Monkeypox signs and symptoms: What to look for and how it spreads
Tropical disease originating in Africa has spread across the world since May
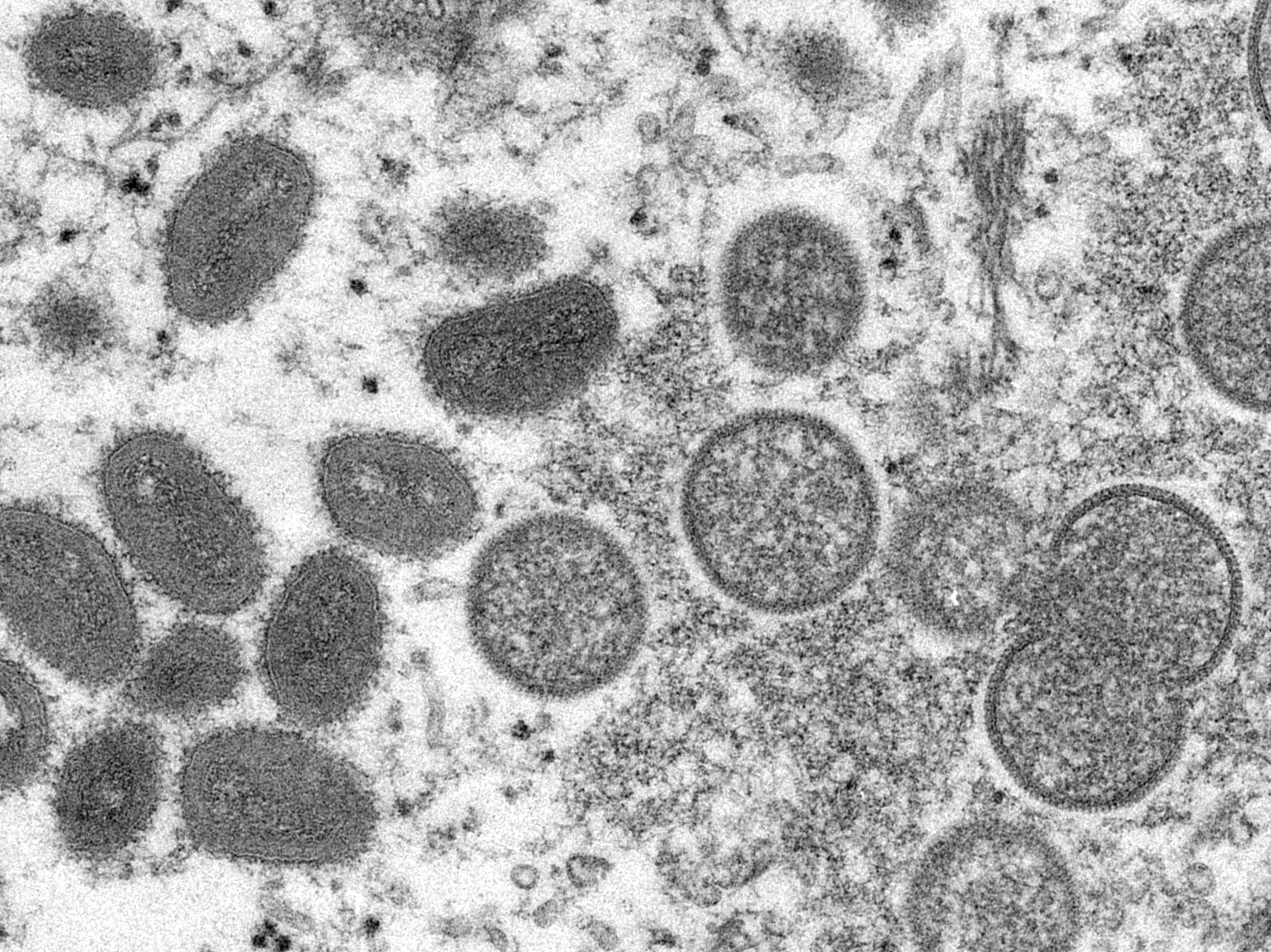
Monkeypox, a rare tropical disease spread by wild animals in West Africa, has unexpectedly spread abroad over the last three months, posing questions about what precisely it is and how dangerous it might be.
As of 22 August, there are 3,207 confirmed and 133 highly probable monkeypox cases in the UK or 3,340 in total, according to the UK Health Security Agency (UKHSA). Of these, 3,191 are in England.
In the US, which has 15,433 confirmed cases as of the same date, according to the Centres for Disease Control (CDC), monkeypox has now reached all 50 states and, more worryingly still, seen the first child infected in one instance in New York.
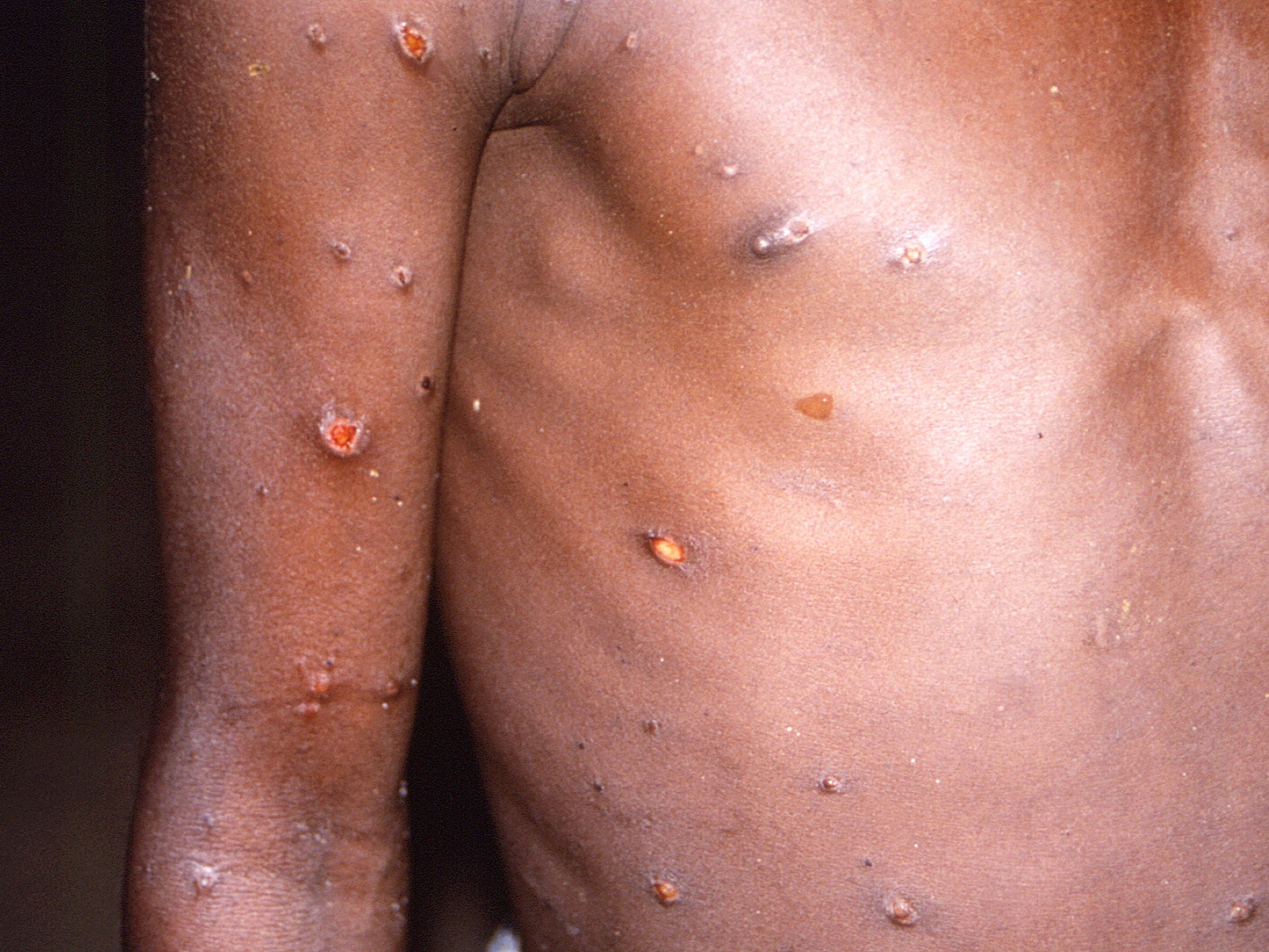
A relatively mild viral infection, the disease has a six-to-16 day incubation period and sees patients first suffer fever, headaches, swellings, back pain, aching muscles and a general listlessness in its opening stages.
Once that passes and the fever breaks, the sufferer will experience a skin eruption, in which a rash spreads across the face, followed by the rest of the body, most commonly the palms of the hands and soles of the feet.
The blemishes evolve from lesions into crusted blisters, which can then take three weeks to heal and disappear.
According to the CDC: “The main difference between symptoms of smallpox and monkeypox is that monkeypox causes lymph nodes to swell (lymphadenopathy) while smallpox does not.”
The virus can be difficult to diagnose without the aid of laboratory analysis because of its superficial similarity to other afflictions that result in a rash, such as chickenpox, measles, scabies and syphilis.
The WHO has traced the sickness to the tropical rainforests of Central and West Africa and defines it as a viral zoonotic disease – meaning it can be transmitted from animals to humans – with the first case recorded in what is now the Democratic Republic of Congo in 1970.
While it would have initially been transmitted to humans by contact with the blood or bodily fluids of contaminated primates, or via intermediary rodents such as tree squirrels and Gambian rats, it is much more likely to be caught from fellow humans.
At present there is no vaccine or specific treatment available but the pre-existing smallpox one has proven to be 85 per cent effective at combating the disease.
The UKHSA is currently investigating possible connections between infected patients and noted that four diagnosed together on Monday 16 May were all gay or bisexual men, warning that that could indicate the virus is being sexually transmitted among that community.
Mateo Prochazka, an infectious disease epidemiologist at UKHSA who is leading the agency’s investigation, said that shared circumstance was “highly suggestive of spread in sexual networks”.
Dr Susan Hopkins, chief medical adviser to the UKHSA, said: “We are particularly urging men who are gay and bisexual to be aware of any unusual rashes or lesions and to contact a sexual health service without delay.”
However, some scientists have cast doubt on the theory that monkeypox might have developed the ability to transmit sexually.
“It may not be actual transmitted by sexual intercourse rather than the close contact associated with sexual intercourse,” said Professor Keith Neal, an epidemiologist at the University of Nottingham.
“Further work looking at whether the virus is found in semen is required to say truly sexually transmitted.”
Professor Francois Balloux, director of UCL Genetics Institute, said: “I would urge some caution at this stage before concluding that monkeypox has morphed into a sexually transmitted infection.
"Monkeypox is not particularly transmissible and the number of cases to date where the route of transmission is known remains relatively small."
Very few of the newly infected individuals in the UK had travelled to a country where monkeypox is endemic, Nigeria, according to the UKHSA.
A man taken ill in Massachusetts during the present outbreak had also recently spent time in that same country, as had the two people diagnosed in Texas and Maryland last year and the travellers who brought the first cases to the UK in 2018.
However, the worst US outbreak seen so far, which resulted in 47 cases across six states in 2003, were caused by a shipment of infected animals arriving from Ghana.
As to how worried the public should be, Dr Michael Head, a senior research fellow in global health at the University of Southampton, admitted that there are “currently gaps in our knowledge”.
But he added that it “would be very unusual to see anything more than a handful of cases in any outbreak” and stressed that “we won’t be seeing Covid-style levels of transmission”.
The WHO puts the fatality rate for the disease at just one in ten.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments




Bookmark popover
Removed from bookmarks