Some mental health services are telling patients: ‘If you really wanted to kill yourself, you would have done it’
When people do get to access crisis care, many feel that the emphasis is on getting rid of them as quickly as possible. Psychiatric inpatients have even been told to phone the Samaritans if they wish to talk
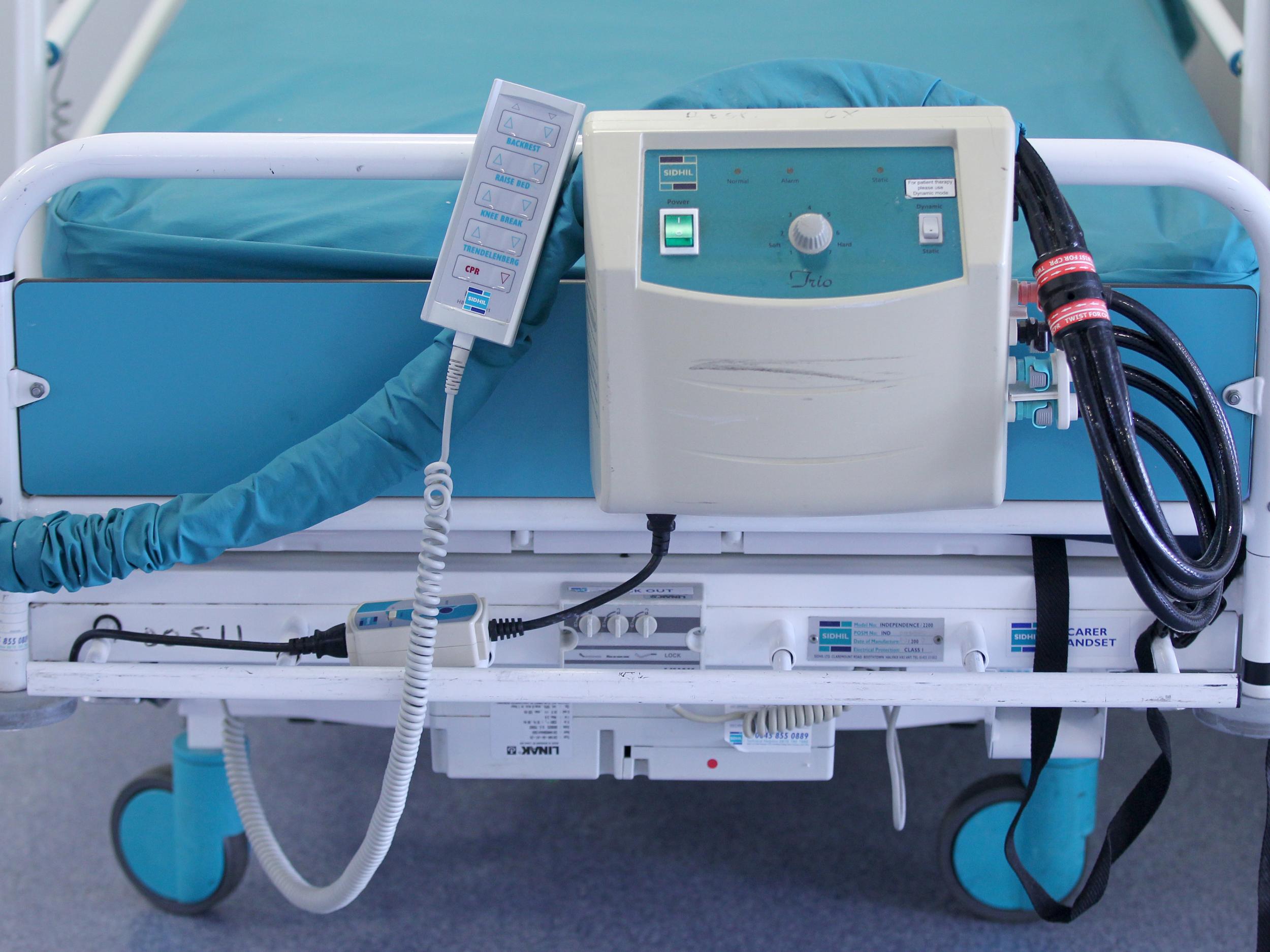
People are encouraged to seek help if they are feeling suicidal like never before. Yet a deadly new mix of funding cuts and dangerous ideas about suicide are leaving many people with long-term conditions at greater risk.
Tom is 22 and has made a couple of serious attempts on his life following prolonged periods of depression. “When I regained consciousness after the last attempt”, he said, “I was told ‘If you really want to kill yourself, you would have done it’.” Tom, like many other people, feels like when he now contacts the crisis team, they treat him brusquely. “It is like they will only take me seriously if I actually die”, he continued. “I am told again and again ‘well if you really want to kill yourself, that’s your choice’.”
We are not talking about nuanced Schopenhauerian conversations about the right to die here. In the context of deep despair, the idea of choice is a deadly one, absolving the other party from doing everything they can to help the person in pain. If one is suicidal it is very difficult to feel any hope that things might change; one is often exhausted. It is crucial that hope is held actively by mental health professionals at these bleakest moments in a life.
Yet the idea of choice is being used increasingly to rebuff those who seek help when suicidal, a discursive move that an increasingly burnout mental health workforce appears to be using more often. This makes those suffering feel rejected and further alienated – key trigger factors to suicide.
Laura, 60, has also made multiple attempts on her life. She has been told that she should “take responsibility” when she is feeling suicidal, an idea fuelled by the neoliberal discourse of rights and responsibilities which has taken hold of mental health services. “There is a strict management plan and boundaries in place”, she said. “I am allowed to call the crisis team three times a week, and the calls are time-limited. When I do call, I am only allowed to talk about the present not the past”, she says. “If I try to talk about anything else, or call at another time, I am told I am ‘threatening suicide’.”
The approach to suicide prevention Laura is receiving is based on a behavioural “carrot and stick” approach to mental health. The idea is to shape behaviours into ones which are healthier in the medium term by positively reinforcing only “healthy” boundaried behaviours, though distress can increase in the short term. This kind of approach is very dangerous if it is transmitted in a judgmental, blaming way; it should only ever be attempted slowly in collaboration with patients with the explicit recognition that change is incredibly hard, and that patterns of behaviour in the face of overwhelming distress have developed for an understandable reason.
Yet these are now being used by undertrained staff, without the consent or understanding of patients, and without giving people access to the kind of long-term therapy so essential to working through the experiences behind the pain. This is actively re-traumatising patients.
“They treat me like a bad person, who doesn’t deserve care and support” says Laura, who has been treated abusively throughout her life.

Laura has a diagnosis called “borderline personality disorder” – a diagnosis that lacks scientific validity and is steeped in misogyny. This diagnosis demonstrably makes professionals more likely to treat patients with distance, fear and sometimes disdain – the feelings of rejection are not simply a result of projection. Like many others, Laura is made to feel like she is “attention seeking” and “manipulative” when she is suicidal or makes attempts on her life. “I don’t do this for fun,” Laura said of her recent suicide attempt, “I do it when there is nothing else left”.
Roger, 34, has also been told the decision to end his life is his because he is deemed to have something called mental capacity. Mental capacity, simply, is the ability to weigh up information and make decisions, something that fluctuates in the throes of a mental health crisis. Mental capacity should never be used to justify withholding treatment from someone seeking help. But mental health services, desperately underfunded, seem to be using ever more drastic means to buffer increasing demand. “I am desperate for help” said Roger, “and my GP keeps writing to mental health services, but the letters get returned unanswered.”
When people are finally able to access crisis care, many feel that the emphasis is on getting rid of them as quickly as possible. “They tell me to distract myself, or take a bath, or go for a walk when I am feeling suicidal, when what I actually need is a few kind words and some compassion”, one service user reported. Psychiatric inpatients have even been told to phone the Samaritans if they wish to talk.
I am writing this article in awareness that most mental health services do a fantastic job, and with the wish that people continue to seek help. I cannot emphasise enough how many people I have met who have made multiple attempts on their life, often over many decades, and come to thrive.
But I write too with a desperate request that we not only fund crisis services better, that we not only skill mental health staff to be able to contain suicidal despair, but that we change attitudes around suicide within psychiatric services which block people from care. It is inexcusable that mental health services make people feel like a burden for continuing to struggle, that we take away from them the possibility of help and therefore hope.
In memory of JL
Dr Jay Watts is a consultant clinical psychologist and psychotherapist, and honorary senior research fellow at Queen Mary, University of London
If you have been affected by this article, you can contact the following organisations for support:
https://www.mind.org.uk/
https://www.beateatingdisorders.org.uk/
http://www.nhs.uk/livewell/mentalhealth
https://www.mentalhealth.org.uk/
https://www.samaritans.org/
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks