Humans placed in ‘suspended animation’ for first time, US doctors announce
‘We’re not trying to send people off to Saturn,’ says leader of medical research team behind potentially life-saving procedure
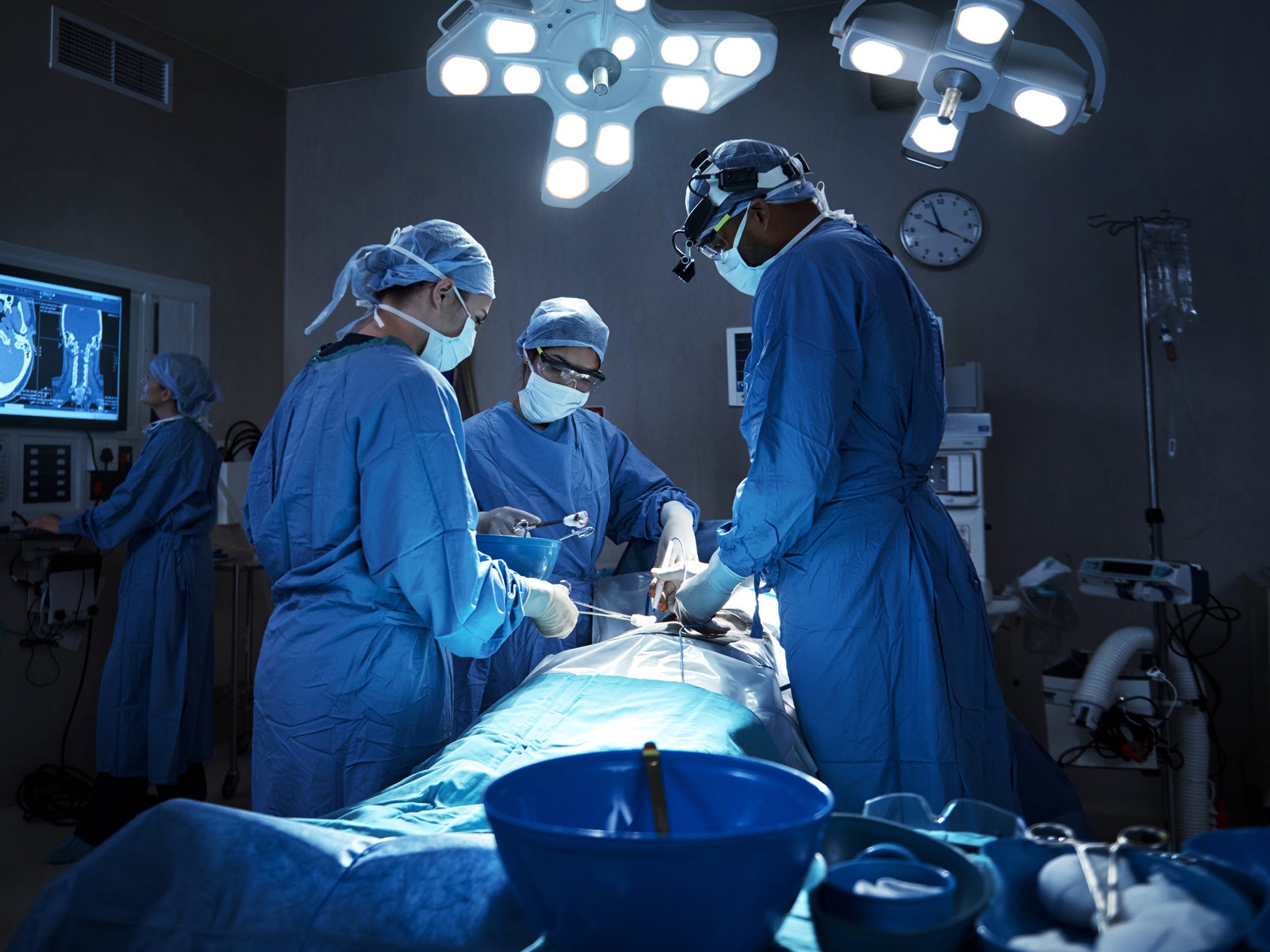
US doctors have placed live human patients in suspended animation for the first time, in trials designed to allow surgeons greater opportunity to carry out life-saving operations.
“At least one person” has undergone the technique – which involves replacing their blood with cold saline fluid for up to two hours, before their hearts are restarted – but doctors have yet to reveal whether it has been fully successful.
Dr Samuel Tisherman, who is leading the trial at the University of Maryland Medical Centre in Baltimore, told the New Scientist that the first time they placed a patient in suspended animation it was “a little surreal”.
The patients are not voluntarily taking part in the trial, but are given the treatment after arriving at the hospital in a critical condition – typically from gunshot wounds or stab wounds to the chest.
Only when traditional efforts to save their lives, such as blood transfusion or opening the chest cavity for surgery, are proving fruitless do the team put them into suspended animation to buy more time.
By this point, the patient’s heart is likely to have stopped beating, and they will already have lost a significant amount of blood. Emergency surgeons may only have minutes to work, and the chance of survival is normally around 5 per cent.
The patient’s blood is flushed out of their system by freezing saline fluid pumped via cannula directly into the aorta. This rapidly cools the vital organs – particularly the brain and the heart.
Once the brain temperature falls to 10-15C, the saline solution pump is switched off, and surgeons have up to two hours to perform essential surgery, while a heart and lung machine keeps the patient alive.
Blood is then returned to the body, and the heart restarted. If enough of a pulse is detected, the patient can be moved off the heart and lung machine and moved to intensive care for recovery.
The technique works mainly through lowering the body temperature, reducing cells’ demand for oxygen. At normal body temperature, around 37C, the demand for oxygen is very high. Panic and stress, such as in the case of a traumatic injury, can also trigger even higher demands on the heart and blood supply.
But as the body enters a hypothermic state, the activity in all cells is rapidly reduced, lowering the demands.
In a Ted talk last year, Dr Tisherman compared the technique to incidents when people have survived cold water drowning, even in some cases being submerged for up to an hour, due to their organs’ reduced demand for oxygen.
“You’re under water, you can’t breathe, but your body cools fast enough that your brain, your heart, your other organs are protected, and you can actually survive for an hour,” he said.
However, inducing hypothermia externally has major risks, such as reducing the clotting of the blood, as well as shivering and stress.
The new technique aims to reproduce the benefits of being chilled, but in a controlled environment.
While suspended animation has long been the preserve of science fiction, allowing characters to travel for years into space while their body is kept in stasis, Dr Tisherman says that is not the aim here.
“I want to make clear that we’re not trying to send people off to Saturn,” he told the New Scientist. “We’re trying to buy ourselves more time to save lives.”
He presented the findings of the investigation, which is due to be completed by the end of next year, at a symposium at the New York Academy of Sciences.
Ultimately the study hopes to compare 10 patients who were given the experimental treatment with 10 for whom the same criteria applied but were unable to undergo the process because all the large team required were not in the hospital at the same time.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks