up scans or imaging”. Nonetheless, the letter said, the radiology department had been asked to do the scan before the end of May and the results to be available for my mother’s appointment in June.
It said: “Both of these requests were achieved, as the results were available at the time of her outpatient appointment. However, they had not been entered into the notes, which resulted in the surgeon being unable to review the scan.” Aha, so we were getting somewhere – and then we weren’t: “We can only apologise for this error, unfortunately, we have been unable to ascertain at exactly what point during the preparation of your mother’s notes this was missed.”
As for procedures: “Currently the system in place is that the notes are returned to the medical secretary for the consultant, and they then wait on a specific shelf marked histology. This means, when the histology comes in, it is entered into the patient’s notes and returned centrally for storage.” Or not, as the case may be.
My brother had also asked what provision there was for speeding up the reporting process when unexpected findings are seen on a scan. “In your mother’s case,” it said, “the results were not unexpected.” In other words, what might seem out of the ordinary to you or me was regarded by the professionals as just more of the same, even though crucial care decisions hung on the change.
My mother died in February. The knowledge of how grave her condition was meant we could arrange for the help that was needed and she was able, thanks to the heroic efforts of my brother and sister-in-law, to end her long life at home. She was aware that her cancer had spread. She would not have been aware of the complaint submitted by her son. She was of a generation that ran a mile from making a fuss and was, for the most part, extravagantly grateful for the NHS.
Of course, the significance of a scan mistakenly left on a shelf should not be exaggerated. This was not, by any manner of means, gross medical negligence. My mother was 91 and terminally ill. But her last months were made more difficult by one link that inexplicably failed in a crucial chain of care. This is why, while I accept the concerns about data selling and privacy, I tend to think that it is less the commercial aspect that is the problem, than the careless, even cavalier, attitude towards other people’s information shown by professionals who should know better.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments