The Independent's journalism is supported by our readers. When you purchase through links on our site, we may earn commission.
Scientists develop new wearable device that injects opioid-blocking drug to reverse overdose
Device detects life-threatening breathing pattern that occurs when people experience opioid toxicity
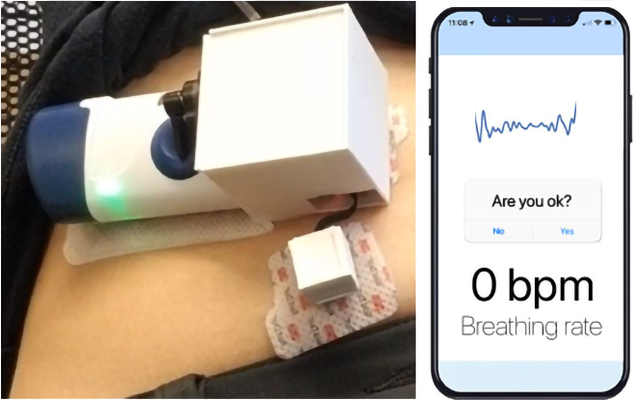
Scientists have developed a prototype wearable device that monitors breathing patterns and administers the potentially lifesaving antidote naloxone to reverse an opioid overdose.
The auto-injecting device, similar to an insulin pump, may potentially reduce fatalities due to opioid overdoses which remain a major public health crisis in the US, particularly heightened during the Covid-19 pandemic, say the scientists from the University of Washington in the US.
The prototype, described in the journal Scientific Reports on Monday, uses sensors and a wearable injector that safely administers medications, along with a specially developed algorithm to detect life-threatening breathing patterns that occur when people experience opioid toxicity.
It includes a pair of accelerometers that measure respiration, as well as an onboard processor that detects the halt of motion associated with breathing, the study noted.
The scientists say naloxone is highly effective and can potentially save lives if administered in a timely fashion.
The wearable system activates the injector in the presence of prolonged abnormal breathing pauses called apneic events, and can also transmit data about breathing rates to a nearby smartphone via Bluetooth, the researchers said.
“A closed-loop naloxone injector system has the potential to complement existing evidence-based harm reduction strategies and, in the absence of bystanders, help make opioid toxicity events functionally witnessed and in turn more likely to be successfully resuscitated,” the scientists wrote in the study.
“We have created algorithms that run on a wearable injector to detect when the wearer stops breathing and automatically inject naloxone,” Justin Chan, study lead author and PhD student at UW said in a statement.
To test the device, the scientists conducted a clinical trial involving 25 volunteers in a supervised injection facility in Vancouver, Canada, and another parallel trial in a hospital environment among volunteers who manifested signs of apnea by holding their breath.
The researchers said these trials were crucial to develop breathing algorithms involving real-world, opioid-induced breathing changes.
At the Vancouver site, the scientists noted that the device could accurately track respiration rates among people with opioid-use disorder and was also able to detect non-medical, opioid-induced apnea – a breathing pattern that commonly precedes a potentially fatal overdose.
This testing measured breathing patterns only to develop the respiratory algorithm and did not involve the injection of naloxone, which the researchers noted was administered only in the second study involving healthy human volunteers who did not take opioids.
In this second study, they said 20 participants simulated overdose events in a hospital setting by breathing normally, then performing a breath-hold for 15 seconds to mimic an apneic event.
When the device detected that the subject had not moved for at least 15 seconds, it activated and injected naloxone into the participant, the study noted.
Based on these results, the scientists believe the system could deliver the antidote into the blood, showing its potential to reverse opioid overdoses.
The UW scientists say further research is needed to assess the comfort and discreteness of the device over longer time periods, particularly in unsupervised settings, adding that more studies of the device are needed to evaluate naloxone injection in people who use opioids for non-medical purposes.
Early data from the US Centres for Disease Control noted that over 100,000 people died in the US due to drug overdoses in the year ending April 2021.
In a recent survey of about 100 opioid users in Philadelphia that was published in the Harm Reduction Journal, about three quarters of the respondents reported a willingness to use a device capable of detecting an overdose and automatically administering a reversal agent.
“We are hopeful it can have a tangible impact on a big source of suffering in this country,” said Shyam Gollakota, a UW professor of computer science and engineering, adding that the device could potentially help people at different stages of opioid-use disorder to avoid accidental death.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks