London hospitals could be overwhelmed by coronavirus patients within days, NHS data shows
Capital’s hospitals had just 46 spare ICU beds on Monday
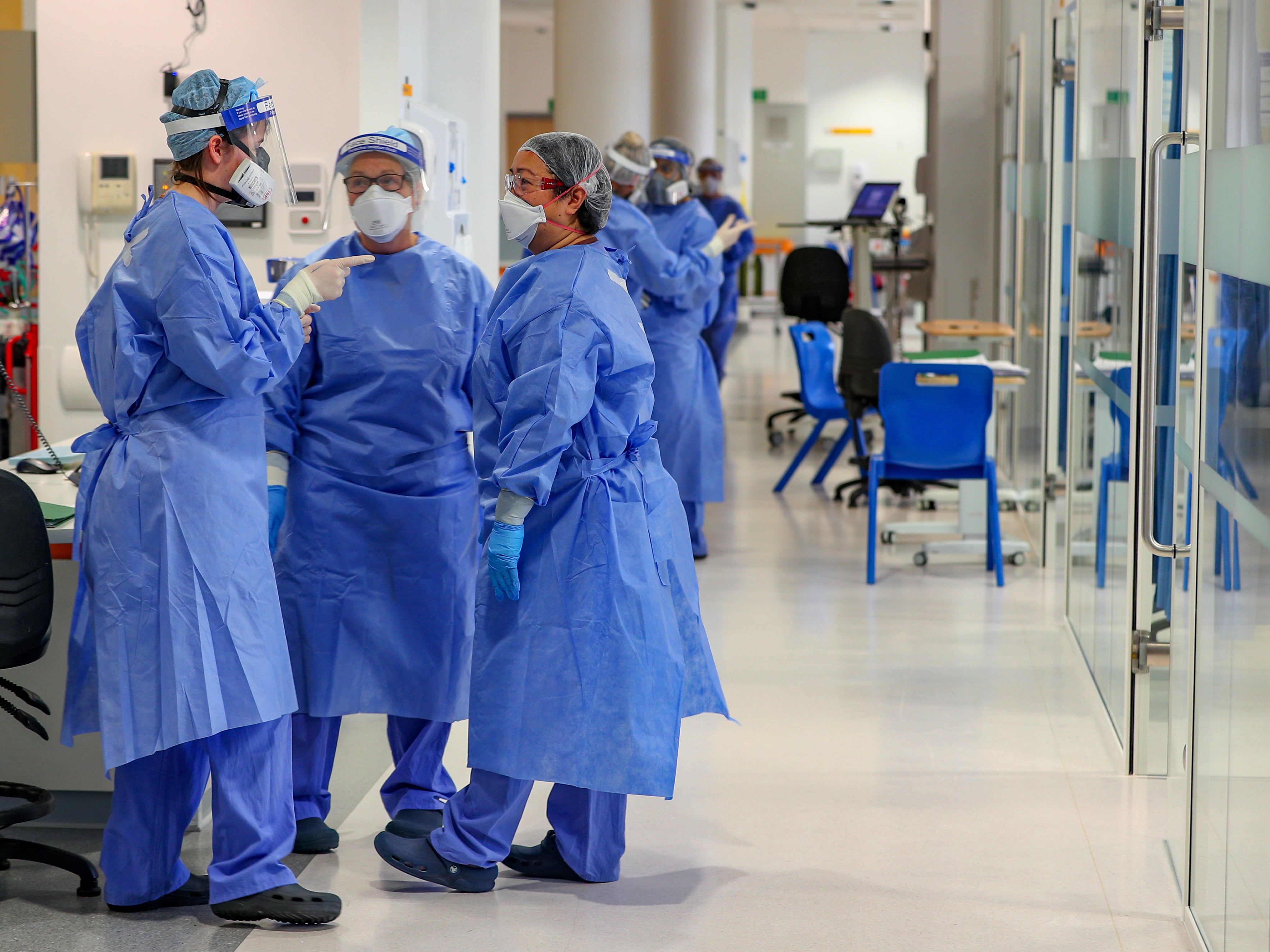
London hospitals could be short of nearly 2,000 hospital beds by 19 January, according to NHS forecasts of rising demand from coronavirus patients.
The stark position facing the capital was set out in a presentation by London’s regional medical director Vin Diwaker in a Zoom call on Wednesday.
Slides seen by the Health Service Journal show that even if the number of Covid patients grows at the lowest rate considered likely, and measures to manage demand and increase capacity, including opening the capital's Nightingale hospital, are successful, the NHS in London will be short of nearly 2,000 general and acute and intensive care beds within 12 days.
The briefing forecasts demand for both general and acute care beds as well as intensive care beds, for both Covid and non-Covid patients, against hospital capacity. It accounted for the impact of planned measures to increase capacity.
Hospitals across the city have been forced to create makeshift intensive care units in operating theatres, children’s wards and recovery rooms as the numbers of coronavirus patients keeps increasing.
NHS forecasts have outlined three scenarios, with the “best case” predicting a 4 per cent daily growth in patients and the worst case envisaging a 6 per cent daily increase in demand for critical care beds as well as general acute beds.
The briefing said that growth on 5January was 3.5 per cent for general beds and 4.8 per cent for intensive care beds.
A 5 per cent growth for two weeks would mean the NHS in London would need 2,300 ICU beds by 19 January. This would mean an increase of 640 ICU beds between 11 January and 19 January and 4,000 general and acute beds.
The briefing also included possible options to increase the numbers of beds required in the city.
This could include the NHS finding another 400 ‘surge’ beds opened up in new areas but there are widespread staffing shortages and sickness with staff to patient ratios already stretched to unsafe levels.
Private hospitals could be used to deliver another 50 beds along with 1,000 “step down beds” for beds ready to leave hospital which will include beds at the ExCel conference centre as part of the Nightingale field hospital.
All these efforts would give a total capacity of 15,600, still 1,500 short of forecast demand.
The shortfall in beds in the “average” scenario would be 2,900 and 4,400 in the “worst” case.
In the West Midlands, seven hospitals there have already declared a critical level 3 alert in their intensive care units with the HSJ report the region could be similarly overwhelmed within the next few weeks.
The central forecast for the Midlands is for Covid-19 positive patients in critical care beds to grow from 426 now to 681 by 21 January but the figure could be as high as 877. If the number of non-covid patients stayed the same, at about 180, then the region would be virtually out of beds even under the central forecast of 681 covid patients by 21 January.
Last week The Independent reported on warnings from NHS England’s London regional director that the city needed to find more beds. The latest data shows the city has come close to being full.
On 5 January London hospitals had just 46 spare ICU beds with just over 70 per cent of its ICU beds occupied by Covid patients.
In the southeast of England intensive care wards have already been overwhelmed with dozens of patients being transferred to hospitals hundreds of miles away.
On New Year’s Day hospitals in Kent reported bed occupancy levels in critical care at 137 per cent, meaning more beds are being used in non-critical care areas where staffing levels were also being stretched.
One clinician in the region told The Independent some patients who needed intensive care were being cared for on other wards because of a lack of space.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments


Bookmark popover
Removed from bookmarks