What is vaccine-derived polio? The last stumbling block in the worldwide fight to eradicate the disease
Since 2000, nearly three billion children around the world have been given more than 10 billion doses of oral polio vaccine
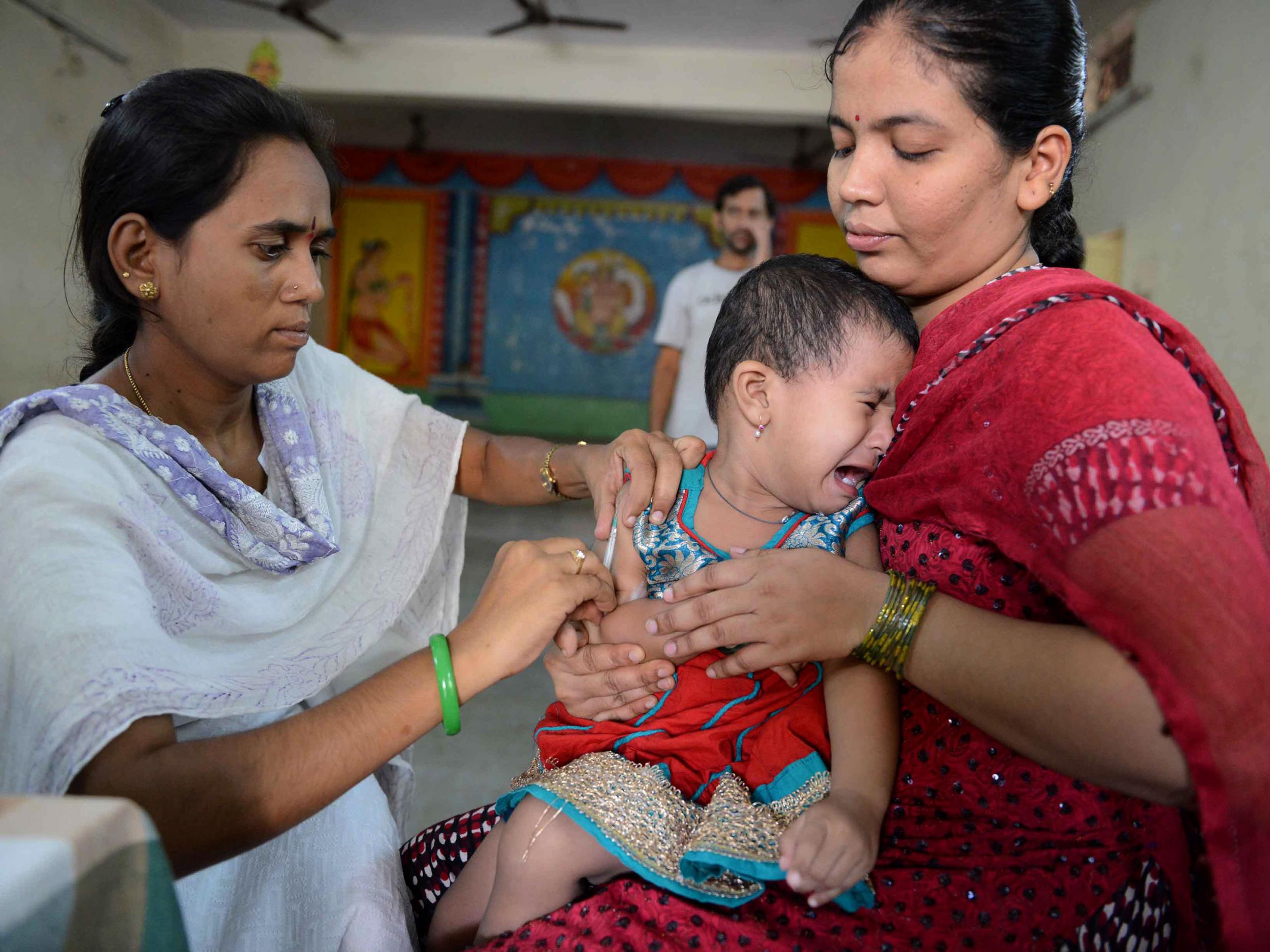
The world is on the verge of eradicating polio, a disease that for millennia has caused paralysis and death, mostly in children.
Polio is now only found in three countries – Pakistan, Afghanistan and Nigeria, and just 37 cases of the disease were recorded last year.
But challenges still remain, including cultural resistance to the vaccinations in some areas, where there have been violent attacks on health workers by Islamists.
In April 2016, the type of vaccine used to fight the disease was changed, to protect against the worrying phenomenon of vaccine-derived polio.
Here is everything you need to know about the switch.
How many different types of polio virus are there?
There are three different types of naturally circulating, or “wild”, polio virus. Even if you become immune to one strain of the virus, you can still be infected with the others.
The success of vaccination campaigns means only one of these strains, type 1, is currently at large.
Type 2 polio virus was last detected in India in 1999 and was declared eradicated in 2015, while type 3 has not been seen anywhere in the world since November 2012.
What is the difference between the injectable polio vaccine (IPV) and the oral polio vaccine (OPV)?
The injectable vaccine, developed in the early 1950s by Jonas Salk, is made from a killed, or chemically inactivated, polio virus. It contains all three strains of the virus and is injected into the skin or muscle by a trained health worker.
Antibodies are then created in the blood that fight the infection and protect against paralysis.
While the vaccine is highly effective in preventing the disease, it does not induce immunity in the intestines. This means that the virus can still multiply in the gut and continue to circulate within a community.
The oral polio vaccine, created by Albert Sabin in 1961, contains a weakened form of the live virus. It is the most widely-used vaccine in the fight against polio worldwide, because it is inexpensive and easy to deliver by volunteers with no medical training.
What is vaccine-derived polio?
The weakened vaccine-virus in OPV can multiply in the gut, spreading immunity between people. This is usually an advantage, because it strengthens a community’s collective defences against the disease and curbs its transmission.
However on rare occasions, when levels of routine immunisation are poor, it can continue to circulate for a long time. If this is allowed to occur, the vaccine-virus sometimes mutates into a form that can cause paralysis.
These cases are unusual; last year, there were just five cases of vaccine-derived polio in the world. But to prevent any further cases, IPV is being deployed as well as OPV.
Since 2000, nearly three billion children globally have been given more than 10 billion doses of OPV, according to the World Health Organisation. This has prevented more than 13 million cases of polio.
In that time, 24 outbreaks of vaccine-derived polio were detected in 21 countries, with fewer than 760 cases reported overall.
How is vaccine-derived polio being tackled?
Different types of OPV contain different strains of weakened polio virus. The trivalent vaccine, which was the main type used until last year, contains all three strains of the virus.
Since April 2016, routine immunisation internationally has used the bivalent OPV, which contains just weakened versions of type 1 and 3 of the virus.
This is to minimise the risk of vaccine-derived polio developing from the type 2 virus.
IPV, which protects against all types of polio, is also being administered in greater frequency to prevent the type 2 virus from making a comeback after it was dropped from the OPV.
Is there a shortage of IPV?
Yes. The two manufacturers of IPV have said they are only able to supply half of the 110 million doses of injectable polio vaccine that global health bodies have said they require this year.
“We are projecting now that we won’t have the quantities we need until 2018,” said Shanelle Hall, director of Unicef’s supply division.
The three countries where wild polio virus is still endemic, Pakistan, Afghanistan and Nigeria, are at the top of the list to receive the most IPV.
And to stretch the supply, governments and health organisations have been told to give children “fractional doses” of IPV, by injecting a rationed amount into the skin instead of the muscle.
What about if polio is finally eradicated?
Rotary International and WHO have said 2017 could be the year in which the world’s last case of polio is recorded.
Jay Wenger, head of the polio programme at the Gates Foundation, said that if worldwide polio eradication was confirmed in 2020, the use of OPV would be discontinued.
“We would treat vaccine-derived polio in small, localised campaigns,” he told The Independent. “It’s obviously a complication, but we see it as a doable activity. The endgame will be just to use IPV then, as insurance for several more years.”
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments