Patient who received groundbreaking pig heart transplant was jailed for stabbing man and leaving him paralysed
In medical circles, its usually considered unethical to base care off a previous criminal record
A first-of-its kind transplant involving a genetically modified pig heart is raising ethical questions, after it was revealed that the patient who received the surgery had previously stabbed a man repeatedly and left him paralysed.
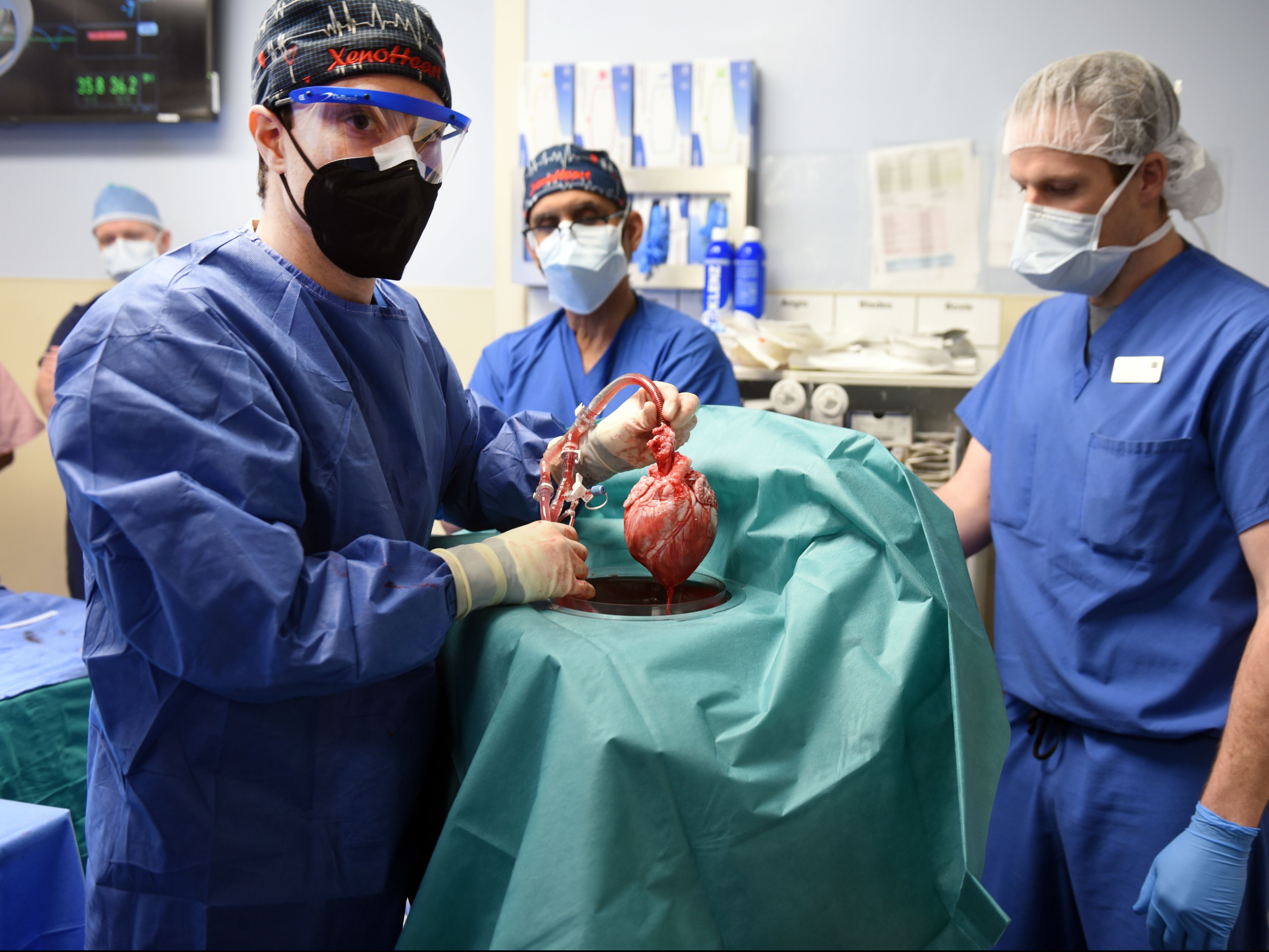
David Bennett Sr, 57, made headlines around the world earlier this week, when it was announced he was safely recovering from the world’s first successful GMO pig heart transplant at the University of Maryland Medical Center.
Doctors at the university heralded the procedure as an important step in helping the more than 110,000 people each year on organ transplant lists get help sooner – where many die before they can get a surgery.
“This was a breakthrough surgery and brings us one step closer to solving the organ shortage crisis. There are simply not enough donor human hearts available to meet the long list of potential recipients,” Dr Bartley P Griffith, who performed the surgery, said in a statement.
The news had a decidedly different feeling for Leslie Shumaker Downer, whose brother Mr Bennett stabbed and paralysed in an attack at a bar in Maryland in 1988. She told The Washington Post, which uncovered the past conviction, that she recognised the significance of the heart transplant, but didn’t view Mr Bennett as a hero.
“Ed suffered,” Ms Downey, told the Post. “The devastation and the trauma, for years and years, that my family had to deal with…Now [David Bennett] gets a second chance with a new heart — but I wish, in my opinion, it had gone to a deserving recipient.”
On 30 April, 1988, Mr Bennett stabbed Ed seven times at a bar in Hagerstown, Maryland, reportedly after seeing Mr Shumaker flirting with his wife. He was convicted and sentenced to 10 years in prison, and was separately ordered to pay the Shumaker family $3.4m in a civil suit, which they claimed to have never received. Edward Shumaker was in a wheelchair for the next two decades, before having a stroke in 2005 and dying two years later. Meanwhile, the rest of the family struggled alongside him, taking out loans to pay for a wheelchair-accessible van. Ed’s brother, an EMT, who had dropped him off at the bar the day of the attack and was later called to respond to the bloody scene, struggled with guilt and later became addicted to opioids, before dying in 1999 of an overdose at the age of 28, according to his family.
UMD said in a statement that it provides “lifesaving care to every patient who comes through their doors based on their medical needs, not their background or life circumstances…This patient came to us in dire need, and a decision was made about his transplant eligibility based solely on his medical records.”
In most medical circles, it’s considered unethical to deny someone medical care based on their past criminal record.
“Punitive attitudes that completely exclude those convicted of crimes from receiving medical treatment, including an organ transplant are not ethically legitimate,” wrote an ethics panel in 2015 for the federal Health Resources and Services Administration, adding, “Criminals not sentenced to death are expected to return to society and be deemed worthy of equal treatment in the receipt of other items/services distributed by society.”
Mr Bennett was denied transplant eligibility at previous hospitals for medical and non-medical reasons. His past record of heart failure and irregular heartbeat made him ineligible for some transplants, as had his past record of failing to follow doctor’s orders, attend follow-up visits, or take medicine consistently, according to his son.
David Bennett Jr, Mr Bennett’s son, said his father never spoke of his past, and lauded him for taking a risky chance that might help benefit medical science. This winter, facing his potential death at a Baltimore hospital, David, Sr, reportedly began inquiring about being an organ donor or other ways to benefit science if he passed away from his heart condition.
“My intent here is not to speak about my father’s past. My intent is to focus on the groundbreaking surgery and my father’s wish to contribute to the science and potentially save patient lives in the future,” David Bennett, Jr, said in a statement.
Roughly 17 people die each day while waiting for an organ transplant.


