The Independent's journalism is supported by our readers. When you purchase through links on our site, we may earn commission.
Adult acne: Causes, myths and treatments
Diets high in sugar have been known to cause acne, as well as certain medications. Studies have investigated the commonly held belief that it is linked to poor hygiene, but shown frequent skin washing aggravates acne.
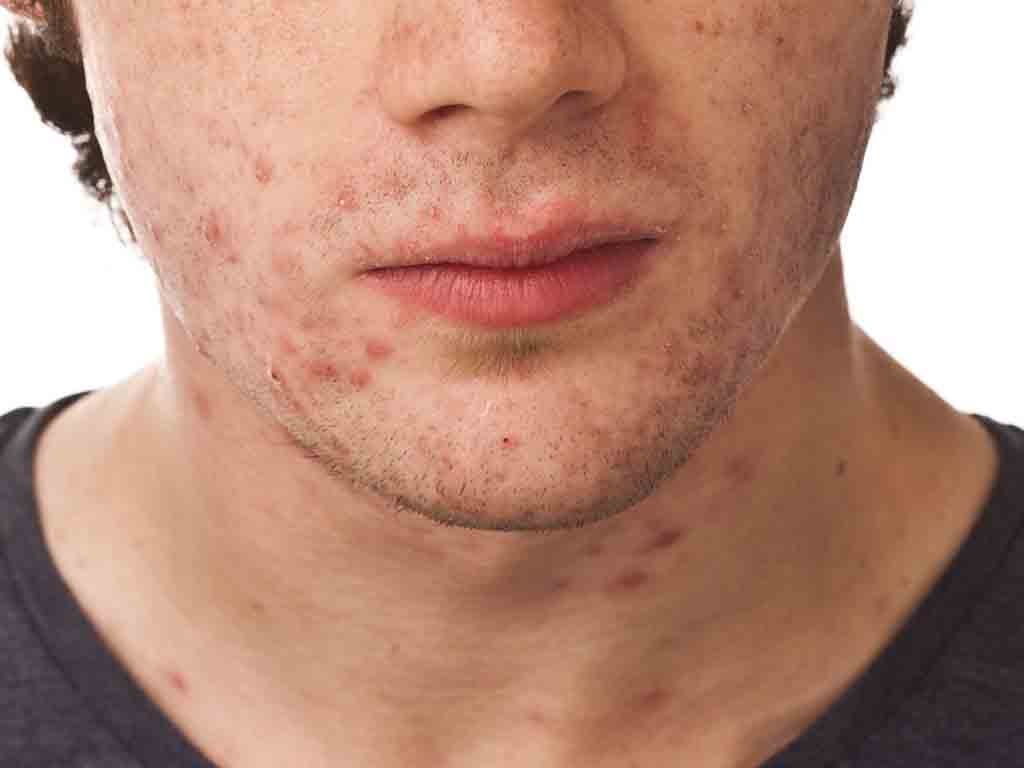
Acne is a condition banished to the back of most people’s minds - a grim memory of their teenage years. In reality, it is a condition experienced by many British adults.
Spot breakouts can happen at any time of life. In adolescence the main culprit is the effect of testosterone on the skin, but as we move into adulthood the list of possible causes increases.
Our skin contains millions of hair follicles and acne occurs when these get blocked. Sebaceous glands within the follicles release a substance called sebum which is responsible for providing moisture, lubrication and a waterproof barrier for the skin. If you have acne there is an overproduction of this sebum which mixes with skin cells and plugs the follicles. This provides perfect conditions for bacteria to flourish, with the resulting inflammation leading to spots.
The triggers
Some patients who have acne as an adult will already have experienced it in their younger years. For others it can present itself for the first time during adulthood. NHS figures suggest it affects 5% of women and 1% of men over 25.
Acne has a strong hereditary basis, with one of the largest twin-based studies demonstrating that up to 80% of acne cases have a genetic component.
Unfortunately for women, many of the triggers of adult acne are hormone related. Fluctuations during the menstrual cycle, pregnancy and around the menopause have all been linked to acne. Women who suffer with polycystic ovarian syndrome (PCOS) are also more prone to acne, as they have higher levels of testosterone, which increases sebum production and is responsible for thicker, coarser hair growth, making the follicles more likely to become blocked.
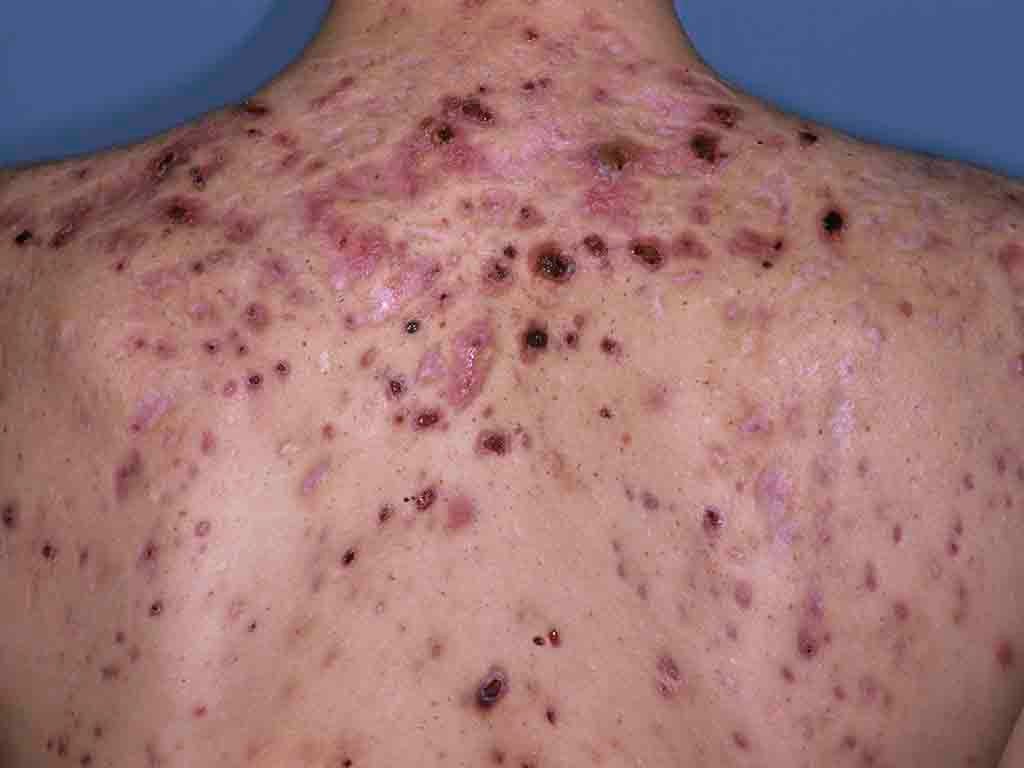
Some commonly used medications have been shown to increase the likelihood of acne too, including corticosteroids, anti-epileptics and some mood-stabilising treatments such as Lithium. Over the last decade there has been increased use of performance-enhancing drugs such as anabolic steroids, which raise the risk of acne.
The myths
There are many common myths regarding acne. Studies have investigated the commonly held belief that it is linked to poor hygiene. However, it has been shown that frequent skin washing aggravates acne with current guidelines recommending skin is washed no more than twice per day.
The debate over acne and diet continues and some patients report an improvement after modifying their diet. The Journal of American Academy of Dermatology published a review in 2014 of the evidence regarding acne and diet. One of the findings suggested that patients who consumed high sugar diets had higher instances of acne. If a patient has found that altering their diet has improved their skin, and if the changes are not detrimental to their general health, it is worth continuing with.
Acne is a cause of stress for many adult sufferers, although there has been no established link between developing acne and your stress levels. Neither is there a clear link between the use of cosmetics. However, wearing make-up that has a higher oil content can, in theory, increase the risk of blocking the hair follicles.
Treatments
There are many treatments to combat acne and they include both over-the-counter and prescription-strength preparations. Patients are encouraged to start with topical treatments in the form of gels, creams or skin washes. First-line treatments for mild acne are topical retinoids or benzoyl peroxide, or an azelaic acid treatment if these haven’t helped. Some women with mild symptoms might find the contraceptive pill - if permitted by their medical history - improves their skin.
If these treatments fail to improve symptoms, topical or oral antibiotics might be considered. Unfortunately, a small percentage of patients will not respond to these treatments, in which case your GP can refer you to a dermatologist for specialist treatment.
The most important aspect of treatment to understand is that they do not work overnight and need to be continued for at least six to eight weeks before improvements can be seen. Some antibiotics may take several months for visible effects.
As medicine moves forward, the treatment options and combinations are ever improving. With all the options available, your GP can help you to banish the breakout.
Dr Alexandra Phelan is an NHS GP and member of the Pharmacy2u.co.uk Online Doctor Service team.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks