PPE priorities for NHS must change as coughing greater risk than first thought for workers, study claims
Health service has prioritised stringent PPE - including respirators - for aerosol generating procedures
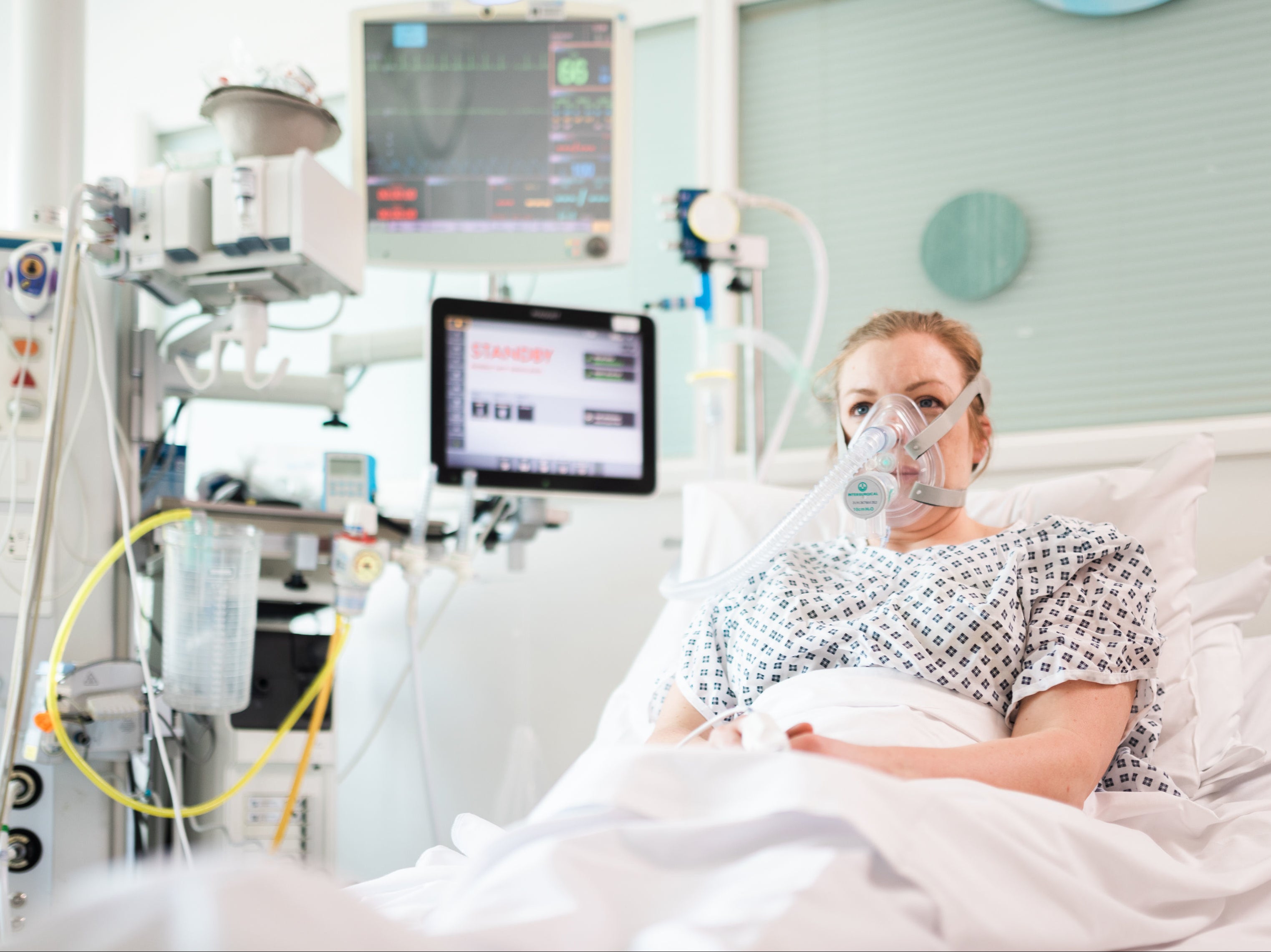
NHS workers surrounded by coughing patients are at a greater risk of contracting Covid than first thought, a study has suggested.
The research found that coughing generated at least 10 times more infectious “aerosol” particles than speaking or breathing.
Throughout the health service’s pandemic response intensive care units have been deemed a particular hazard area to healthcare workers due to concerns that some treatments, including continuous positive airway pressure, or CPAP, may increase the risk of the virus spreading.
Aerosols are believed to be a significant route of transmission for the virus, and may remain in the air for hours after leaving a person’s body - creating a risk to anyone in the same area without proper protection.
The level of risk has seen PPE prioritised for those dealing with aerosol generating procedures - with guidance telling workers to wear FFP3 respirator masks instead of the fluid repellent surgical mask provided in more typical care settings.
However a study, not yet peer reviewed, has suggested the risk may be far greater in general wards with covid patients, with coughing related to a significantly greater spread of aerosols into the air.
The study from the University of Bristol and the North Bristol Lung Centre said: “In healthy volunteers, CPAP… produced less aerosols than breathing, speaking and coughing.”
Meanwhile those who underwent high-flow nasal oxygen treatment, used for patients with acute respiratory failure, were also found to cause minimal risk - with aerosols produced too small to carry virus particles.
“HFNO did emit aerosols”, the study’s findings added, “but the majority of these particles were generated from the HFNO machine, not the patient.
“HFNO-generated particles were small, passing from the machine through the patient and to the detector without coalescence with respiratory aerosol, thereby unlikely to carry viral particles.”
Researchers tested the risk of such procedures by monitoring the aerosols produced when healthy test subjects underwent both treatments, as well as when they breathed unassisted, spoke and coughed.
They then separately measured the emissions of aerosols from Covid-19 patients in the same circumstances.
The study added: “Although direct comparisons are complex, cough(ing) appears to generate significant aerosols in a size range compatible with airborne transmission of SARS-CoV-2.
“As a consequence, the risk of SARSCoV-2 aerosolisation is likely to be high in all areas where patients with Covid-19 are coughing.
“Guidance on personal protective equipment policy should reflect these updated risks.”
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks