NHS at 70: How it took nearly a century for the health service to be formed
By the 1930s the cost of specialist and hospital care had reached the point at which it was beyond the means of a large proportion of the population. But from its early beginnings in 1854, it took 94 years for the service we needed to be formed. Andreas Whittam Smith documents the journey
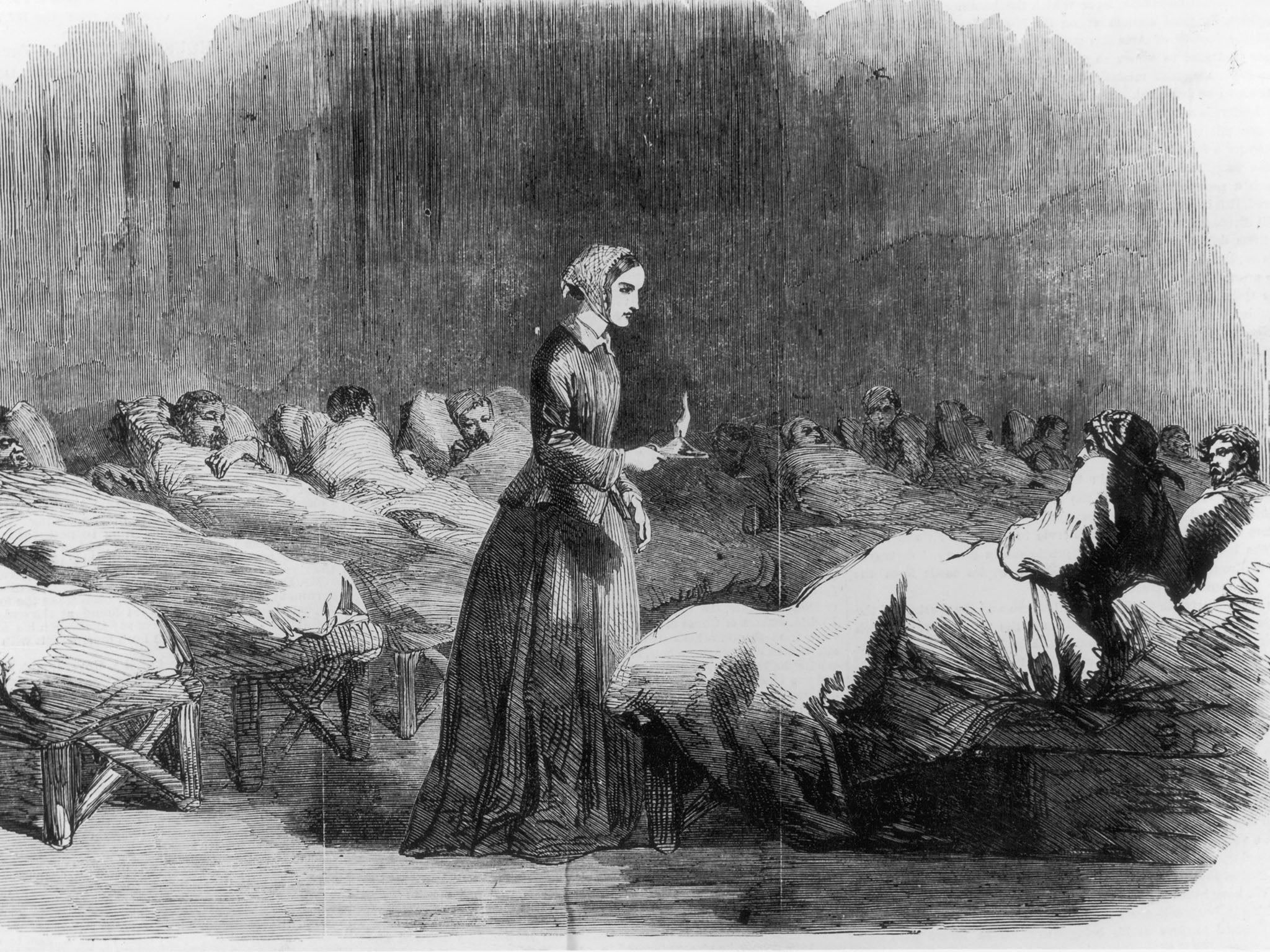
I would date the first glimmer of the idea of a national health service to 1854, when Florence Nightingale had arrived at the army hospital near Istanbul where British soldiers wounded in the Crimean War were being cared for. During her first winter, 4,077 soldiers died in the hospital, but most of these had suffered from illnesses such as typhus, typhoid, cholera and dysentery rather than from battle wounds.
So Nightingale came to the conclusion that the high death rates were mainly due to poor nutrition, lack of supplies, stale air and overworking of the soldiers. That is what she told the Royal Commission on the Health of the Army.
In other words, this was already civil society, in the person of Nightingale, urging the state to improve its performance in the matter, not yet of the health of the nation as a whole, but in one rather important bit of it, the British army.
In 1875, 20 years later, the prime minister of the day, Benjamin Disraeli, built on Nightingale’s ideas. He sponsored a Public Health Act, whose purpose was to codify previous measures aimed at combatting filthy urban living conditions which, it was now accepted, caused various health threats, including the spread of many diseases such as cholera and typhus.
The act provided local authorities with new powers to purchase, repair or create sewers, to control water supplies, to regulate cellars and lodging houses and to establish by-laws for controlling new streets and buildings.
Then, 30 years later, acknowledging that poverty was one of the root causes of ill health, local authorities were given an additional power: the right to furnish meals to impoverished children.
In a House of Commons debate on this measure, the first speaker, Mr WT Wilson, who represented Westhoughton near Bolton – then a centre for coal mining, cotton-spinning and textile manufacture – said he did not think anyone in the house would doubt that a very large number of children went to school without food or underfed, and the object of the bill was to provide that meals should be given to such children.
That was in 1906. Five years later came the first major move towards a comprehensive health scheme. Under the National Insurance Act of 1911, virtually all low-income workers were compulsorily insured and in the event of illness, were guaranteed for themselves, but not their dependents, free drugs and the care of a physician.
The scheme was to be jointly financed by the employer, the employee and the government. Free drugs were as much a statutory benefit for the insured as the services of a general practitioner. This has been seen as the key legislative achievement of Asquith’s Liberal government of 1908 to 1915 just as the creation of the National Health Service itself was to be of the Atlee government of 1945 to 1951.
What this history is telling us is that a really big idea such as a national health service can only be realised in long-drawn-out stages. From time to time, for instance, the notion of a “national education service” is discussed, but as yet there is no feeling that we are even moving through the stages necessary for the attainment of that ideal.

The difference is perhaps that the provision of medical care became more and more expensive. By the 1930s, the cost of specialist and hospital care had reached the point at which it was beyond the means of a large proportion of the population. The sources of funding – charity, contributory schemes, health insurance and self-help – were all failing to meet the need.
Hospitals that had once required a few general practitioners and a small nursing and administrative staff now demanded the services of a small army or nurses and auxiliaries in addition to laboratory technicians, dietitians, occupational therapists and many other specialists. At the same time, medical discoveries followed one another in rapid succession, and each tended to find a broader and more expensive application. In a well-known provincial hospital there were fewer than 600 X-ray examinations in 1918. By the end of the 1940s, nearly 20,000 were required annually. Cost was the factor more than any other that rendered inevitable the creation of a state medical service.
A white paper issued in February 1944 identified as serious shortcomings the disorganisation of the hospital service, the inadequacy and inaccessibility of specialised medicine and surgery for many patients, and the piecemeal and uncoordinated health services of the local authorities. The demoralisation of the doctors could also have been added to this list. For the net income of the medical profession was too low. Since the per-head payment or capitation fees under the National Insurance Act was small, most doctors preferred private patients. However, a royal commission in 1926 found no evidence that insured patients received an inferior service. Instead there was a growing tendency among physicians to refer patients to the outpatient departments of hospitals.

The attitude of the British Medical Association was that while doctors were willing enough to accept as unavoidable a more comprehensive free medical service for patients unable to pay, they wanted an income limit so as to preserve for private practice all those with incomes above that level. In short, they believed that a general policy of opposition to the proposals of the government offered the best hope for good financial terms.
By the end of the Second World War, there was overwhelming support from all political parties for some sort of health service. The ordeal of war had had a levelling effect. The Beveridge Report, which proposed widespread reforms to the system of social welfare to address what William Beveridge identified as five “giant evils” in society: squalor, ignorance, want, idleness, and disease. Published in the midst of World War II, the report promised rewards for everyone’s sacrifices. It was overwhelmingly popular with the public.
Finally, Sir Winston Churchill, speaking as prime minister in the spring of 1944, affirmed that it was the policy of the government to establish a national health service that would make accessible to all, irrespective of social class or means, adequate and modern social care. The high and rising cost of medical care was the key consideration. Healthcare shouldn’t be rationed by price.
As we celebrate the 70th anniversary of the NHS, that is the key achievement. By contrast, this gruesome story has just arrived from across the Atlantic. A tweet from the New York subway system describes “an awful scene”. A woman’s leg got stuck in the gap between the train and the platform. It was twisted and bloody. Skin came off. She’s in agony and weeping. Just as upsetting she begged no one call an ambulance. “It’s $3,000,” she wailed. “I can’t afford that.” That’s why we have the National Health Service.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks