Long Covid ‘changes brains of people differently to those who recover from virus’
More than two million people in the UK are thought to be suffering from long Covid and many report ‘brain fog’, perstistent fatigue and digestive problems.
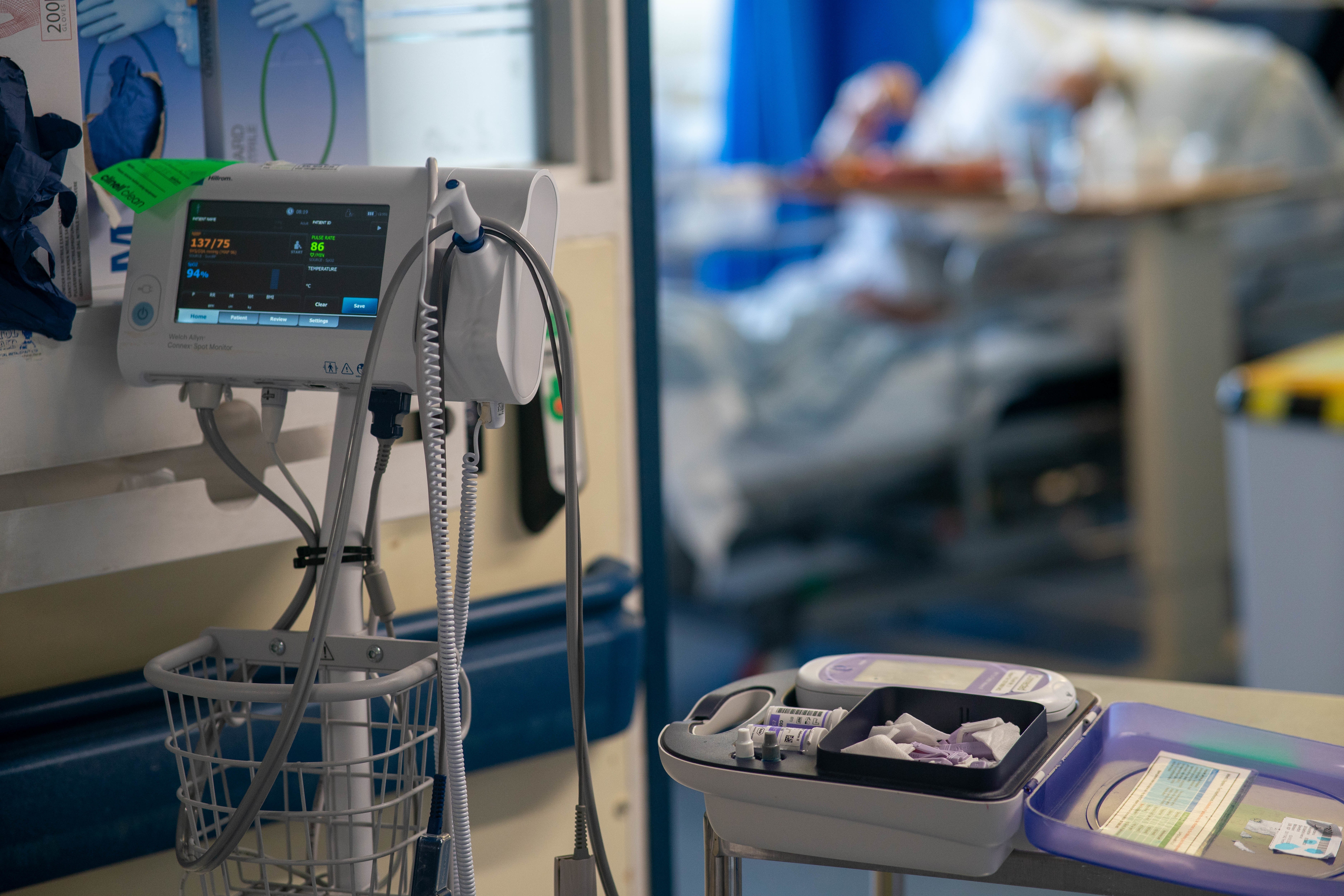
Long Covid alters the brains of people differently to those who recovered from the virus, new study reveals.
An estimated 2 million people in the UK reported symptoms of ‘long covid’ – an illness that continues to debilitate people long after initial Covid symptoms – according to the Office of National Statistics.
People with long Covid have reported a range of symptoms - including difficulty concentrating or “brain fog”, change in sense of smell or taste, persistent fatigue, joint and muscle pain, shortness of breath and digestive problems.
The symptoms can persist for long periods of time, and a new study by German scientists suggest sufferers of long Covid can feel symptoms years after their initial infection.
The study estimated as many as 10-25 per cent of people diagnosed with the virus suffer from long Covid.
Rachel Gristock, 49, was first diagnosed was Covid-19 in March 2020 at the beginning of the pandemic and has felt the effects more than three years later.

Speaking to The Independent, Miss Gristock said: “Covid first affected me quite badly for three weeks, and a few months later I still didn’t feel like myself.
“I was tired all the time, and my body was swelling up constantly, I couldn’t even think straight.”
She first noticed her symptoms at work, where she struggled to pay attention during meetings and manage the team she oversaw.
“I’ve lost 30kg because I can’t even eat properly, and I have to carefully manage my energy levels to get through the days. Some days I am okay and other days I’m peeled to the living room sofa. I struggle to cook dinner for my two children sometimes.”
Miss Gristock had to move to part-time work due to her debilitating symptoms and has had financial issues as a result.
She said she still suffers from chronic fatigue and cannot drive at night because her eyesight has been affected, though her inflammation has got better.
“It feels like I have a really bad case of the flu every single day,” she added.
The group of researchers, led by Dr Alexander Rau, of University Hospital Freiburg, found that people with long Covid exhibit patterns of changes in the brain that are different from fully recovered Covid-19 patients.
They used diffusion microstructure imaging (DMI), a new MRI technique, to detect the changes.
Dr Alexander Rau said: “To the best of our knowledge, this is the first study comparing patients with long Covid to both a group without history of Covid-19 and a group that went through a Covid-19 infection but is subjectively unimpaired.”
He explained that DMI looks at the movement of water molecules in tissues, and by studying how water molecules move in different directions and at various speeds, DMI can provide detailed information on the microstructure of the brain.
This means scientists can detect very small changes in the brain, not detectable with conventional MRI.
Dr Rau and his team compared MRI brain scans of three groups: 89 patients with long Covid, 38 that had contracted Covid-19 but did not report any long-term symptoms, and 46 healthy controls with no history of Covid.
The researchers first compared the cerebral structure of the three groups to test for atrophy and any other abnormalities, then used DMI to gain deeper details into the brain.
The three groups were compared to reveal group differences in the brain’s microstructure, and DMI parameters were read for the gray matter in the brain.
Whole brain analyses was also used to reveal the spatial distribution of alterations and associations with clinical data, including long Covid symptoms such as fatigue, cognitive impairment or impaired sense of smell.
The results showed no brain volume loss or any other lesions that might explain the symptoms of long Covid.
However, Covid-19 infection induced a “specific pattern” of microstructural changes in various brain regions, and the pattern differed between those who had long Covid and those who did not.
Dr Rau said: “This study allows for an in vivo insight on the impact of Covid-19 on the brain.
“Here, we noted gray matter alterations in both patients with long-Covid and those unimpaired after a Covid-19 infection.
“Interestingly, we not only noted widespread microstructural alterations in patients with long Covid, but also in those unimpaired after having contracted Covid-19.”
The findings also revealed a correlation between microstructural changes and symptom-specific brain networks associated with impaired cognition, sense of smell and fatigue.
Dr Rau added: “Expression of post-Covid symptoms was associated with specific affected cerebral networks, suggesting a pathophysiological basis of this syndrome.”
The team said that, despite the new brain imaging findings, it remains “unclear” why some people develop long Covid while others do not, although previous studies have identified risk factors including being female, older age, higher body mass index (BMI) and smoking.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks