NHS waiting times will increase without fresh investment, cash-strapped local health bodies warn
Rising inflation and population growth 'to cause £330m funding shortfall in next three years'
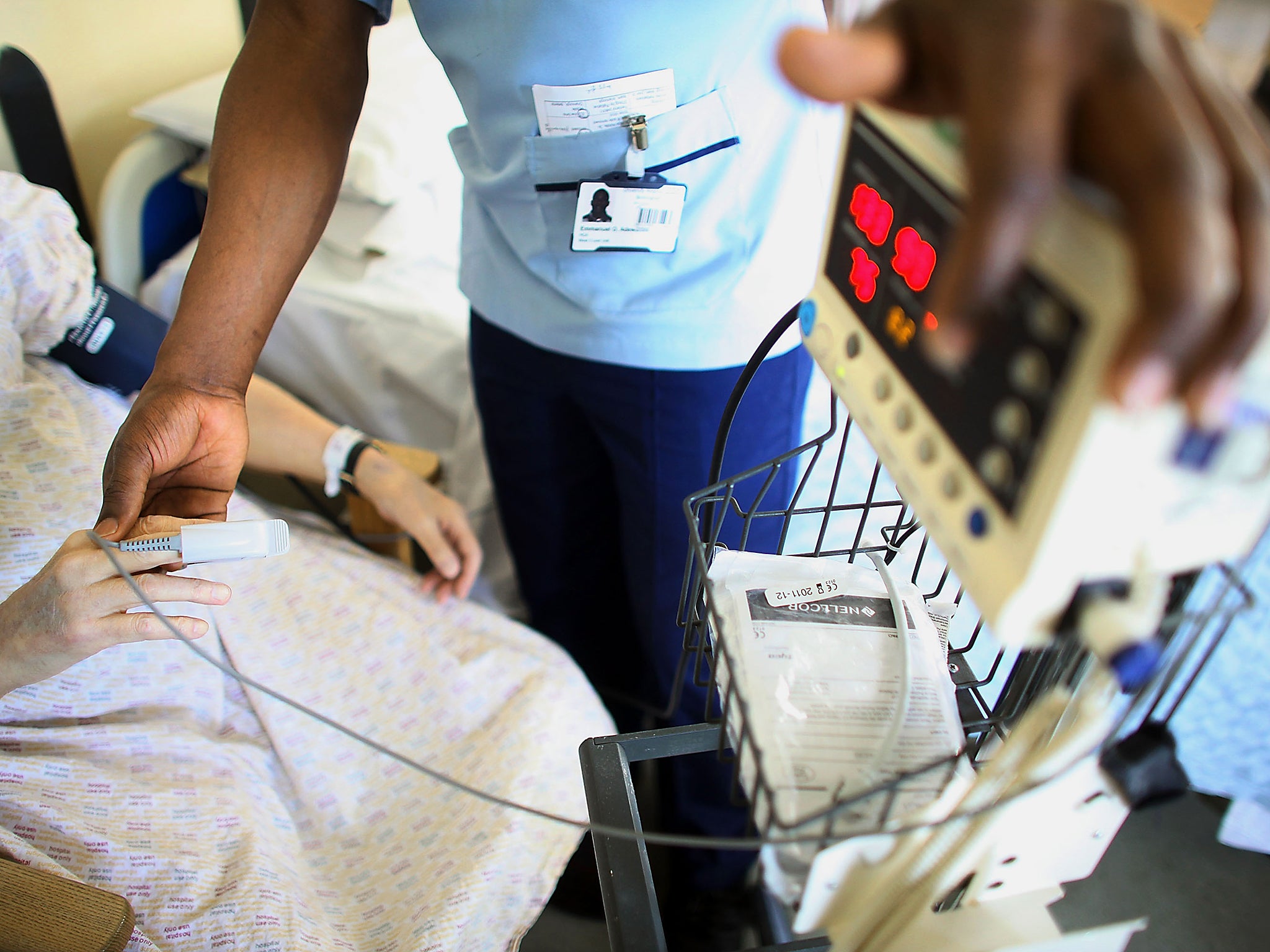
Patients may have to wait longer for NHS treatment as budgets are increasingly squeezed, the organisation that represents local health bodies across the country has warned.
A predicted real-terms funding drop of £330m in the next three years will result in a “slowing down” of access to routine care, said Julie Wood, the head of NHS Clinical Commissioners.
On paper, local health budgets appear to be increasing, with Theresa May claiming earlier this year that “funding is now at record levels for the NHS”. However, rising inflation and a growing population mean that by 2019-20, clinical commissioning groups (CCGs) – responsible for planning healthcare provision in each area of the UK – will face a shortfall of £5.72 per person on average compared to this year.
“The potential consequences will vary from area to area but could mean taking decisions about slowing down access to routine care and thus slowing down spend,” said Ms Wood in a statement. “It could be about looking at where services are provided and it could be about looking at the relative priority of where the NHS spends its [money].”
Simon Stevens, chief executive of NHS England, faced criticism in March after he indicated patients may have to wait longer than 18 weeks for non-urgent operations such as cataracts and hip replacements in a “trade off” for improvement in other areas.

A target that no patient should have to wait longer than 18 weeks for a hospital operation from when they are referred by their GP has been in place since 2004, but the number of patients waiting longer than that is rising. Politicians, charities and health experts condemned the suggestion the target could be softened, with shadow Health Secretary Jonathan Ashworth calling the plans “appalling”.
The Conservatives promised to retain the 18-week target in their general election manifesto, but lawyers have suggested Health Secretary Jeremy Hunt may have broken the law by failing to enforce it in his mandate to NHS England for 2017-18.
NHS Clinical Commissioners said other pressures including rising demand for services and an ageing population would add to difficulties faced around the country.
Ms Wood said savings could be made by withdrawing funding for medicines and treatments considered “low value”, adding to the list of former prescription items patients now have to pay for such as cough medicine and gluten-free food.
“We’ve been working with our members, NHS England and partners across the health and care system on identifying medicines and other items of low clinical value that we should not be spending the NHS pound on as it can be better used elsewhere,” she said.
The organisation said it was essential the £8bn of additional funding for the NHS by 2022-23 promised by the Tories in the lead-up to the general election was seen in local health budgets in the next two years.
Policy analysts called this pledge “deeply disappointing”, with The Health Foundation predicting it will create a funding gap of £12bn in the next four years when faced with increasing demand fuelled by an ageing population and the rising cost of new treatments.
Andrew Pepper, chair of the NHS Clinical Commissioners' Finance Forum, called for "realism about what the NHS can deliver, support for local decision-making and ring-fenced funding for transformation".
"Additional funding will help with this and we are calling on the Government to ensure that the money promised in the lead up to the election is to be allocated into CCG budgets sooner rather than later," he said.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks