The deadly Covid cocktail that pushed an opioid crisis into overdrive
When coronavirus hit West Virginia, it collided with a raging drugs epidemic – and overdoses surged. Richard Hall reports from the towns where measures to stop the virus had lethal consequences for addicts

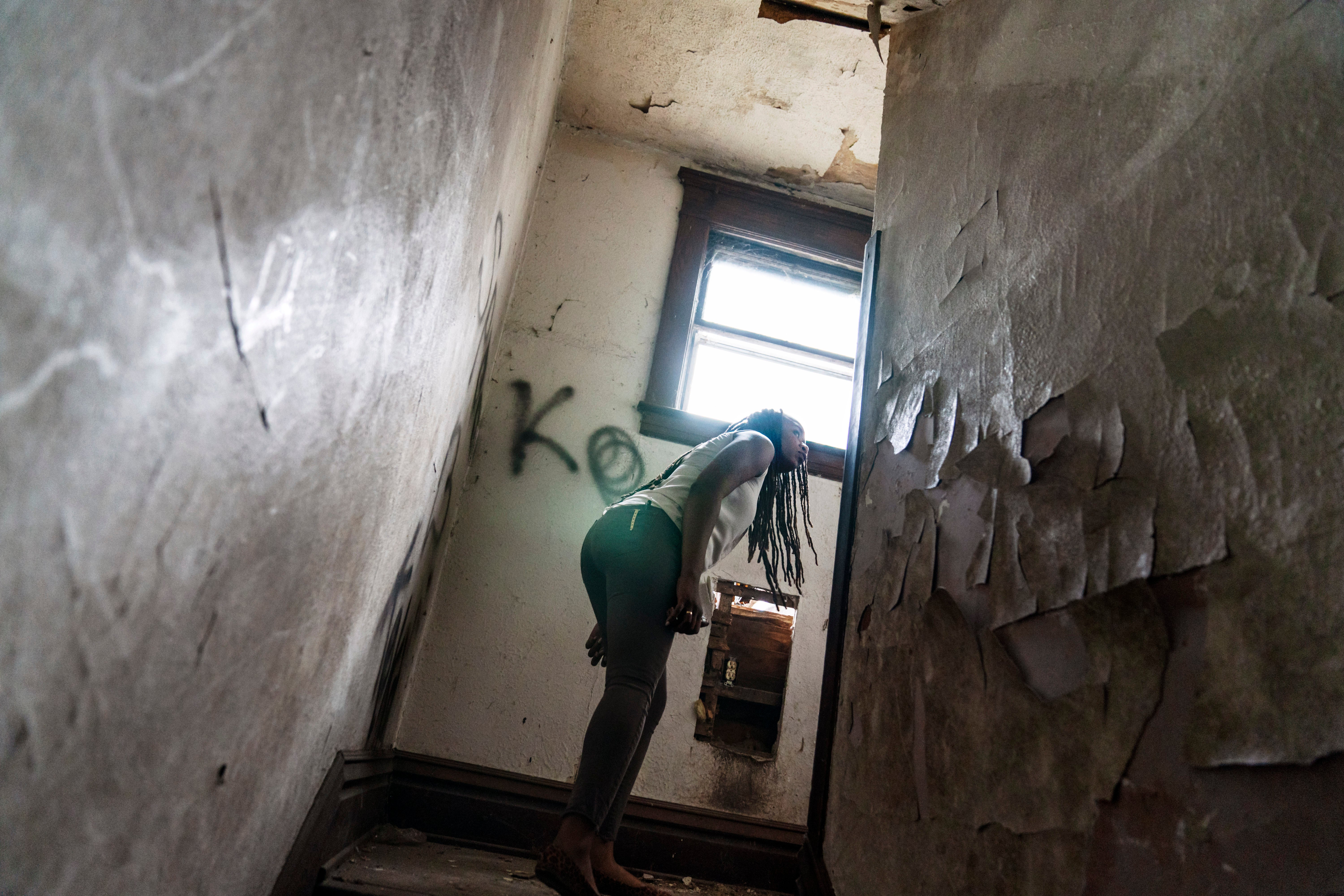
Natasha Robinson vividly remembers the day her first stimulus cheque came through. She was homeless and in the depths of heroin addiction at the time. Most of her days were spent scrambling to find enough money to get a fix. This day was different.
“The first thing I did is I went to the ATM down here. The second thing I did is I went to my dealer’s house, and it wasn’t not even 10 minutes after that my husband was dead on the floor,” the 26-year-old says, pointing to the spot where he overdosed in the back room of this small church building in West Virginia.
“That first cheque was gone in two days. It was just bad. So many people that I know overdosed, some people died. It was probably about the worst thing for people in addiction.”
There was a grim irony in what happened to Natasha, and she was not alone. The Covid stimulus cheques distributed from April last year – $1,200 for most American adults – were a lifeline to millions around the country, but a potential death sentence to those in addiction.
It was just one of the many ways in which public health measures put in place across the US to stop the spread of coronavirus had unintended, adverse effects on communities that were already battling a deadly opioid epidemic. It forced people on the front line of that crisis to make impossible choices about which of the two to fight at any one time.
Here in West Virginia, the consequences were fatal. The state, one of the worst-affected by the nationwide crisis, had been making progress: five consecutive years of rising overdose deaths had given way to two of slight decline. There was still a long road ahead, but there was a sense that things might be about to turn a corner. Then, it all fell apart.
Last year, as much of the country was shut down to stop the spread of the virus, fatal overdoses in the state rose by 47 per cent to a record high. At least 1,291 people died from drug overdoses in West Virginia in 2020, up from 877 in 2019, and 909 in 2018. Nationwide, more than 90,000 people are thought to have died from overdoses in 2020, up about 30 per cent on the year before.
‘The worst thing that could possibly happen’
Those numbers are no surprise to Natasha and others struggling with addiction. Her husband would have been among them had she not revived him on the floor of the church room where she now sits. Surrounded by a circle of chairs scattered around the room at a recovery meeting held by a local pastor, she tells the story of her addiction. It began from a young age.
“Drugs and alcohol was part of my life [for] my whole life,” she says.
Her addiction followed a path familiar to many, driven largely by what was available: weed at 14, prescription opioids at 15, then a transition to heroin. Three or four years into her heroin addiction things really began to fall apart. She was living on the streets and her child was taken away. She went into rehab soon after.
Natasha had seen it all, but even for experienced addicts the impact of Covid-19 was a jolt to the system. She and other addicts talk of the early days of the pandemic like veterans talk of a vicious battle in a war gone by.
“Oh my goodness, that Covid,” she says with a deep breath. “When that hit, that was the worst thing that could possibly happen to me.”
The stimulus payments, she says, were the spark.

“It was probably about the worst thing for people even in recovery, let alone people in active addiction. The first thing they’re going to do is they’re going to run and get their fix. You cannot give them that kind of money. You can’t give 20 bucks to an addict.”
Joni Adkins, 25, sitting across the room, nods in agreement. “I overdosed on my first stimulus cheque,” she says. “I went wild with that one. I blew it in a week and that was the most heroin I’ve ever done in my life.”
People working on the front line saw the impact immediately. Amanda Coleman runs a homeless shelter in the centre of Huntington, a city that has borne the brunt of West Virginia’s opioid crisis. Sitting in the courtyard of an apartment block run by the charity, she explains that restrictions on social security payments that were put in place to protect people suffering from addiction broke down during the pandemic.
“Each month we pay their rent, we pay their bills and then we give them a weekly cheque for living expenses or personal expenses,” she says of the programme. “With the stimulus, we were required to just give it to them all at once.”
The shelter came up with a novel solution to deal with the inevitable overdoses that would follow.
“We were handing them Naloxone with their cheques,” she says, referring to the medication that revives someone who has overdosed.
All it takes is one bad day, one thought and you acting on that thought will mess up your whole life
“We would try not to be offensive. Most of our folks are just open with us because they’re not going to get any judgment from us about it. But some like to pretend that they don’t and we’d say, ‘Well, in case your friend goes down, you know, go ahead and take it.’”
The spike in overdoses was impossible to ignore, however. Coleman says it was around early summer that things got really bad.
“It was overdoses in our shelter, down the block. People would come running from two blocks away to ask for help. It was people coming in and saying, ‘I ODed three times this weekend’, or, ‘My friend ODed.’” she says.
The chaotic bursts that followed the stimulus payments were followed by another problem that would be harder to shake. Those who made it through the early days of the pandemic without relapsing faced another challenge to their recovery: isolation.
Pandemic lockdowns, lifesaving for the wider population and essential for stopping the spread of the virus, created the perfect conditions for addicts to fall through the gaps. Quarantines tore them away from support systems and the help they needed. Natasha experienced it at first hand.
“When you’re isolated, all of your thoughts come back,” she says. “I don’t care how far you got in recovery – I don’t care if you got two months or 10 years, all it takes is one bad day, one thought and you acting on that thought will mess up your whole life. And for people to be isolated, and then given a big bunch of money, that’s just asking for death.”
‘The devil’s playground’
An hour’s drive east from East Lynn, along winding roads through the countryside, lies Madison. This town of fewer than 3,000 residents thrived when the region’s coalmines were busy. Like much of rural West Virginia, it suffered greatly when the industry declined. Jobs left, then people followed.
The aggressive marketing and delivery of millions of prescription pain pills, from early in the millennium onwards, into an area that was suffering economically was a death blow. Addiction soared and places such as Madison became regular features on nightly news programmes about the crisis. America was used to seeing drugs in the city, but not in small towns like this.
The opioid crisis hit rural communities like East Lynn and Madison just as badly as it did urban areas. At its height, one small drive-in pharmacy here distributed more than 9.6 million doses of prescription opioids hydrocodone and oxycodone, according to a lawsuit filed against the owners. Today, that small pharmacy is boarded up and closed, like many other businesses in the town.
Around 2012, opioid manufacturers were curtailed by regulations that reined in prescription abuse. That led addicts to turn to whatever drugs were available – mostly heroin and fentanyl. Those drugs are responsible for the majority of overdoses today.
Chelsea Carter grew up here. She was once an addict, but for the past 12 years she has been in recovery, and today works at a rehabilitation clinic helping others overcome their addictions.
The Brighter Futures clinic had just opened in January last year with funding from the nearby Boone County Memorial Hospital. Before, people would have to travel for 10 or 20 miles to receive treatment. The clinic aimed to reduce the distance between people in recovery and their treatment. As any rehabilitation counsellor will tell you, regular contact is essential. When that was taken away during the pandemic, it had a devastating effect.

“We’re not only dealing with addiction, we’re dealing with the mental health side,” says Carter, in an office on the fourth floor of a building on Madison’s high street.
“The thing about addiction is that your brain is like the devil’s playground. When you’re alone, all you do is sit and think. And you start migrating back towards using because you think, ‘At least I won’t be stuck in my head all the time.
“Our patients have been introduced to a way of treatment – they come in here and we hold them accountable and they have drug screening and all this stuff. Then when the pandemic started we just had to say, ‘We’ll call you on a phone, but I want you to stay clean.’ They were left to their own devices.”
Some went to great lengths to keep the meetings going. In the winter, when Covid was raging and everyone was shut down again, one person told The Independent they arranged a meeting for 70 people out in a field. They collected wood, built a giant bonfire, and shared their stories as they usually did.
Some clinics even turned to telemedicine to continue treatment programmes, keeping in touch with their patients over video calls. But that, too, has drawbacks.
Now it’s nothing to hear two, three, four people a day overdosing, and sometimes on even larger scales than that
“It’s easy for me to lie to you if you’re on a computer screen. I can look at you and not be able to tell you’re high,” she says. “Now, if you’re in front of me, I can tell if you’ve taken something,” Carter says.
Brent Tomblin, the Brighter Futures clinic’s executive director, says telemedicine has further difficulties in a poor, rural town like Madison.
“Our population here, many haven’t worked in years,” he says. “We don’t have a lot of money. If we do have money, it’s going to go toward our addiction. So I don’t have a cell phone. If I have a cell phone it’s more of a flip phone or something that doesn’t have a lot of minutes on it. I don’t have a computer. I don’t have a home. I don’t have internet. Maybe I live with my cousin or somebody and they’re low-income too. They can’t afford to do all that kind of stuff.”
So they decided to stay open, while following the public health guidelines such as social distancing and limits on the number of people in a room.
“We still allowed our patients to come in because we thought that was the most effective treatment,” says Tomblin. “And we know we never closed our doors at all, but for a couple days just trying to figure it out.”
Read more special reports from our Supporter Programme
Elsewhere, though, this break-off from treatment sparked a deadly chain of events. The increased isolation made people more likely to relapse and overdose, and those overdoses became more deadly because there was no one around to revive the victim. Treating an overdose victim is a relatively simple but lifesaving process that most people are able to do. It involves administering Naloxone, a drug known by its brand name Narcan.
“What’s happened now is all these people are using alone and at home. Nobody’s there to Narcan you, to call 911 when they overdose. So we have people dying at big rates,” Carter says.
“Now it’s nothing to hear two, three, four people a day overdosing, and sometimes on even larger scales than that. It just depends on what’s going around.”
‘I didn’t have any connection to the outside world’
After surviving the chaos of the early days of the pandemic, there was time for more ironies to befall Natasha and Joni. This time it was the good kind. In the most difficult circumstances, when their friends and acquaintances were falling around them, when they could have easily fallen through the gaps again, they managed to get clean and stay clean.
Joni says she had managed to keep her addiction a secret from her family until the overdose following the first stimulus cheque.
“I don’t think it was until after I was revived with Naloxone and I came back that I was really like, ‘Wow, maybe I’m not as suicidal as I think, because that was scary.’”
She became fearful that child-protection services would take away her infant, so resolved to get clean. She entered rehab just as lockdowns went into place.
“I didn’t have my cell phone. I didn’t have any connection to the outside world. We were in Covid shutdown so we didn’t leave the building at all,” she says.
“So as soon as I got out, I jumped right back into being a full-time mom.”
Natasha got clean after a decade of addiction, the only person in her family to do so. It was a six-month stay in rehab, her second attempt, that did it.
“That was probably about the best thing that ever happened to me,” she says.
“At that point in my life, I was homeless living in Huntington and was robbing and stealing and breaking into places. I even came back out here. I broke into this church several times. I weighed 85 pounds. I’ve done it all. If I hadn’t been sentenced, I wouldn’t have stopped and I would have ended up killing myself.”

Bookmark popover
Removed from bookmarks