Prostate cancer tests: Life saving or a nuisance?
After a simple blood test was introduced in 1994, the death rate from prostate cancer dropped by more than half. However, Jane E Brody notes how the disease is often unlikely to kill a patient, yet often causes anxiety and unnecessary treatment – sometimes leading to impotence, incontinence or both
We’ve long been schooled on the lifesaving value of early detection of potentially deadly cancer. So when a simple blood test was introduced in 1994 that could detect the possible presence of prostate cancer, the second-leading cause of cancer deaths among American men, it’s not hard to understand why it quickly became popular.
Suddenly, in the decades after approval of the test known as the PSA, for prostate-specific antigen, the number of men receiving a diagnosis of prostate cancer skyrocketed, along with the number undergoing biopsies of this walnut-size gland between the bladder and penis that produces the seminal fluid to nourish sperm.
The goal of screening is to find aggressive cancers early enough to reduce the risk of death, and national health statistics seem to justify the popularity of PSA screening. Today, 90 per cent of prostate cancers are found while the disease is still confined to the gland and its neighbours, and nearly 100 per cent of men with the disease survive five or more years. And indeed, the death rate from prostate cancer has dropped by more than half in the US since the PSA was approved as a screening tool by the Food and Drug Administration.
Nonetheless, controversy over the true value and necessity of annual PSA testing for most men has flourished for several reasons. In many men identified as having prostate cancer after PSA screening, the disease is neither aggressive nor likely to kill them before something else does.
In fact, a previously unknown prostate cancer is found at autopsy in more than a third of men who die in their 70s or older from some other cause.
Yet when a biopsy after an elevated PSA reveals cancer, even a cancer considered indolent, it can provoke considerable anxiety, and some men may choose to undergo unnecessary treatment that can cause impotence, incontinence or both.
The not-inconsequential problems of overdiagnosis and overtreatment for a cancer that is unlikely to threaten a man’s health or life has prompted attempts to develop appropriate guidelines for PSA screening, to determine which men without prostate-related symptoms should have a PSA test and how often, how the test results should be interpreted, and when follow-up biopsy and other testing is warranted.
As Dr Henry Rosevear, a urologist who endorses the value of the PSA, wrote in Urology Times, “Not everyone needs to be screened, not everyone found to have an elevated PSA needs to be biopsied, and Lord knows that not everyone with prostate cancer needs aggressive treatment.”
Men age 70 or older should be told that the potential harms of screening could outweigh the benefits
In most cases, prostate cancer is slow-growing, and a PSA level of less than 4 nanograms per ml of blood is considered within the range of normal. But when the PSA level rises precipitously, say from four to six or higher in a year’s time, doctors are likely to suggest a biopsy. Among men with an elevated PSA who are found on biopsy to have cancer, about 80 per cent have an indolent form of the disease that is highly unlikely to become life-threatening.
In May 2018, the US Preventive Services Task Force concluded that for men ages 55-69, the decision to have a PSA test should be made jointly by patients and their doctors based on a man’s preferences, values and risk factors.

Men with multiple health problems and a limited life expectancy, and those who would not opt for treatment if a cancer is detected, should not be screened, the task force said. And, it added, men age 70 or older should be told that the potential harms of screening could outweigh the benefits.
That said, there are possible exceptions that could tip the scale in favour of screening. PSA screening is a potential benefit for younger men with a strong family history of prostate or related cancers, men who carry a BRCA1 or BRCA2 mutation, and African-American men, who are more likely than others to develop an aggressive prostate cancer. For them, screening is best started at ages 40 or 45.
Among older men, screening can be beneficial to those 70 or over who are very healthy and expected to live another 10 years or longer. Dr H Ballentine Carter, urologist at Johns Hopkins Hospital, noted in an editorial in the journal Jama that “older age is associated with more aggressive prostate cancer; thus, a very healthy older man with the prospects of extended life might benefit from PSA testing”.
Complicating matters is the fact that circumstances other than cancer can result in an elevated PSA reading
“Nevertheless,” he added, “routine screening of average-risk men 70 years and older should be rare, because they are more likely than younger men to experience the harms of screening, diagnosis and treatment”.
Complicating matters is the fact that circumstances other than cancer can result in an elevated PSA reading. Among them are recent sexual activity, vigorous physical activity, bicycling, benign prostatic enlargement and inflammation of the prostate. Thus, the test is usually repeated some weeks later before further action is taken.
There are also men in whom the PSA level rises inexplicably and remains elevated despite a repeated inability to find any sign of cancer in their prostates.
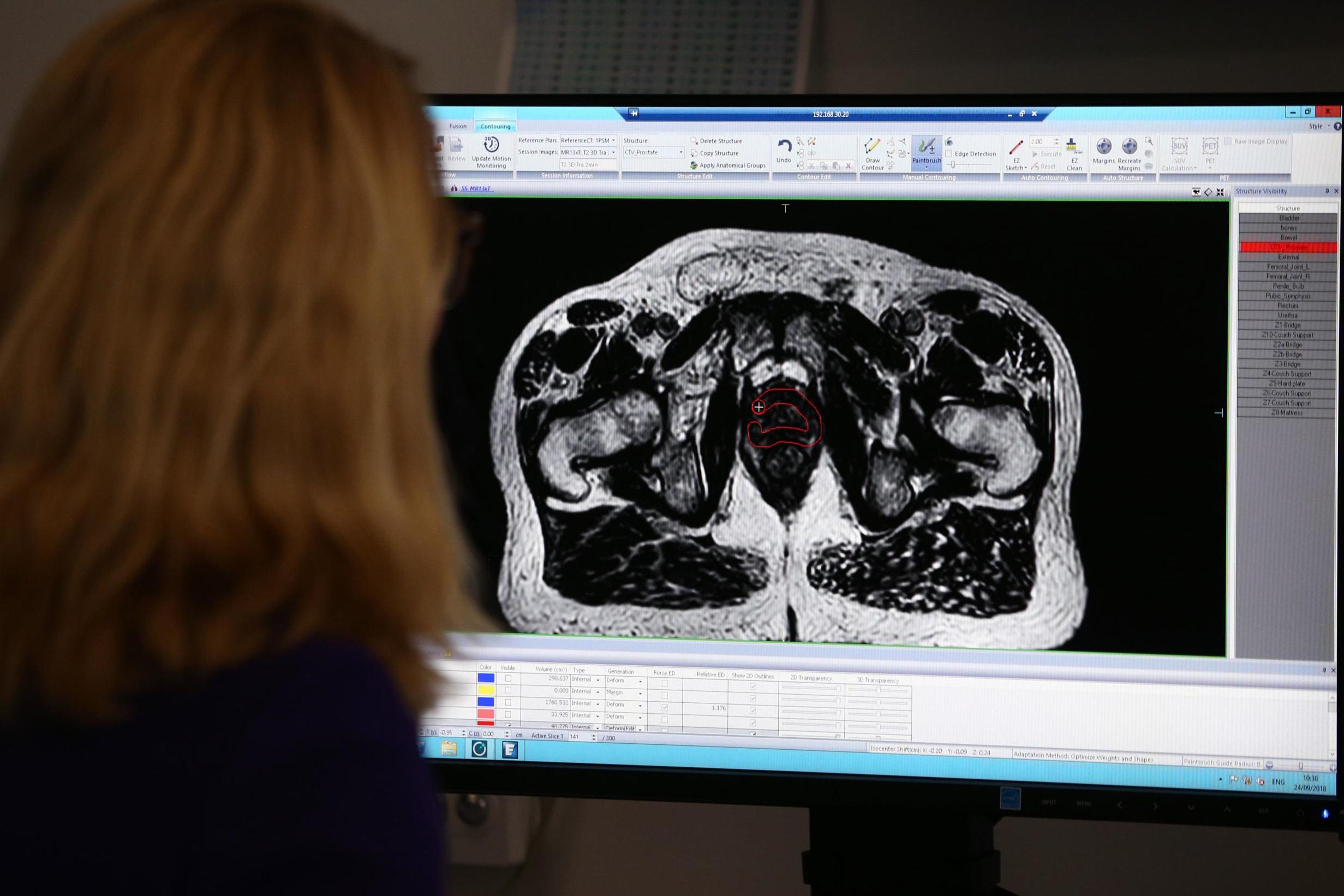
In the most definitive study done to date to assess the value of PSA screening, the European Randomised Study of Screening for Prostate Cancer concluded that 781 men ages 55-69 when they enrolled would have to be screened to prevent one man from dying of prostate cancer after 13 years. In this study, approximately one man in six who were screened was falsely identified as possibly having prostate cancer, and two-thirds of positive PSA results in the first round of screening were false positives.
Given the limitations of the PSA, researchers have been developing more refined tests that are better able to detect a worrisome cancer, reported Dr James Eastman of Memorial Sloan Kettering Cancer Centre in New York.
One is the 4Kscore test that combines the levels of four prostate-specific antigens with clinical information to estimate a man’s risk of having an aggressive cancer. The other, called the PHI, for Prostate Health Index, combines three different PSA measurements to better predict the presence of cancer.
Also under study is the use of an advanced form of MRI that can detect the presence of cancer with a higher risk of becoming lethal while overlooking low-risk disease.
Perhaps the measure that can currently do the most to reduce repeated biopsies and unnecessary treatment for prostate cancer when the PSA test is elevated is the growing popularity of active surveillance – periodic monitoring of men with a low-risk cancer. Only if the cancer starts growing or shows signs of becoming aggressive is treatment considered.
© The New York Times
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments