'Breakthrough' diabetes drug cut kidney and heart disease deaths by a third, trial shows
'With five million people worldwide predicted to have kidney failure by 2035 this is a major breakthrough'
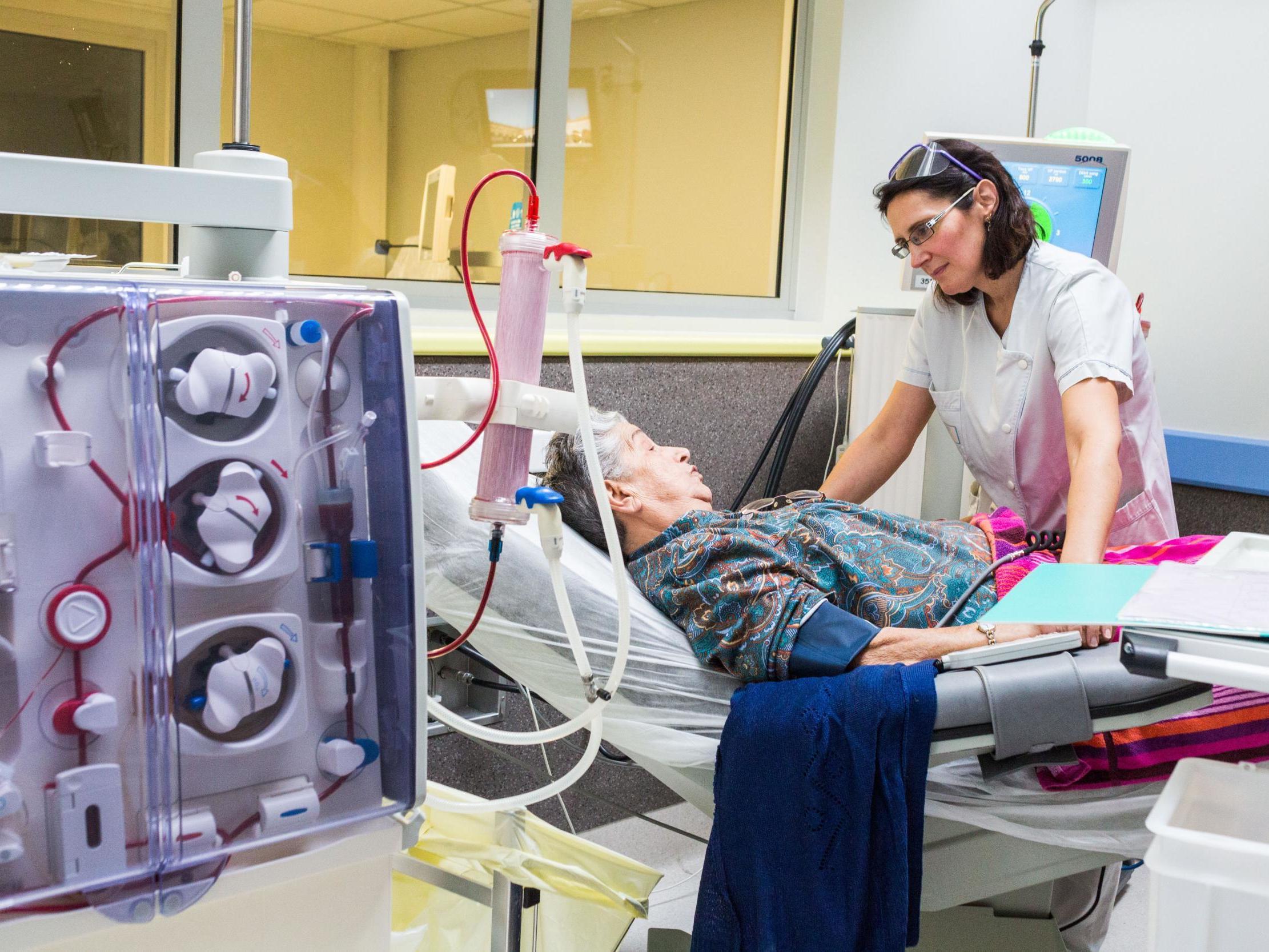
A breakthrough treatment could help protect hundreds of millions of people from the “21st century epidemic” of deadly diabetic kidney disease, a major trial has found.
Research from Australia and the UK has shown that a once-a-day blood sugar lowering drug, canagliflozin, reduced cases of kidney failure and death by a third in diabetic patients.
There are nearly five million UK diabetics and diabetic kidney disease costs the NHS as much as £927m a year according to researchers . However there have been no new treatments for nearly two decades.
“There are more than 400 million people with diabetes worldwide, around 40 per cent of these people will get kidney disease,” said the study’s lead author Professor Vlado Perkovic, executive director of the George Institute for Global Health.
“Once they’ve got kidney disease, they’re at very high risk of kidney failure, heart attack, stroke, and of death.”
Diabetic kidney disease is caused by years of poorly controlled blood sugar damaging the blood vessels in the kidneys, and undermining its ability to clean the blood of salts, protein and other waste products that can cause damage.
As well as increasing the risk of death from a range of cardiovascular conditions people who develop kidney failure may require regular dialysis sessions to clean their blood.
To test the effects of canagliflozin the authors recruited 4,401 patients with diabetes and kidney disease across 34 countries. It randomly assigned them to receive either canaglifozin, or a placebo, on top of their regular diabetes treatment.
The trial was stopped early because its high success rates meant leaving some participants on a placebo was unethical.
Its findings, published in the New England Journal of Medicine, show that over two and a half years kidney failure and deaths fell by 34 per cent compared to the placebo group.
Hospitalisations related to heart failure were also 39 per cent lower and heart attacks, strokes and deaths from heart diseases were 20 per cent lower. There were no major side effects.
“What we have shown is that this drug not only protects people with diabetes from developing kidney failure, but it also protects them from heart disease, heart failure and other cardiovascular complications,” said Dr Meg Jardine, co-author of the study.
“Importantly, it helps people who already have reduced kidney function and are at particularly high risk.
“With five million people worldwide predicted to have kidney failure by 2035 this is a major breakthrough.”
The UK National Kidney Federation said: “The exciting research from [the trial] is the first positive dedicated trial of an antidiabetic agent in this area, showing how under-recognised the irreversible impact of chronic kidney disease and type 2 diabetes has been up until now.”
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks