Africa's new affordable HIV treatment deal under threat from US budget cuts
A drug widely available in the west is finally affordable for African nations, but Donald Trump's budget cuts threaten that progress
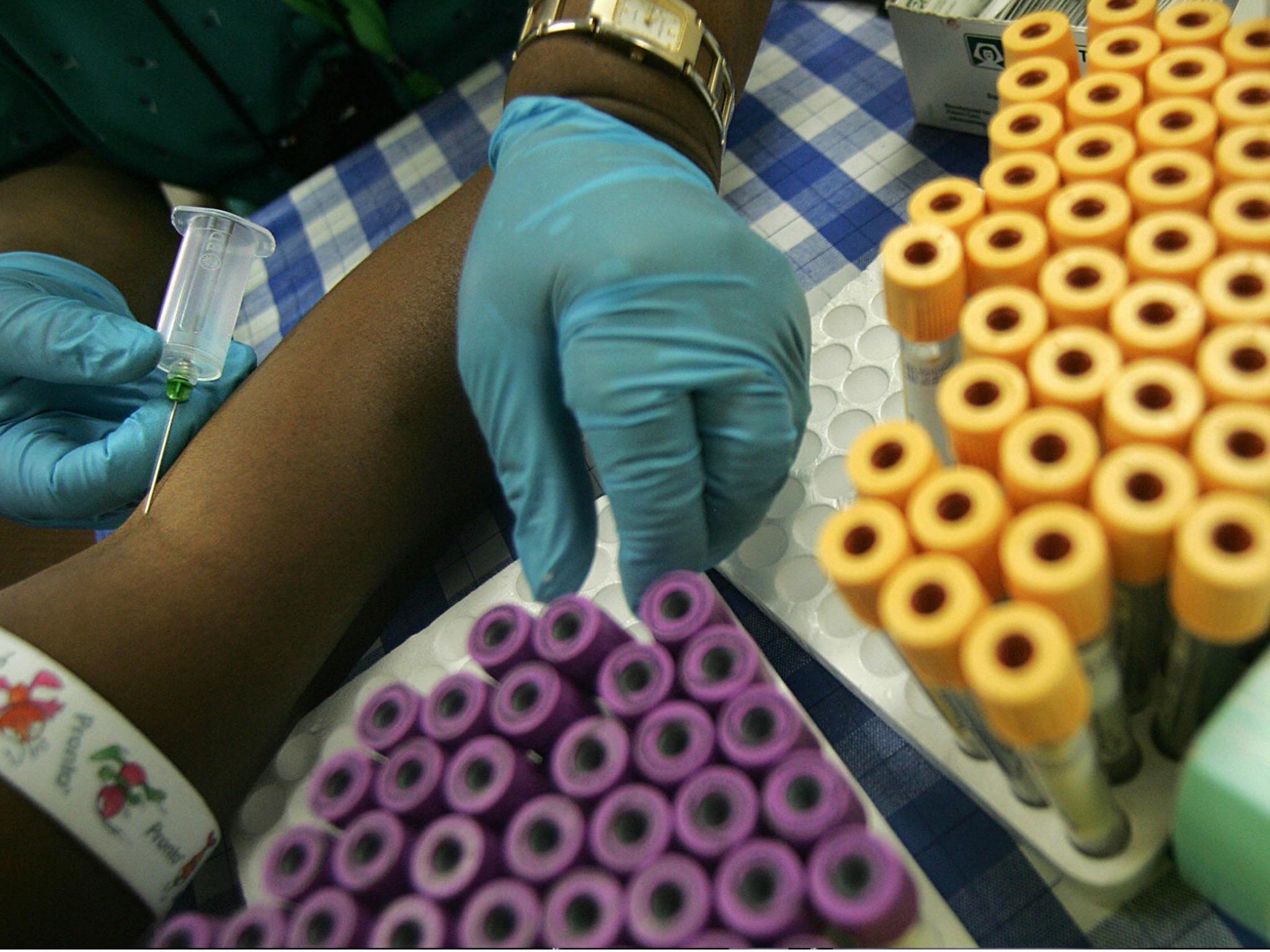
A “best in class” HIV/Aids treatment drug will now be be more affordable to African nations, but proposed budget cuts by the US could make ending the epidemic difficult.
A new pricing partnership has been struck between the UN, African nation governments such as South Africa and Kenya, the pharmaceutical industry, and the US President’s Emergency Plan for Aids Relief (PEPFAR) to drastically reduce the price of a crucial HIV/Aids treatment drug.
The cost for treatment has now been set at around $75 per person per year in over 90 low to middle-income countries. The treatment cost was previously upwards of a $1,000.
The drug in question contains dolutegravir (DTG), which has been billed by the Joint United Nations Programme on HIV/Aids (UNAIDS) as the “first affordable, generic, single-pill HIV treatment regimen” that will be available to public purchasers.
The once a day, one pill treatment is also the preferred treatment option by the US Department of Health and Human Services as well as the World Health Organisation.
The drug, which is actually a combination of tenofovir disoproxil fumarate, lamivudine, and dolutegravir (TLD), was developed by two pharmacies: Mylan and Aurobindo Pharmaceuticals.
They have licensing agreements from ViiV Healthcare, the original developer of DTG.
Dr Larkin Callaghan, Director of Strategic Communications and Partnerships at the Aids Research Institute at the University of California - San Francisco, told The Independent that DTG is a “best in class integrase inhibitor”.
Dame Sally Davies, the Chief Medical Officer for the UK, said DTG is known to fight a growing problem with HIV/Aids treatments in sub-Saharan Africa - resistance to the disease.
Speaking during a news conference on Thursday, Ms Davies said the drug also produced significantly fewer side effects for patients, which encouraged continued use of the drug and thus prolonged life.
Dr Mike Reid, a Clinical Fellow at the University of California-San Francisco Hospital said DTG is not a new drug.
In fact, he uses DTG in his California practise. However, this is the first time the drug will be made affordable to over 90 lower and middle-income countries.
“DTG is so much more potent than any other drugs used in sub-Saharan Africa,” Mr Reid said.
He also said that the drug is good for patients who have never been anti-retroviral drug treatments (ARVs) as well, making it accessible to a larger pool of infected people.
While the number of Aids-related deaths have fallen by 42 per cent in eastern and southern Africa since 2010, South African Minister of Health Aaron Motsoaledi pointed out that his country still has about seven million people living with either HIV or Aids.
In 2016, there were 19.4m people in eastern and southern Africa living with HIV, with women and girls making up nearly 60 per cent of that population.

These parts of Africa also account for approximately 43 per cent of new HIV infections, or nearly 800,000 new cases in last year.
Over a quarter of those were in South Africa.
Mr Motsoaledi said the majority of people infected in South Africa are receiving help from government sources, with only about a quarter million able to afford private care.
With the new pricing agreement, combined with the effectiveness of DTG however, he said that the burden on the state is dramatically reduced.
Over the next six years, the government will save approximately $900m according to Mr Motsoaledi.
“We can now treat more people with the same amount of money,” he said, adding that without the new pricing agreement his government would need an additional $900m to treat an increasing number of infected people by 2022.
Lelio Marmora is the Executive Director of Unitaid, a UN global health initiative that works to invest in better prevention and treatments of pandemics like HIV/Aids.
He said that one of the biggest problems African leaders who come to his organisation have is “increasing the fiscal space and investments available for health.”
Pilot programmes or small public initiatives have been run in the past, but to have a lasting impact on an entire population, programmes will need to reach a wide swathe of people being serviced by the governments.
Also, companies like Viiv, Mylan, and Aurobindo cannot reduce prices of drugs, even generic versions of them, if the number of patients cannot be accurately forecast and market conditions in these countries cannot be accurately predicted, Mr Marmora explained.
The new pricing deal announced at the UN is groundbreaking because it serves to address this problem of “scaling up” in sub-Saharan African disease treatment and provides a stable market for the pharmaceutical industry.
The “industry is an ally” Mr Marmora said, as he noted there are several successful private-public partnerships in global health.
“Access, access, access,” is at the centre of the deal according to Dr Michel Sidibe, Executive Director, UNAIDS.
In 2000, South Africa only had about 90,000 people on HIV/Aids treatment. That number is up to four million now according to Mr Sidibe and will likely increase with the pricing agreement.
However, that “access” is under threat.
US President Donald Trump has threatened to cut what is arguably the most successful American global health programme, the Presidential Emergency Plan on AIDS Relief (PEPFAR).
Mr Trump’s proposed budget cut would reduce US contributions to the programme by 17 per cent from $4.6 billion in the current budget to $3.8bn.
As has become a common justification for budget cuts and increasing isolationism from multilateral organisations, the Trump administration said the cuts would be made to reduce American burden and "with the expectation that other donors can and should increase their commitments to these causes."
Mr Sidibe said the cut could be “a major setback” in the effort to end the HIV/Aids epidemic in the region.
“It would be catastrophic” to South Africa, said Mr Motsoalebi.
Ms Callaghan said that the DTG pricing deal “is a multilateral partnership with six high-level partners is really encouraging, and should underscore the need for PEPFAR to remain fully funded.”
PEPFAR makes up two-thirds of the US global health budget, but Ms Callaghan argues it has continued to get funding since its inception under President George W Bush “because it’s working”.
The programme provided ARVs on the continent to 11 million people in 2016 alone.
Part of the reason PEPFAR works is because of its sustained financing.
Keeping people on drug treatments is key, as infection rates increase when people go off of them.
That the new deal provides a drug with fewer side effects that is less resistant to HIV is crucial but without the distribution and administrative structure as well as expertise of PEPFAR, the deal would not have nearly the positive impact it could.
“So at a period of time when we are making huge progress in many developing country contexts, to yank the very reason why is just incredibly short sighted,” said Ms Callaghan.
The Trump administration’s thought that the gap in the US budget cut could be filled by other countries is worrying to many experts and the elephant in the room today as a panel discussed the new DTG pricing deal.
Mr Sidibe praised the “generosity of the American people” in funding so much of global health efforts, but groups like the Bill and Melinda Gates Foundation and the Clinton Health Access Initiative can only make up so much for the American government funding.
Ms Callaghan noted “Aids-related illnesses are still the leading cause of death for women [aged] 15-49 globally. when you look at that it seems really hard to justify to me why you would cut the funding that is working towards changing that statistic.”
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks