Coronavirus: Watchdog relaxed rules on doctors operating in private hospitals weeks after inquiry’s safety warning
‘I am appalled more patients could be going into the private sector when not a single recommendation from the Paterson inquiry has been implemented,’ victim of rogue surgeon tells The Independent
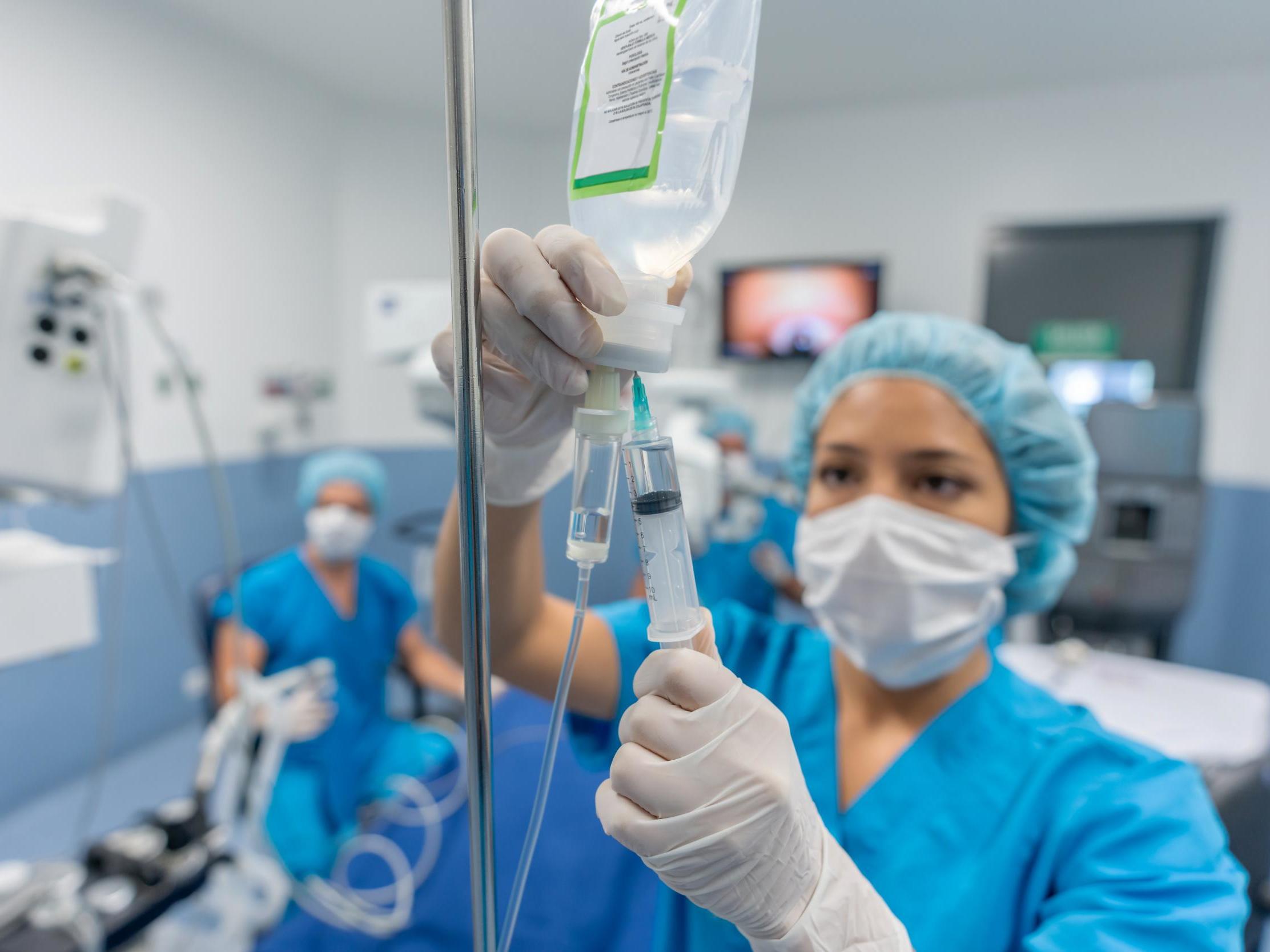
Controversial rules allowing doctors to operate on patients in private hospitals have been fast tracked during the coronavirus crisis, just weeks after an independent inquiry warned they were a risk to patient safety.
The Independent has learned the Care Quality Commission (CQC) wrote to private hospitals in March and agreed to a streamlined process for consultants to gain what is known as “practising privileges” to allow them to start work immediately in private hospitals.
These privileges allow a doctor to operate on patients, but they are not considered employees of the hospital and their work is monitored less closely. It was under this system that rogue breast surgeon Ian Paterson was able to operate unnecessarily on more than 1,000 women.
In February, a government inquiry into how Paterson was able to operate with impunity for more than 17 years warned the system was open to abuse, and said ministers needed to address “as a matter of urgency this gap in responsibility and liability”.
The Rt Rev Graham James, who chaired the inquiry, told The Independent that keeping the rules in place meant “people would be less safe in the private sector than they are in the NHS. I cannot think the government wants people to be less safe”.
In March as the country faced an expected coronavirus surge in critically ill patients, the NHS signed an unprecedented three-month deal with private hospitals.
In a key change to the normal process the CQC said doctors were not expected to provide any evidence of their criminal record checks, CV, qualifications or health status beyond a signed declaration that this information was held by their NHS trust.
The hospitals were expected to confirm their identity and registration with the General Medical Council (GMC) before they started treating patients.
The CQC said the move was a pragmatic step taken with the expectation that large amounts of patients would be treated in private hospitals during the pandemic.
At the weekend The Independent revealed the NHS was now in talks with private hospitals to extend the contract and agree a new deal to tackle the growing backlog in delayed surgeries.
The increased use of the private sector has angered victims of Ian Paterson.
One of his victims, Deborah Douglas, from Hall Green, Birmingham, said she was left feeling “mutilated” by Paterson, who was jailed for 20 years in 2017.
She said: “I am worried and appalled that more patients could be going into the private sector when not a single recommendation from the Paterson inquiry has been implemented.”
David Rowland, from the Centre for Health and Public Interest think tank (CHPI), said the decision to fast track consultants into the private sector looked like a “kneejerk response” by the regulator. “A lot of private hospitals are standing empty. It wasn’t like there was a need to rush through all the people to have practising privileges. It wasn’t a problem for the sector,” he said.
He added: “This is further evidence that maintaining patient safety standards is not a top priority for the CQC. One of the reasons Paterson was able to get away with what he did for so long was because no one was monitoring his actions.
“Relaxing this already weakened requirement shows they have not learned the lessons from the Paterson inquiry.”
The CHPI has previously highlighted safety in the private hospital sector as a key concern, with many hospitals lacking the critical care facilities to deal with patients who deteriorate. Many rely on being able to transfer patients back to the NHS if they become too unwell.
“If we are increasing the number of patients in the private sector when NHS intensive care units will be under pressure for some time to come, where will the additional capacity come from?” Mr Rowland said.
Neither the CQC nor the Independent Health Providers Network (IHPN), which represents private hospitals, could confirm how many doctors had been granted practising privileges since March.
Professor Ted Baker, the CQC’s chief inspector of hospitals, said: “The interim approach for granting practising privileges agreed by CQC in consultation with the Department of Health and Social Care, the GMC and the IHPN ensures the formal legal process is streamlined, so not to act as a barrier to consultants who need to move between or start work in an independent hospital setting where they do not already hold practising privileges, while ensuring providers have appropriate governance processes in place and that patient safeguards remain robust.
“The process remains subject to review as we move beyond the first phase of the pandemic.”
David Hare, chief executive of the IHPN, said: “IHPN has worked closely with the CQC during this hugely challenging period to ensure that NHS consultants are swiftly and safely able to treat patients in independent sector hospitals where urgently required to do so due to Covid-19.
“The streamlining of the practising privileges process has helped to ensure flexibility during a serious pandemic whilst ensuring that the necessary clinical governance safeguards are in place to protect patients.”
The IHPN said safety standards were high in private hospitals with more than 80 per cent rated good or outstanding by the CQC.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks