A chilling warning from Britain’s most senior A&E doctor: Tory winter plan could kill thousands
Exclusive: Frail elderly and mentally ill will suffer most this winter, warns Dr Adrian Boyle
Government plans to prepare the NHS for winter have been criticised by the UK’s most senior A&E doctor, who warned that inadequate provision could see thousands of people die needlessly this year.
Dr Adrian Boyle, president of the Royal College of Emergency Medicine (RCEM), warned that plans drawn up this week are wholly insufficient, allowing for less than half of the beds needed to cope with the crisis.
He said that at least 11,000 additional staffed beds should be provided at hospitals across the country, while the prime minister has only pledged 5,000.
The NHS will also offer financial rewards to hospitals that hit waiting-time targets, which Dr Boyle said would mean they simply “game” the system and leave the most seriously ill patients waiting the longest.
The senior doctor said vulnerable elderly patients and the mentally ill would be affected most by the government’s poor planning.
He told The Independent: “If you just look at the figures, all the indicators of our target performance, 12-hour waits in hospital, are all going the wrong way. If we compare them to what was going on at the same time a year ago, it makes me anxious that we are heading towards a worse winter than we just had.”
Dr Boyle warned the government that it was “blithely sailing towards an iceberg”, and that if it allows this winter to be as bad as the last, “it will break the very people who keep this broken system creaking along”.
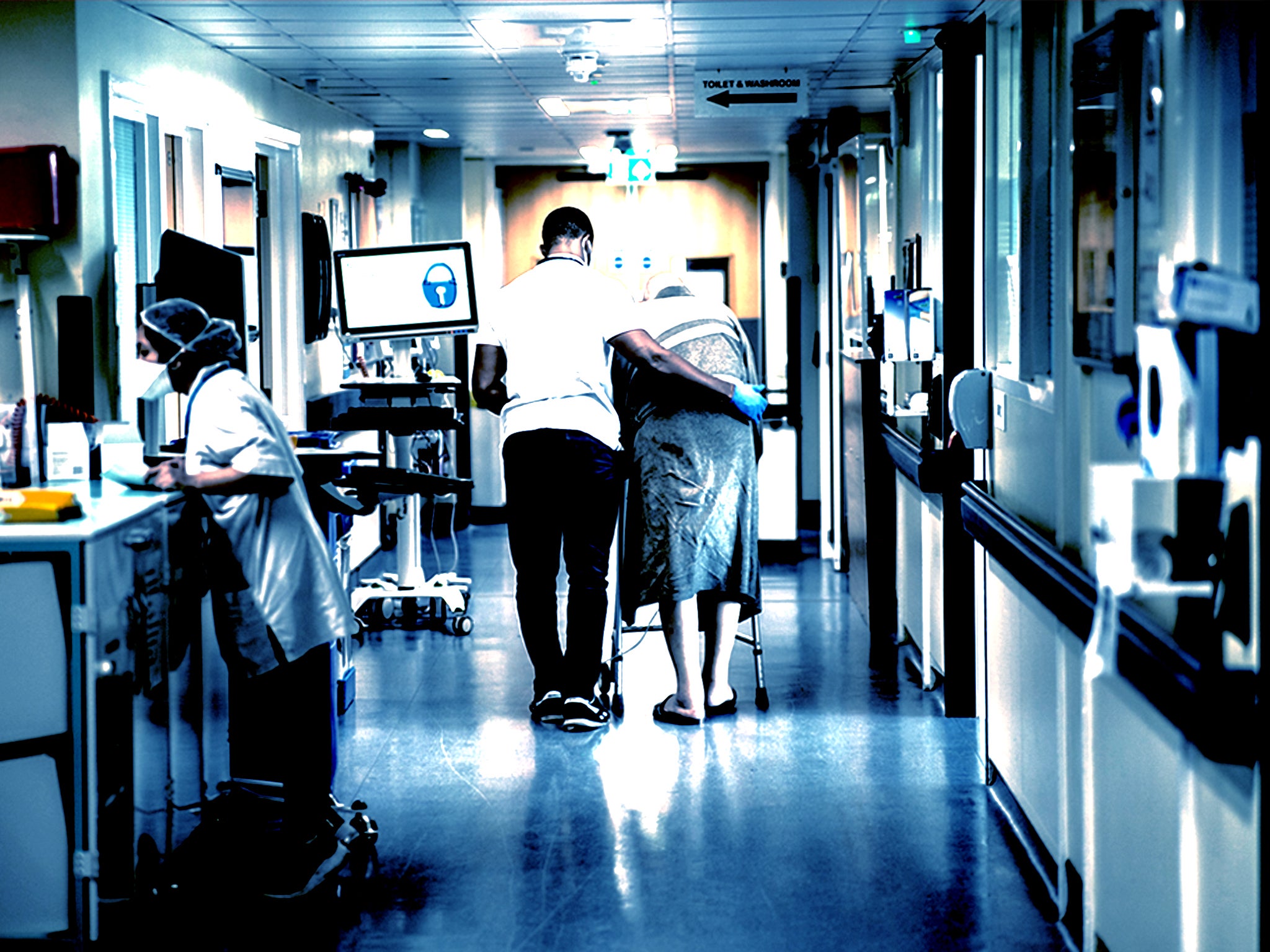
Last winter, more than 500 excess deaths a week were estimated to be linked to long waiting times, with a record number of patients spending more than 12 hours in A&E, as revealed by The Independent.
When asked whether the country was at risk of seeing even higher excess deaths during the coming winter, Dr Boyle said: “Yes, actually, I think we are.”
The winter plans were quietly announced this week, informing hospitals that they could access some of the £150m in capital funding available from the government if they hit targets for 80 per cent of their patients to be seen within four hours.
In addition, the Department of Health and Social Care (DHSC) announced that the NHS would have 5,000 extra hospital beds, 10,000 “virtual beds”, and “traffic control centres” focused on helping hospitals discharge patients into social care.
The 5,000 additional beds were originally promised last winter. However, the RCEM has pointed out that the health service now has 1,841 fewer beds compared with January this year.
Wes Streeting, Labour’s shadow health secretary, said: “Under the Conservatives, a winter crisis in the NHS has become an annual event. 13 years of broken promises and understaffing have run the health service into the ground.
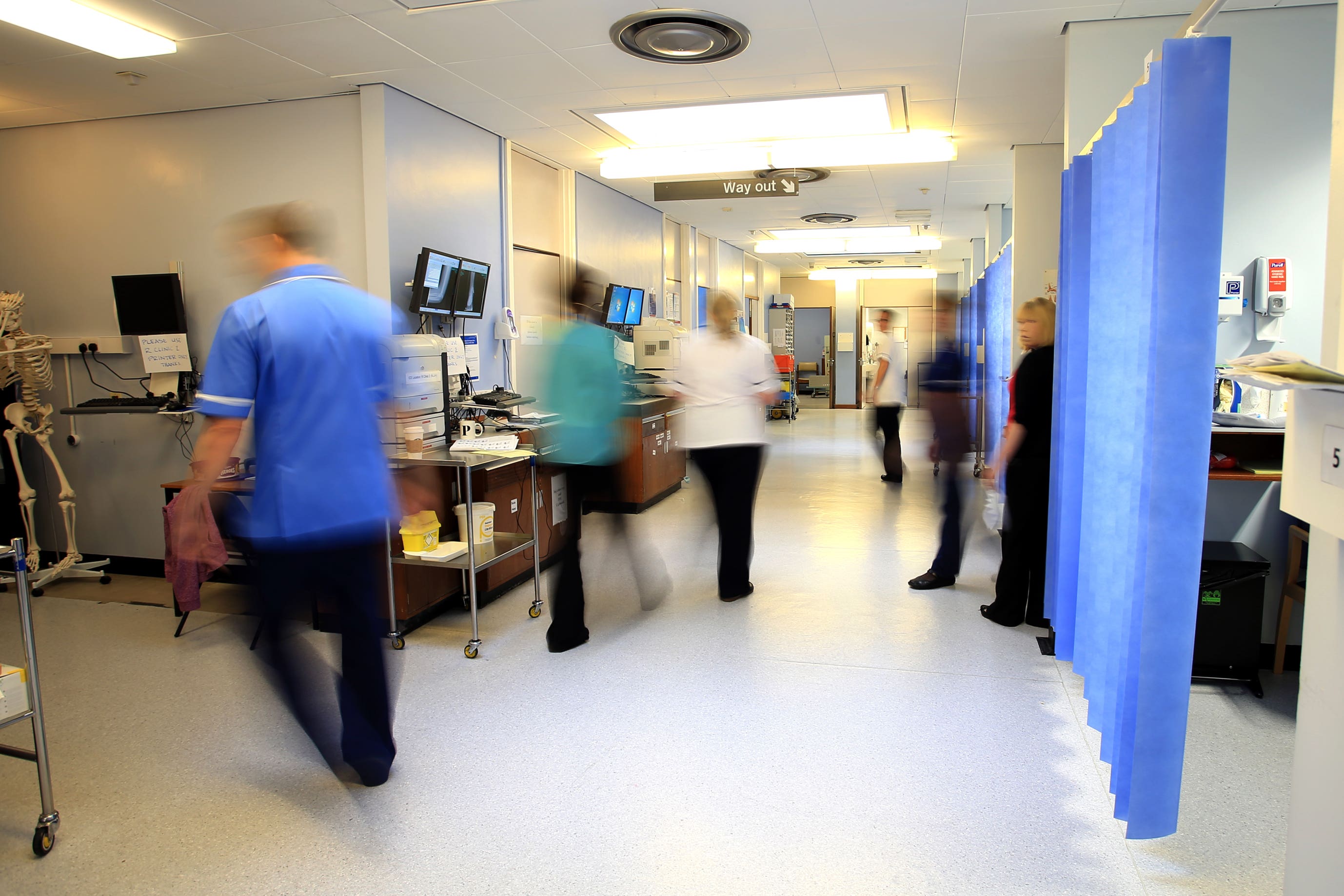
“The government must learn the lessons of last winter, or patients will pay the price ... It will fall to the next Labour government to restore the health service. We will deliver the reform and modernisation to ensure the NHS is there for us when we need it once again.”
Dr Boyle said he has “little confidence” that the government’s plan will “prevent queues of ambulances outside of hospitals, or the shameful sight of patients waiting for hours on trolleys in the corridors in A&Es [that are] full to bursting”.
He said that financial incentives for meeting targets are “distasteful”, and that they offer the wrong solutions, “detracting” from the most pressing problems such as hospital discharges and reducing the length of stay.
“People will start trying to look after and prioritise people who they think they can send home [within four hours] over patients who need admitting. They’ll just accept the patients who need admitting are going to spend longer than four hours ... It distorts clinical priorities away from those who aren’t the sickest,” said Dr Boyle.
“This would leave the most vulnerable, typically the elderly and those in a poor mental state, waiting for hours potentially on trolleys in corridors.”
Writing for The Independent, the senior medic said the money was likely to flow only to “affluent” areas, because A&E departments in deprived areas tend to struggle more with waiting times.
This week, the DHSC announced it was providing £600m to local authorities to help them deal with the problem of hospital discharges.

Dr Boyle said that while the money was “welcome”, it was “quite a small amount [and] spread over two years”, working out at around £1m per hospital.
The government is also facing strike action by doctors, who are campaigning for higher pay and better working conditions. Dr Boyle said he is “very worried” about walkouts continuing into the winter, adding: “I think we all want the strikes to be over.”
Health minister Helen Whately said: “Our urgent and emergency care recovery plan, backed by record funding, is already improving A&E performance and ambulance response times. Thanks to that plan, the NHS is getting 800 new ambulances, 5,000 extra hospital beds, and 10,000 virtual ward beds.”
An NHS England spokesperson said: “We have already seen significant improvements in ambulance and A&E services over recent months through initiatives in our urgent and emergency care recovery plan, which includes measures to increase bed capacity. The NHS will continue to build on this with our winter plan, which, after clinical engagement, was published on Thursday.
“With more than 12,000 patients every day in hospital despite being medically fit for discharge, a nationwide rollout of care transfer hubs will provide a one-stop [service] for staff to locate and coordinate the best and quickest discharge options for patients – either at home or into social or community care – which helps free up beds for other patients who need them, including those coming into emergency departments.”
They pointed to other plans focused on reducing A&E admissions, such as the increased use of same-day emergency care units and virtual wards.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments


Bookmark popover
Removed from bookmarks