What is gout? Symptoms and tips to avoid ‘embarrassing’ disease that afflicted Josie Gibson
Gout diagnoses have doubled since 1990. It affects 1 in 40 adults in the UK, mainly men aged between 30 and 60
This Morning host Josie Gibson has revealed that she has been diagnosed with “gout” after filming a new travel show for Channel 5 called Around the World in First Class.
The 40-year-old was told about the diagnosis when she underwent a health check for another show called The 1970s Diet. Gibson admitted to overindulging while filming the Channel 5 travel show and said the health revelation forced her to change both her eating and sleeping habits.
Joking about the condition, Gibson added: “I thought only kings like Henry VIII got gout. I was like, I'm a 40-year-old woman, this is really embarrassing. I think when some presenters taste something, they just have a little nibble. But I love my food too much, I just can't help it.”
“As soon as I stopped catching all the flights and started drinking a bit more water and less champagne, it levelled itself out,” added the TV personality. Other notable individuals who have confessed to having the disease include James Corden and Jared Leto.
What is gout and what are its symptoms?
Gout is a disease caused by inflammation within a joint. A chemical in the blood called uric acid works to break down a substance called purine. If there is too much uric acid in the body, it crystallises to form deposits in the joints, tendons and tissues. These deposits cause the inflammation that we refer to as gout.

Gout diagnoses have reportedly doubled since 1990. It affects 1 in 40 adults in the UK, mainly men aged between 30 and 60. The big toe is the joint most commonly affected. Symptoms typically include a red, hot, swollen joint that is excruciatingly painful, often with a rapid onset. It can be difficult to determine if a patient is suffering from gout or an infection in the joint, as both appear quite similar. For that reason, patients should see their GP if symptoms develop.
Gout can also present as a more chronic problem. Uric acid can form clumps called tophi, often in the tips of the ears, knuckles or within tendons and joints. When in a joint, they can cause damage to the bone and lead to chronic arthritis problems.
How does someone get gout?
There are many reasons why a patient might suffer from gout. Genetics play a significant role. Medication can also be a factor, with diuretic treatments that help eliminate excess fluid from the body being linked. If the body is not able to eliminate uric acid effectively, for example, if the kidneys are not working efficiently, the risk of developing gout is higher. Other risk factors include a higher body mass index (BMI), stress, dehydration and joint trauma.
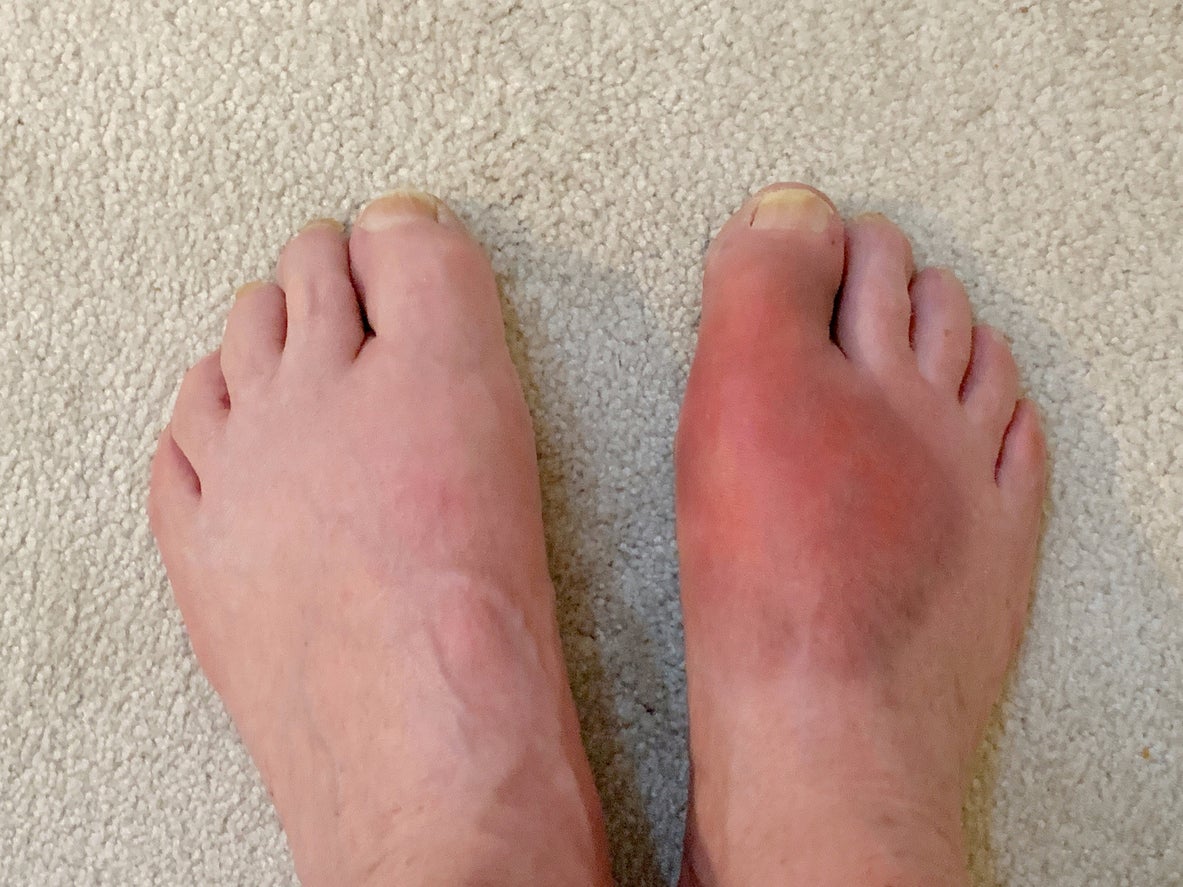
Diet plays a key role in increasing the chances of developing gout. Patients who drink alcohol above the recommended guidelines, particularly beer, should reduce their intake. Other links have been established with the consumption of high fructose-sweetened drinks, meats including liver and kidney, and seafood such as shellfish and sardines. These foods are generally high in purine. Patients with a history of gout should opt for low-purine diets.
How to treat gout
There are a number of treatment strategies for gout. They depend on whether patients are suffering from acute attacks of gout or chronic gout, or want to prevent further attacks of gout.
Vitamin C can be effective in reducing the frequency of acute gout attacks, as can regular consumption of low-fat dairy products such as skimmed milk. There is also evidence to suggest that coffee has a place in reducing gout attacks, although this comes with caution regarding monitoring caffeine intake. Lifestyle changes bring the most benefit: Things to consider include reducing how much alcohol you drink, ensuring a healthy BMI (although crash diets can worsen gout so should be avoided), ensuring adequate hydration, avoiding fructose-sweetened drinks and reducing overall purine intake.
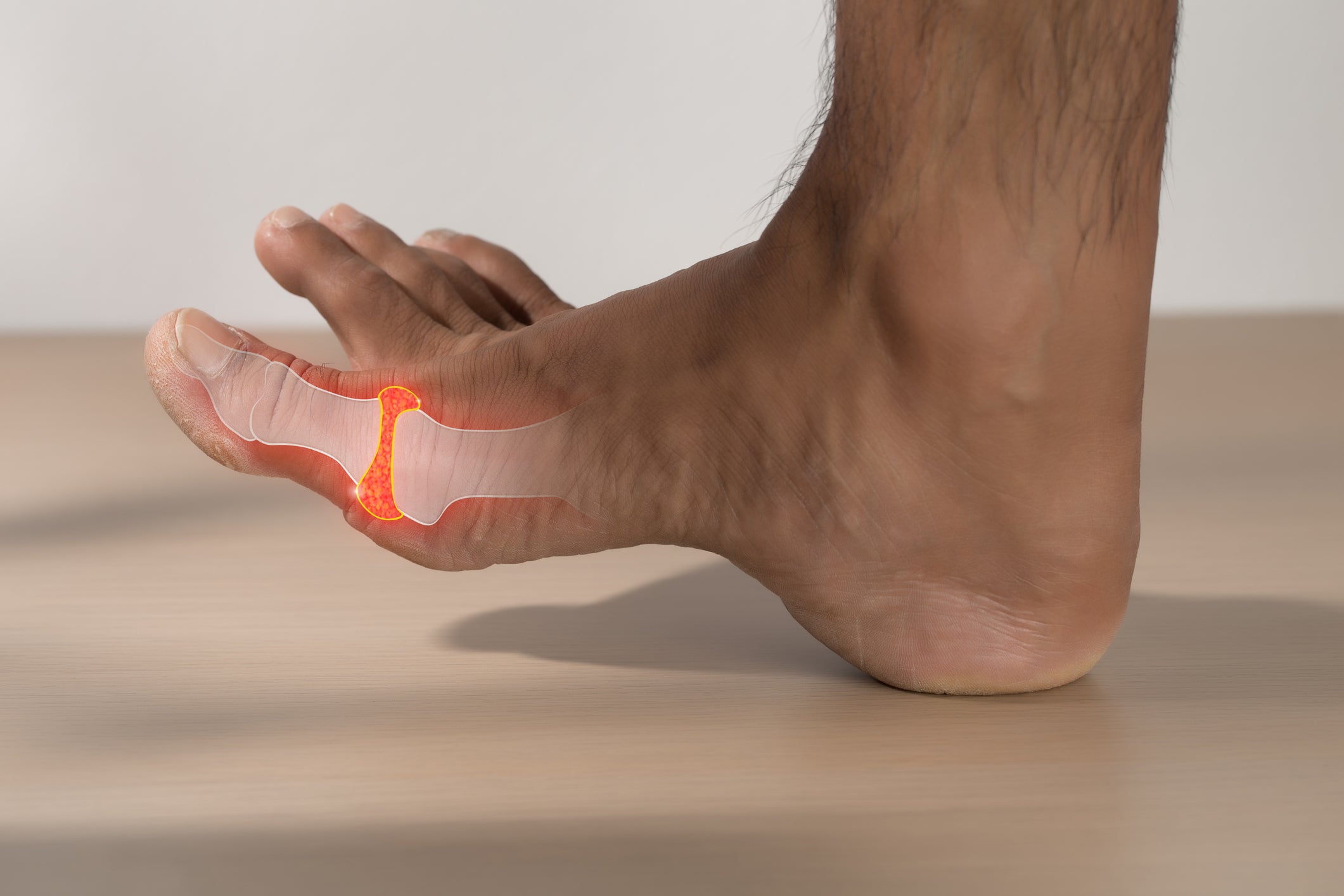
Your GP can offer several treatments for gout. Patients are initially offered a non-steroidal anti-inflammatory medication if permitted by their medical history. If this is not suitable or helpful, a specific treatment called colchicine is available, or a course of steroid medication may be offered. This should be used alongside pain relief medication. Other simple measures, such as ice treatment for the affected joint, with elevation, and resting the joint, are encouraged. If you have had more than two attacks in a year, your GP may discuss a preventative treatment called allopurinol or febuxostat.
Without treatment, most acute attacks will last up to seven days. Unfortunately, 60 per cent of patients experience further attacks within the next year.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks