NHS at 70: The scientific breakthroughs that revolutionised the service
The NHS’s greatest innovation was also the simplest: free healthcare for all. But it didn’t stop there. Josh Gabbatiss charts the life-saving technologies pioneered by our health service
When the NHS was launched in July 1948 it marked a radical shift in the UK’s healthcare system, but there were still plenty of shifts to come.
Many of the life-saving therapies that are now taken for granted simply did not exist when the service was created. Most vaccination programmes were not in place, cancer was still largely a death sentence and no one had heard of DNA.
Though its greatest innovation was also the simplest – to provide healthcare to the millions of British people who could not afford it – in the decades that have followed, scientific breakthroughs have profoundly altered the way the NHS operates.
Mass vaccination
Vaccinations were still in their infancy when the NHS began, but their introduction helped define the service and its goal to prevent illness wherever possible.
Smallpox vaccination had been compulsory but was discontinued as the disease was eradicated from British shores. However, in the 1940s many other infectious diseases were still having a devastating impact.
“Both my parents were GPs in Somerset and they could remember very well people dying from diphtheria – people suffering from diseases that we just don’t see these days,” says Professor Peter Openshaw, director of the Centre for Respiratory Infection at Imperial College London.
“It was really with the advent of the NHS that the vaccination programme has grown and become enormously sophisticated.”
Shortly after the NHS got going, mass vaccinations were introduced for some of the most serious afflictions of the day, including TB and whooping cough.
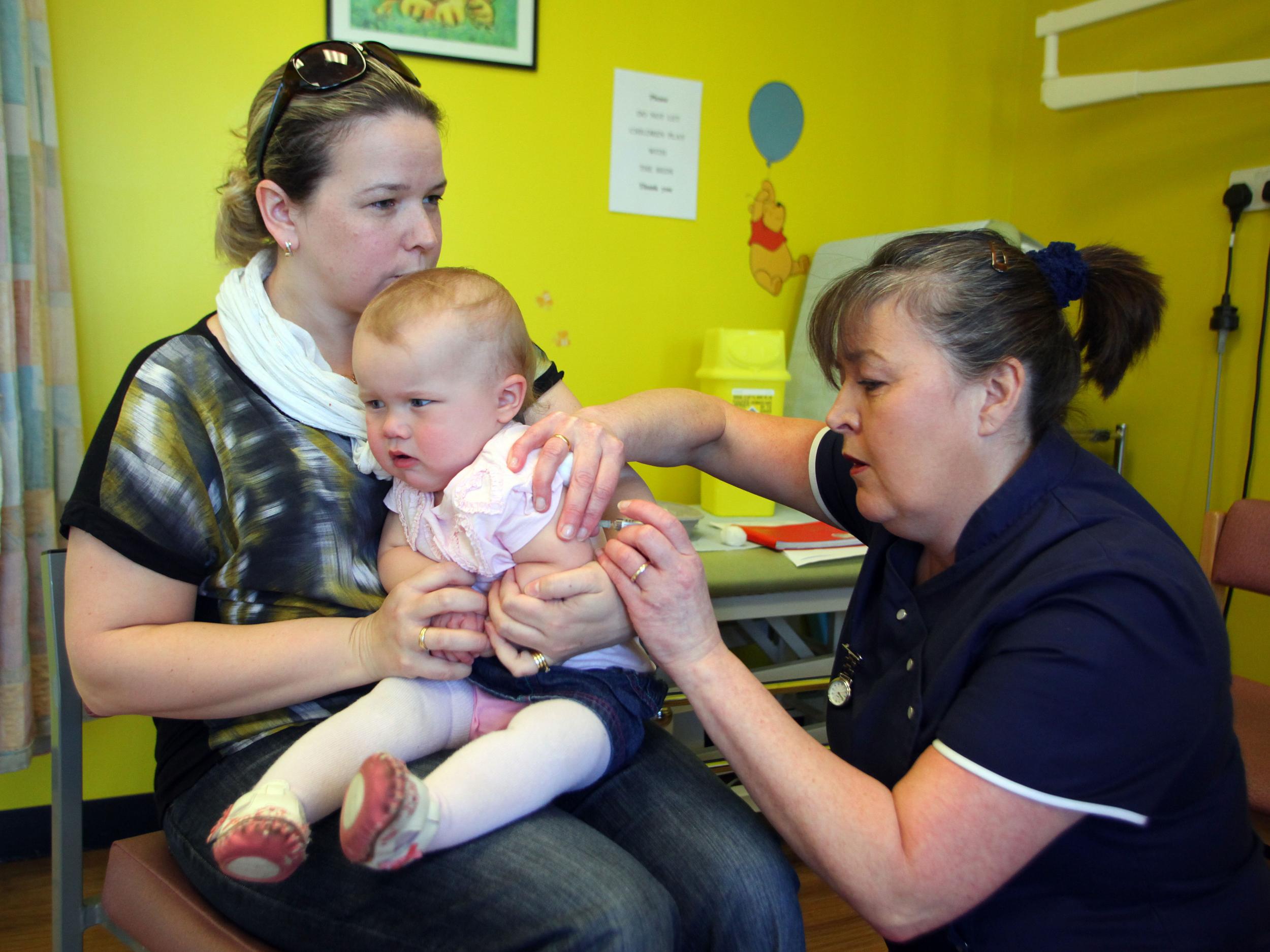
Soon enough diseases that had caused mass death and – in the case of polio – left many people permanently disabled, had gone the way of smallpox, with rates of infection dropping significantly.
According to Professor Openshaw, it was the NHS and its focus on prevention rather than just treatment that allowed these radical changes to sweep across the country. Doctors were incentivised to stop people from becoming ill rather than “just making money out of treating people who are sick”.
Today, so-called “anti-vaxxers” are waging war on vaccines, and Professor Openshaw says this has been the case ever since the earliest days of vaccines when they were described as “unnatural, animalistic and anti-religious”.
While some of the NHS’s campaigns have faced similar opposition, the tightening of vaccine regulations has ensured they now work more effectively than ever before.
“The amazing thing is how much is still going on – in the 1950s there were so many vaccines being introduced but just in the last 15 to 20 years there has been a whole slew of improved, new vaccines,” says Professor Openshaw.
“Things are just gradually getting better and better.”
Organ transplants
The first successful organ transplant was performed by Boston-based surgeon Dr Joseph Murray in 1954. A kidney was removed from one donor and transferred to his identical twin brother, saving his life and paving the way for surgeries that continue to benefit thousands every year.
Though initially slow to spread across the Atlantic, six years later Sir Michael Woodruff performed a similar procedure on another set of identical twin brothers at the Royal Infirmary of Edinburgh.
The operation marked the first of many successful NHS transplants operations, with the first UK heart and lung transplants following in 1968. However, procedures would be limited until more sophisticated drugs were developed that prevented bodies from rejecting the new organs.
Both my parents were GPs in Somerset and they could remember very well people dying from diphtheria – people suffering from diseases that we just don’t see these days
Today, nearly 5,000 organ transplants are performed every year in the UK, and 2017 saw the number of people alive due to organ donation hit 50,000 for the first time.
Transplant operations have become ever-more ambitious, with the nation’s first ever hand transplant taking place at Leeds General Infirmary in 2012.
However, despite the introduction of the NHS organ donor register in 1994, demand for organs in general still outstrips supply. As of 2015 there were more than 7,000 people on the transplant waiting list.
In vitro fertilisation
A true British success story, the first IVF baby – Louise Brown – was born at Oldham General Hospital in 1978.
Since then IVF has become standard procedure, offering couples who would otherwise be unable to conceive the joy of having children.
Using the technique, doctors are able to combine a couple’s eggs and sperm in a laboratory before inserting the fertilised egg into the woman’s womb to develop.
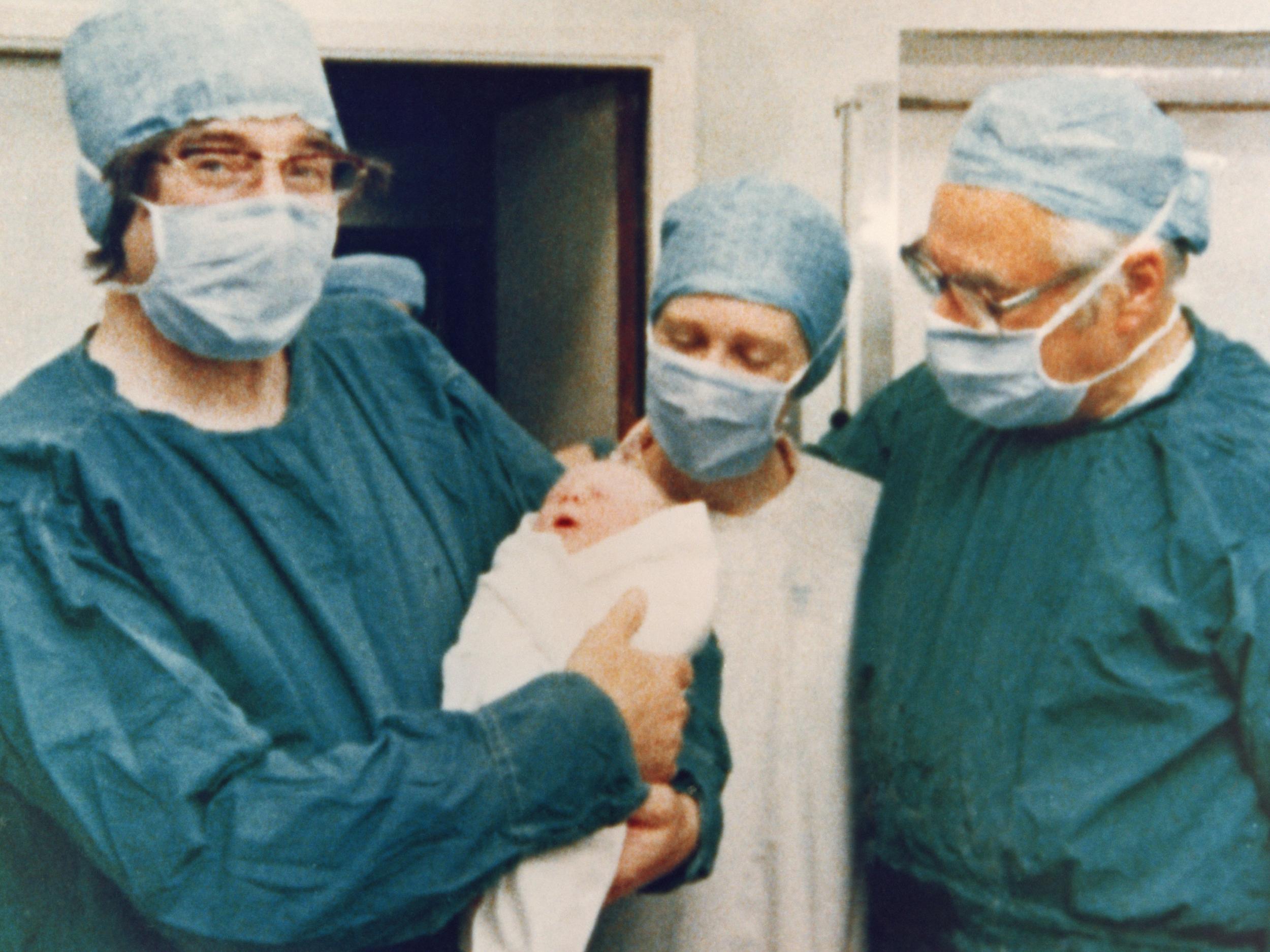
While today the treatment is available in NHS practices up and down the country, the journey to IVF was not smooth sailing for scientist Robert Edwards and gynaecologist Patrick Steptoe, who began working on the procedure in the 1960s.
In a premonition of the moral panics that would grip the nation in later years when stories broke about cloning and “designer babies”, people were alarmed at the prospect of embryos being created in test tubes.
The amazing thing is how much is still going on – in the 1950s there were so many vaccines being introduced but just in the last 15 to 20 years there has been a whole slew of improved, new vaccines
“It was developed against considerable hostility and scepticism, which I think is difficult to understand in these liberal days,” says Professor Richard Anderson, a reproductive scientist at the University of Edinburgh.
“Forty years is a long time in the UK for public and scientific attitudes.”
Though millions of babies have been born using IVF, the procedure is not straightforward and still only has a success rate of around 30 per cent. What is more, the cost per treatment has made many services across the country unwilling to commit the necessary funds.
“From the NHS’s point of view the provision is very patchy across England and Wales particularly – and in some areas is lamentable,” says Professor Anderson.
Keyhole surgery
First employed by the NHS in an operation to remove a gallbladder in 1980, keyhole – or laparoscopic – techniques have revolutionised the way surgery is performed.
In a keyhole procedure, a thin telescopic rod connected to a tiny camera is used to operate via small incisions made in patients’ abdomens.
Thanks to this pioneering new way of performing surgery, an operation that would once have involved an enormous incision can now be undertaken with minimal damage to people’s bodies.
Not only did this mean a shorter hospital stay for patients, the development of these procedures has meant less pain and lower risk of infections.
The widespread roll-out of keyhole methods in the 1990s has led to laparoscopy being applied in a range of conditions in the abdomen or pelvis, and new techniques are constantly being developed.
In 2014, cardiac surgeon Vinnie Bapat and his team at St Thomas’ Hospital were able to complete a heart valve replacement on a beating heart for the first time in the world.
Mr Bapat welcomed the opportunity to “give our sickest patients a chance of survival and a better quality of life”.
Crucially, the surgeons were able to complete their work through a tiny opening in the chest, avoiding the risks of open heart surgery and completing the operation in just over half an hour.
Cancer treatment
After decades of mixed success experimenting with surgery and radiation therapies, anti-cancer drugs first came on the scene around the time of the NHS’s inception in the 1940s.
The first chemotherapy drug to be developed came from an unlikely source. After blighting the soldiers of First World War trenches, the poison gas nitrogen mustard was rebranded as mustine after doctors found they could use it to treat lymphoma.
But it was the American pathologist Sidney Farber – widely regarded as the “father of modern chemotherapy” – who paved the way for future treatments with his work on childhood leukaemia.

Over time the combination of drugs, radiation and surgery would become the standard means by which doctors fought back against cancer.
In the years that followed, many discoveries emerged that would form the bedrock of current strategies to either catch cancer early or prevent it altogether.
After observing an alarming increase in lung cancer incidence, Sir Richard Doll studied patients in 20 London hospitals throughout the 1940s. He assumed the cancer was caused by fumes from coal plants or cars, and was surprised to find instead that smokers were far more likely to develop the disease.
It was really with the advent of the NHS that the vaccination programme has grown and become enormously sophisticated
Many frustrating years of campaigning followed before the establishment accepted these conclusions, but now they form the basis of campaigns that aim to keep lung cancer rates far below 1940s levels. Two years after Sir Richard’s death in 2005, smoking was banned altogether in virtually all public spaces.
Screening programmes have been instrumental in locating and dealing with cancers at an early stage.
Some of the first studies of cervical screening were conducted in the 1950s by Cancer Research UK scientists, and these have given rise to the current screening programme that now saves thousands of lives every year.
In 1988, the first comprehensive national breast-screening programme was introduced in an effort to reduce cancer deaths in women over 50. Combined with improvements in drug therapies, screening has cut breast cancer deaths by a fifth – a trend that looks set to continue.
Advances in genetics and gene therapies
In 1953, Cambridge University scientists James Watson and Francis Crick announced a discovery that would turn the world upside down.
“We wish to suggest a structure for the salt of deoxyribonucleic acid (DNA),” they stated in the introduction to the scientific paper describing their discovery.
“This structure has novel features which are of considerable biological interest.”
This considerable understatement marked the beginning of genetics in medicine.
Understanding DNA ultimately meant understanding the diseases that are caused by defective genes, such as cystic fibrosis or sickle cell disease. The mapping of the human genome, which was completed in 2003, took the field of genetics even further.
Now, doctors hope that diseases that have always been viewed as inherited and therefore incurable could one day be treated with gene therapies.
Exciting work by researchers at NHS hospitals has shown that for conditions like cystic fibrosis, doctors may one day be able to insert healthy copies of defective genes into patients and rid them of it altogether.
Though research in this area still has a long way to go, gene therapies could one day be the answer to many previously incurable afflictions and genetic analysis could be widely utilised to screen people for all sorts of diseases.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks