Growing success of UK vaccine rollout offers cause for new hope
The scale and speed of Britain’s rollout marks a rare win for the government
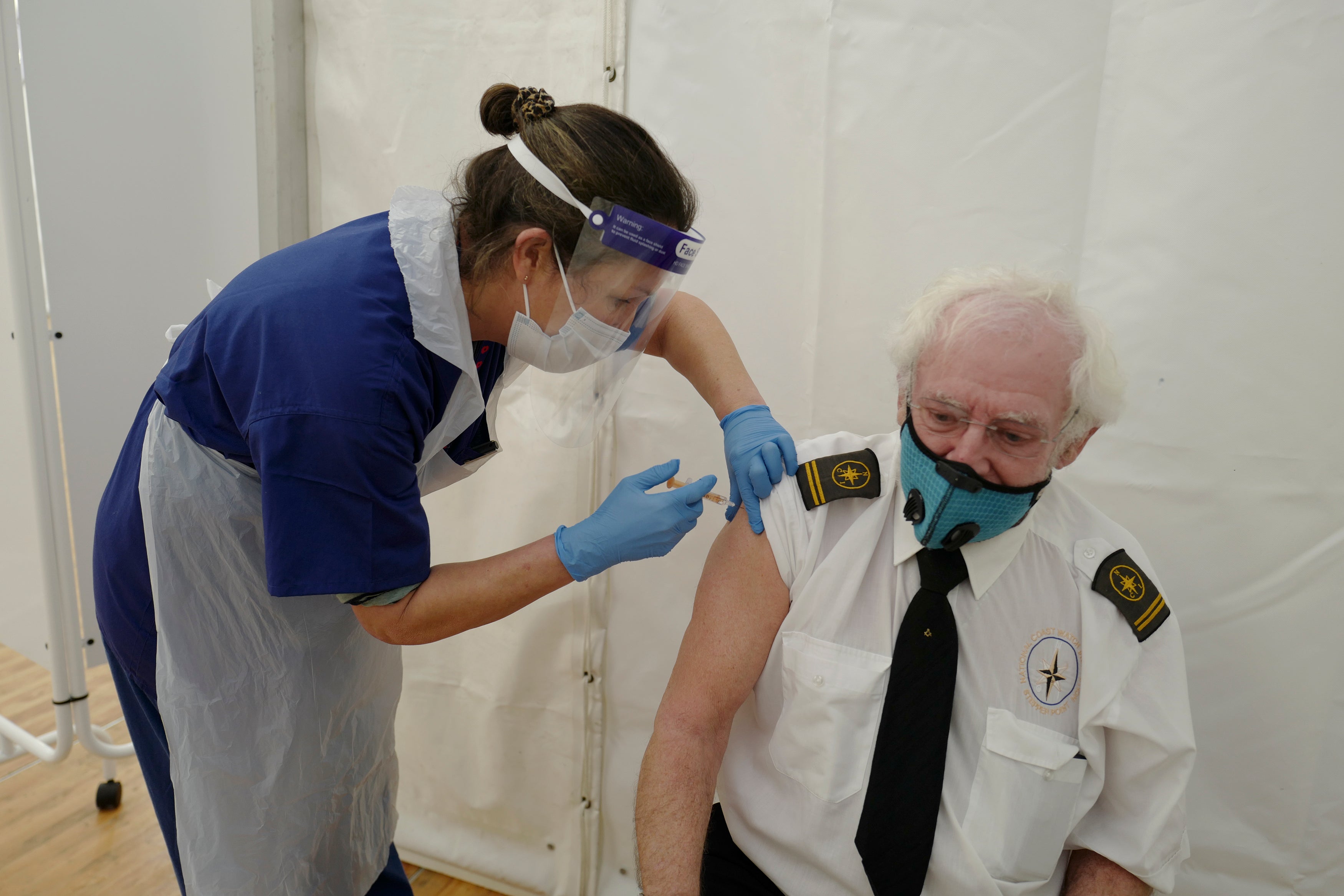
With more than 10 million first doses administered to date, the UK has moved rapidly and efficiently in delivering one of the largest vaccine programmes seen on the planet.
Amid this uncharacteristic success, the government has had no qualms in declaring that Britain currently has one of the world’s highest vaccination rates per capita – despite repeatedly warning against drawing comparisons with other countries throughout the pandemic.
It is a testament to the work of the UK’s Vaccine Taskforce in compiling a diverse portfolio of vaccines – with many deals secured long before the release of any trial data – as well as the collaborative and streamlined efforts of the NHS, which has led the way in getting jabs into people’s arms as quickly as possible.
After a catalogue of errors in responding to and handling the pandemic throughout much of 2020, there was initial reservations as to whether the government could deliver on its ambitious target of providing vaccines to 15 million vulnerable people by mid-February.
Even Sir John Bell, regius professor of medicine at Oxford University and a member of the Scientific Advisory Group for Emergencies, acknowledged that the success of the rollout depended on whether or not the government “screwed up” the distribution of the vaccines.
But following initial teething issues, supplies of the AstraZeneca and Pfizer jabs are now being delivered to the frontline on a regular basis, allowing GPs to administer 100s of doses a day within their local practices.
On the current trajectory, with just under 400,000 jabs being rolled out on a daily basis, the UK is on course to hit its mid-February target. Within the government itself, there is now quiet confidence that Britain is running ahead of schedule for its plans to offer a vaccine to all adults by August.
Spirits are meanwhile running high among GPs out in the field. “It’s been remarkable how well this has all gone,” one doctor told The Independent earlier this week. Many have said that the success of the rollout demonstrates what the NHS is capable of, arguing that test and trace could have been better run it had been handled by local health protection teams.
Of course, the vaccination programme has not been perfect. While some areas of the UK have raced ahead in offering a first dose to their entire over-80s population, others have lagged far behind.
It’s led to a patched picture of coverage throughout the four nations and plenty of consternation among regional politicians, who have vented their frustration at a perceived lack of supplies and accused the government of prioritising other regions in the UK.
Concern has also been raised over the “substantial divergence” in vaccination rates that have been recorded between different ethnic groups.
Of the 476,375 patients aged 80 and over who received a Covid-19 vaccine between 8 December and 13 January, the rate of vaccination was 42.5 per cent for white people. This figure stood at 20.5 per cent for black people – the lowest rate among England’s ethnic minority groups.
Labour MP Marsha de Cordova, the shadow women and equalities minister, said that the data provided yet more evidence that black, Asian and ethnic minority people were being hit hard by the virus, and accused the government of failing to protect these vulnerable communities.
“We must vaccinate Britain, and to do that we need a plan to ensure that no one from black, Asian and ethnic minority communities is left behind,” she told The Independent.
One of the most notable question marks hanging over the rollout is the decision to extend the delay between the administration of the first and seconds dose in a bid to stretch supplies and provide protection to as many people as possible.
Various scientists, experts and health groups have waded into the debate, arguing for and against the policy. In the case of the Pfizer/BioNTech vaccine, many claim that the UK has turned its back on the trial data and entered into uncharted scientific territory.
Indeed, research from Israel, which is leading the global vaccination race, suggests that that a single dose of the highly effective mRNA vaccine may provide less protection than originally hoped.
Others insist that unprecedented measures are justified in these unprecedented times. Compromise and adaption have been a common theme of this pandemic, with officials forced to break with scientific tradition when confronted by the existential threat of Covid-19.
The UK’s four chief medical officers have all publicly advocated for the current vaccine policy, while Independent Sage said there was “sound theoretical and empirical public health reasons” to support the decision to delay a second vaccine dose, including trial evidence which showed this prolonged interval boosts the effectiveness of the Oxford jab in preventing Covid disease.
The latest pre-print published by Oxford University certainly seems to have vindicated the government’s decision to extend the dosing interval. According to the study, the Oxford vaccine offers 76 per cent protection for up to 12 weeks after a first dose. This rises to 82.4 per cent once a booster shot is administered after three months.
Despite the lingering controversy, there’s no denying the scale and speed of the UK’s rollout to date. It marks a rare win for the government at a time when mismanagement, blunder and indecision seem to have been the order of the day.
With the UK following a similar path to Israel, where the recent fall in infections has been linked to the country’s vaccination programme, there’s growing hope Britain will be able to equally reap the rewards of its own impressive rollout and turn a corner in the not too distant future.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments


Bookmark popover
Removed from bookmarks