Baldness ‘breakthrough’ as scientists claim to have found key to growing new hair from stem cells
‘Scaffold’ for embedding stem cells leads to cell growing in more regular pattern and brings clinical use a step closer
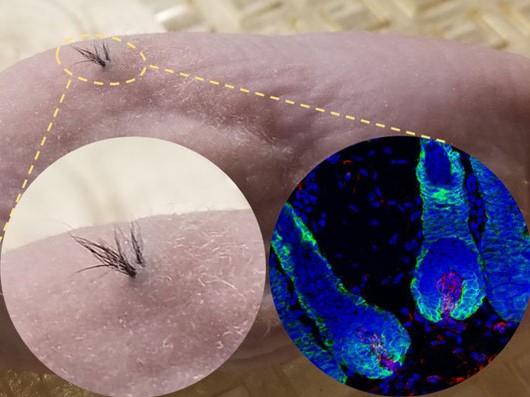
A cure for baldness may be only a hair’s breadth from success as researchers claim to have overcome one of the major hurdles to cultivating human follicles from stem cells.
Researchers have previously grown hair from the cells, which can transform themselves into any part of the human body, but until now had little control over the process.
However, a US team says it has developed a system that guides the cells to implant and develop in a way that replicates natural hair production.
They used a biodegradable “scaffold”, made of the same materials as the dissolvable stitches used to close wounds, to help the human cells integrate with a mouse subject.
Presenting the findings at the conference of the International Society for Stem Cell Research (ISSCR) in Los Angeles, the researchers described the advance as a ”critical breakthrough” that could help millions.
“Our new protocol ... overcomes key technological challenges that kept our discovery from real-world use,” said Alexey Terskikh of Sanford Burnham Prebys Medical Discovery Institute in California.
“Now we have a robust, highly controlled method for generating natural-looking hair that grows through the skin using an unlimited source of human [stem cells].”
Male pattern baldness affects about 50 per cent of men over the age of 50, according to the British Association of Dermatologists, with many men suffering hair loss from puberty.
Current treatments include the drugs minoxidil or finasteride, which have side-effects and have to be taken for life.
Hair transplants, where follicle cells are extracted from other parts of the body and implanted in the head, can cost anywhere between £1,000 and £30,000.
Dr Terskikh and colleagues are now looking to try out their technique in human subjects.
The work was awarded a merit award by the ISSCR – but has not yet been published in a peer-reviewed journal and hurdles remain in scaling it up.
In the study, the mice subjects were immunosuppressed to stop their immune system attacking the foreign stem cells.
This could be overcome in humans by using stem cells from the intended recipient.
The cells used in Dr Terskikh’s experiments were obtained from a blood sample and then reprogrammed to revert into stem cells – a process known as induced pluripotency.
While there is a potentially “unlimited” supply of these cells in the blood, this reprogramming process is still relatively costly with current techniques.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks