Maternity failings account for the majority of the NHS’s £13bn spend on negligence
The parents of twins Harry and Henry Jackson, who died following hospital failings, have called for the NHS to learn lessons

Maternity failings continue to account for the majority of billions of pounds spent by the NHS on clinical negligence claims, as an NHS body warns of the “devastating” consequences of poor care.
Two-thirds of the £13bn spent by the NHS in 2021-21 in respect of negligence claims was related to maternity care, according to new data.
A report released by NHS Resolution said it was “a stark reminder that although the NHS remains one of the safest healthcare systems in the world within which to give birth, avoidable errors within maternity can have devastating consequences for the child, mother and wider family, as well as the NHS staff involved.”
According to the figures, 1,243 obstetric-related negligence claims were reported to the NHS in 2021-22, up from 1,157 in the previous year.
The data also shows that 200 claims relating to cerebral palsy or brain damage were received in 2021-22 – a decrease from the previous year, in which there were 250.
The organisation said that the growth in obstetrics claims over the past three years was due to trusts reporting cases of cerebral palsy and brain damage earlier through its early notification scheme, which was launched in 2017.
Earlier this year, the landmark report into maternity failings at the Shrewsbury and Telford Hospital NHS Trust found that almost 300 incidents of death or brain damage had occurred over two decades as a result of poor care.
The chair of the Shrewsbury review, Donna Ockenden, has now begun a review into alleged poor care in hundreds of maternity-related cases at the Nottingham University Hospitals NHS Trust. A third review, into failings at the East Kent Hospitals Foundation Trust, is also expected to be published later this year.
According to the organisation’s annual report, the overall cost of harm in the NHS reached £13bn in 2021-22 – up from £7.9bn in 2020-21.
Much of this increase is related to changes made by the Treasury in the way in which claims are calculated. However, NHS Resolution said that without these changes, the cost of harm would still have increased to £8.7bn as a result of a higher volume of claims linked to increased activity in the NHS.
The report said: “Obstetrics claims accounted for 62 per cent of all clinical claims by value received in the year, highlighting the underlying impact of the financial costs of maternity indemnity payments, alongside the impact of harm on patients, families and healthcare staff.”
The second biggest area for clinical negligence claims in 2021-22 was emergency medicine, which had 1,229 claims, followed by orthopaedic surgery, which accounted for 1,203 claims.
‘Catastrophic’ consequences
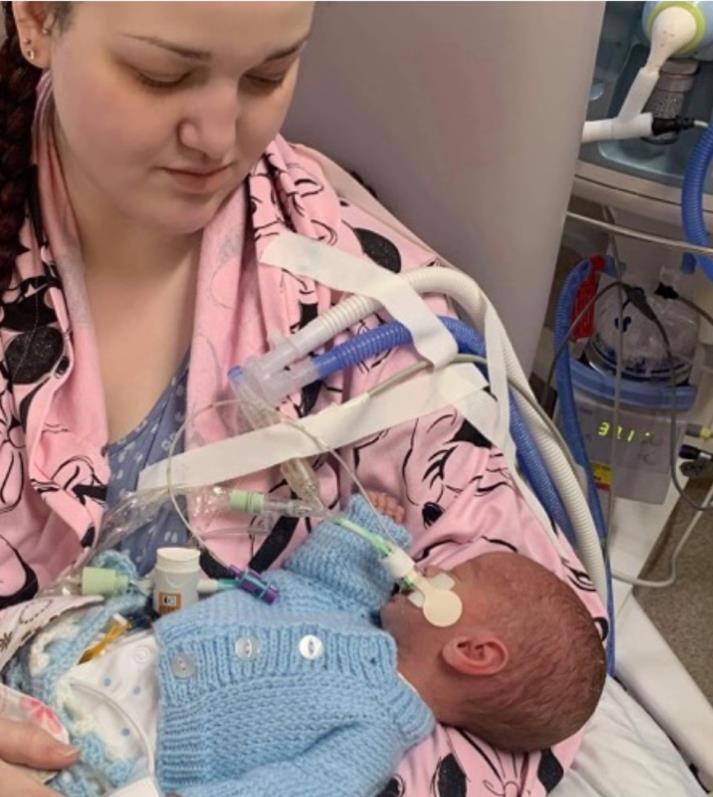
The news about maternity claims comes as Siobhan Weir and Luke Jackson, the parents of twins Harry and Henry Jackson, called for the NHS to learn lessons after an inquest found multiple failings in their babies’ care by maternity services in Sheffield.
Harry died stillborn following an emergency caesarean in June 2021 at the Jessop Wing, run by Sheffield Teaching Hospitals NHS Foundation Trust, and his brother Henry died six days later. The Jessop wing is currently rated inadequate by the Care Quality Commission.
An inquest at Sheffield’s Medico-Legal Centre was told that Ms Weir had been admitted to the Jessop Wing three times prior to her caesarean, because of severe vomiting.
According to a report of the inquest provided by the lawyers representing the family, on the third admission, the pain in her abdomen was so severe that she could not tolerate the monitoring of the babies’ heart rates.
An investigation report by the trust found that the risks associated with not having the babies’ heart rates monitored were never explained to Ms Weir, and that the results of her observations were not reviewed by a medic.
The trust’s investigation found that there were “missed opportunities” to investigate the cause of Ms Weir’s persistent sickness during her pregnancy, along with a failure to recognise a deterioration in her condition. The organisation admitted that, had the twins been delivered sooner, they would have survived.
Ms Weir, a care-home worker, said: “It’s impossible to put into words how difficult it remains trying to come to terms with how Henry and Harry died. It’s difficult not to think how things could be different and both the boys could be at home, growing up and starting to cause mischief.
“Nothing will ever fill the void in our lives. I don’t think we’ll ever get over losing Harry and Henry, and we will continue to think about them every single day. They will always be a part of our family, and we’ll never stop loving them.”
Rosie Charlton, a lawyer at Irwin Mitchell, which represented the family, said after the hearing: “Sadly through our work we continue to see the catastrophic consequences that families are left to face following issues in maternity care. Behind each case is a human story of how families have been devastated.”
Sheffield Teaching Hospitals Foundation Trust was approached for comment.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks